Discount albenza 400mg
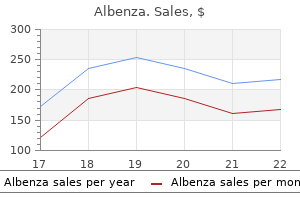
However medicine 7253 pill purchase genuine albenza, the threshold by which we measure the efficacy of these procedures should be tailored to the benefit/risk profile and the overall intent of the therapy. Based on the intent of therapy, safety and efficacy are evaluated in conjunction with repeatability, durability, and permanent or nonpermanent alteration of the anatomy [6]. This treatment modality can be considered in morbidly obese patients as an alternative to conventional procedures and treatments. The resulting excess weight loss should be comparable to a bariatric operation with a similar risk profile. This therapy will also need to have a significant long-lasting effect as seen with a surgical intervention. It may be permanent or require repeatability if the durability of the effect is of shorter time period. Modest weight loss (~5 %) in these patients has shown a significant improvement in cardiovascular risk factors [12]. Procedures used in this patient population should have a lower risk profile and higher durability (or repeatability) than therapies intended for greater weight loss. Weight regain or weight recidivism has been cited as the most common indication for revision [5]. A number of endoluminal platforms will provide the tools necessary to perform stoma and pouch reduction after gastric bypass and modifications after other bariatric procedures. It is important to understand the limitations of many of these studies including small numbers, no comparators in many, and short-term follow-up. However, at the same time it is important to evaluate these modalities for their technical feasibility and benefit/risk profile. As in any technology, there will continue to be refinements that will allow for greater technical feasibility and potentially a more favorable benefit/risk profile, greater durability, and potential for repeatability. Early Intervention/Preemptive Therapy the goal of early intervention/preemptive therapy is to achieve weight loss in potentially class I obese patients who are at risk of disease development or disease progression. The evidence to support this concept of treatment comes from prospective studies demonstrating significant weight loss and improvement/resolution of weight-related comorbidities in class I obese patients undergoing bariatric surgery. Endoluminal Techniques Altering Gastric Capacity Limiting the functional capacity of the stomach has been the goal for a wide variety of bariatric procedures. This has been demonstrated in multiple surgical subspecialties including bariatric, 40 Experimental Alternatives in Bariatric Surgery 449 gastric plication. These techniques vary from endoscopic suturing and stapling platforms to space occupying devices. Endoscopic suturing and stapling platforms have been used to create a vertical gastroplasty. The first reported series of endoluminal vertical gastroplasty in managing obesity was reported in 64 patients. This study recreated the anatomy of a dilated pouch with an enlarged stoma in a porcine model. The concept of placing an intragastric balloon to restrict oral intake dates back to the mid-1980s. The individual dual-balloon technology prevents unwanted migration in case of deflation of one of the balloons. Metabolic Endoluminal Procedures Endoluminal devices are also being designed to have more of a metabolic effect similar to bariatric or metabolic surgeries. Strategies will focus on achieving modulation of gut hormones and the amount of interaction of chyme with the intestinal tract. Seventeen of the 22 patients were able to maintain the device for the complete 12-week trial. The authors also reported effective glycemic control without medication in seven diabetic patients [23]. The first feasibility study was carried out in 12 patients where the device was used to enhance preoperative weight loss. More recent studies have compared the duodenojejunal bypass sleeve to low-calorie diet or sham controls and showed a significant difference in weight loss favoring the bypass sleeve [25, 26]. Other strategies have focused on recreating the anatomy of a Roux-en-Y gastric bypass. This communication will then mature after a few days to become an anastomosis [27]. Innovative Surgical Techniques the evolution of minimally invasive techniques have shifted the practice of bariatric surgery and fueled the evolution of newer therapies. The current practice of weight loss operations involves division and anastomosis of gastrointestinal structures, gastric resection or plication, or implantation of medical devices. Others have focused on reproducing the effects of currently accepted bariatric operations without the undesirable morbidity or commitment to irreversible operations. As our understanding of the neurohormonal functions of the gastrointestinal tract continues to evolve, newer procedures will continue to emerge. They should be evaluated on the intent of therapy, benefit/risk profile, durability, and the potential to be revised. Combining the adjustable gastric band and gastric plication procedures limits some of the advantages that triggered the development of gastric plication, such as lack of a foreign body and potential reversibility [33]. They encourage the performance of this operation under third-party oversight as well as publication of transparent results [30]. Ileal Interposition and Digestive Adaptation Different theories have been proposed to explain the obesity epidemic. One of these theories focuses on the difference between the primitive and modern human diet. In the modern human diet, we ingest more refined nutrients with less fiber and residues that can be efficiently absorbed in the proximal small bowel [34]. The operation consists of a sleeve gastrectomy, omentectomy, and resection of proximal small bowel shortening the entire length to 3 m. In theory, this length of bowel is sufficient for efficient nutrient absorption based on a modern diet [34]. More recent studies have developed animal models to better understand the physiologic implications of such a procedure [36]. This operation introduces the concept of "ileal brake" by which undigested nutrients reach the ileum, triggering a hormonal response that increases satiety and improves glycemic control. It has been recently used in combination with sleeve gastrectomy to accentuate the metabolic response. In theory, this operation avoids the risk of malabsorption and eliminates the need for vitamin and mineral supplementation required in gastric bypass patients [37]. Gastric Plication and Laparoscopic Adjustable Gastric Banded Plication Many different types of gastric altering procedures have been developed and described throughout the years. More recently, sleeve gastrectomy has gained popularity among surgeons and patients. The gastric plication attempts to reproduce the gastric restrictive effect of the sleeve, without resection of the stomach. Variations of the technique have been described since its introduction in 2007 [28]. Greater curvature plication has been the most widely practiced technique in the past few years. This operation involves division of the short gastric vessels proximal to the pylorus and complete mobilization of the body and fundus of the stomach. The greater curvature is then invaginated using two or more layers of nonabsorbable suture [29]. Current data has been insufficient to draw definitive conclusions on the effectiveness of this operation [30]. Feasibility studies have Neurohormonal Modulation Interruption of vagal conduction results in decreased gastric emptying, loss of appetite, and decrease in pancreatic exocrine function, among other gastrointestinal effects. Implantable devices that stimulate, block, or modulate vagal 40 Experimental Alternatives in Bariatric Surgery 451 nerve conduction are a new strategy that is being investigated for management of obesity. The mechanism by which vagal blockade promotes weight loss is not completely understood. Elongation of the small intestine and gastric capacity as part of evolution of our species.
Order albenza paypal
Medication such as Depo-Provera injections may be effective to prevent pregnancy but also can inhibit weight loss after surgery so should be avoided if possible symptoms queasy stomach and headache albenza 400mg sale. Patients presenting to your office with a suspected anastomotic leak can have a wide variety of signs and symptoms. Patients can complain of vague abdominal discomfort, malaise, and low-grade fever. Two important signs and symptoms are shoulder pain (often left-sided referred pain) and tachycardia greater than 120 beats per minute. Any bariatric surgery patients presenting with tachycardia greater than 120 beats per minute should have a high index of suspicion for an anastomotic leak until proven otherwise. If an anastomotic leak is suspected and the patient is clinically stable, communication with the bariatric surgeon performing the procedure should be undertaken. He or she will recommend and facilitate transfer to the appropriate institution if warranted. Time is of importance in diagnosing an anastomotic leak, because, if detected early enough, patients can usually be managed conservatively without necessitating re-exploration. Nausea and Vomiting Postoperative nausea and vomiting is not uncommon and therefore practitioners should be familiar with common etiologies and treatment options. Often just aggressive hydration even without the need of antiemetic medication will suffice for amelioration. If pharmacotherapy is warranted, a scopolamine patch behind the ear every 3 days along with increased hydration is often effective. Eating too much or too quickly or not chewing food adequately can also cause nausea. Postoperative Medical Management Anastomotic Leak Detection With 90 % of all bariatric surgeries being performed laparoscopically, the average length of stay is approximately 2. To this end, although clearly a surgical issue, medical professionals should be cognizant of the signs and symptoms of an anastomotic leak so that appropriate communication and transfer to the surgical facility can be expedited. Small Pouch Syndrome There is a small subgroup of patients who, for unclear reasons, are unable to tolerate much, if any, liquids or solids by mouth after surgery. Moreover, parenteral nutrition may 18 the Perioperative and Postoperative Medical Management of the Bariatric Surgery Patient 181 be warranted in some individuals as well. Another potential etiology is once a small pouch is created during surgery, the nausea and vomiting sensor in their hypothalamus becomes hyperactive to liquids and solids in their newly created pouch. This medication helps with appetite, mood, and sleep, which all can be affected by this "small pouch syndrome" for a lack of a better term. Severe thiamine deficiency (beriberi) results in a spectrum of neuropsychiatric, cardiac, and gastrointestinal symptoms. Neurologic or "dry beriberi" presents with seizures or numbness, pain, and weakness in the extremities. And lastly, gastrointestinal beriberi manifests with delayed emptying of the stomach. Depending on the surgical procedure and institutional rates, one should have a high index of suspicion for Clostridium difficile colitis. A careful history of medications, especially in the liquid form, should be obtained. It is not uncommon for patients to complain of "lactose intolerance" after undergoing a gastric bypass procedure. In reality, their symptoms most likely represent an intolerance to lactose sugar rather than a lactase deficiency for there is no pancreatic manipulation during surgery to account for a true lactose deficiency. The most common cause of postoperative diarrhea seen in at least gastric bypass patients is dumping syndrome. Dumping syndrome is a constellation of gastrointestinal and vasomotor symptoms including nausea, cramping, diarrhea, sweating, palpitations, and lightheadedness. The partially digested food draws excess fluid into the small intestine causing these unpleasant symptoms. Dumping usually occurs after the consumption of too much simple or refined sugar in a patient who underwent gastric bypass surgery. Dietary compliance with avoidance of refined sugars and high glycemic carbohydrates is the primary treatment. It is thought to be related to the early development of hyperinsulinemic (reactive) hypoglycemia. An initially high concentration of carbohydrates in the proximal small bowel results in a rapid absorption of glucose, which is countered by a hyperinsulinemic response. The symptoms include sweating, shaking, loss of concentration, hunger, and fainting. If late dumping persists despite dietary compliance, it may be treated with a small amount of sugar about 1 h after a meal, which may prevent its occurrence. If symptoms are resistant to medical management, the rare possibility of an insulinoma or nesidioblastosis of the pancreas should be considered. Conclusion: Disease Management As stated at the beginning of this chapter, the primary reason for considering bariatric surgery is for the reduction of comorbid medical problems-weight loss is secondary. Medication recommendation immediately postoperatively may need to be adjusted to meet metabolic needs. Preoperative weight loss with a very-low-energy diet: quantitation of changes in liver and abdominal fat by serial imaging. Corazziari E, Badiali D, Bazzocchi G, Bassotti G, Roselli P, Mastropaolo G, et al. Impact of clopidogrel in patients with acute coronary syndromes requiring coronary artery bypass surgery: a multicenter analysis. Continuous perioperative insulin infusion therapy for patients with type 2 diabetes undergoing bariatric surgery. A potential complication of bi-level positive airway pressure after gastric bypass surgery. Continuous positive airway pressure in immediate postoperative period after laparoscopic Roux-en-Y gastric bypass: is it safe Postoperative nausea and vomiting with application of postoperative continuous positive airway pressure after laparoscopic gastric bypass. Improvement of associated respiratory problems in morbidly obese patients after open Roux-en-Y gastric bypass. Prolonged thromboprophylaxis with low molecular weight heparin for abdominal or pelvic surgery. Extended release medications should be changed to regular release formulation and be crushed or in the liquid form for maximum absorption following gastric bypass surgery. Insulin requirements are significantly reduced immediately following gastric banding surgery. Hypertensive medication requirements may be significantly reduced immediately following gastric bypass surgery. Tachycardia greater than 120 beats per minute is an indicator of a possible anastomotic leak. Typically, gastric banding does not cause an immediate improvement in insulin sensitivity and glycemic control. Therefore, continuing 75 % of the preoperative diabetic medication is usually required. Extended thromboprophylaxis with lowmolecular-weight heparins after hospital discharge in high-risk surgical and medical patients: a review. Enoxaparin thromboprophylaxis in gastric bypass patients: extended duration, dose stratification, and antifactor Xa activity.
Safe albenza 400mg
Long-term results of sleeve gastrectomy are also becoming better reported in the literature treatment 4 syphilis buy albenza on line amex. When weight regain occurs, it tends to be after 1 year and seems to be most prevalent between 3 and 6 years. Again, these results may represent early techniques with large pouches and heavier patients. Anatomic Causes of Failure the gastric sleeve created at the initial operation may not maintain its shape or orientation over the long term. This has been attributed to weight regain, inadequate weight loss, and the development of undesirable symptoms postoperatively. Interestingly, in this limited series of patients, antral dilation did not always correlate with excess weight loss. This may in turn lead patients to dietary habits that do not support weight loss in an attempt to control symptoms. The un-calibrated sleeves had inadequate weight loss while that observed in those made with 32 French bougies was superior to the 44 French. Similar results were seen for resolution of dyslipidemia, diabetes mellitus, and hypertension. They cite inad- equate weight loss with larger sizes and increased complications with smaller. Evaluating Failure As previously described, the reasons patients fail to achieve the desired outcomes of their bariatric procedure are diverse. Hopefully, patients are complying with their diet and exercise programs and are being regularly evaluated for this during their scheduled follow-up. Early identification of failure and the symptoms and behaviors that may contribute to inadequate weight loss is important. Often minor, nonoperative interventions may be sufficient to get these patients back on track. Once a patient has been identified as failing after a sleeve gastrectomy, we recommend a full history and physical exam. The history should focus on identifying symptoms of gastroesophageal reflux or obstruction. We recommend reviewing the food and exercise diary as well as reinforcing appropriate behaviors as the initial step in evaluating failing patients. It is best to do the study yourself or at least be present for the examination to ensure that the appropriate concerns are addressed. The study should look for the presence and size of hiatal hernias, which could contribute to reflux symptoms and maladaptive eating. Segmental or generalized pouch dilations as well as the size of the antrum should be evaluated. The rate of pouch emptying should be rapid without delays in any segment or significant reflux into the esophagus. Signs of esophagitis, hiatal hernia, pouch dilation, and volvulus should be evaluated. It is important to recognize that weight regain can occur without pouch dilation or anatomic abnormality. Thus, it is important to fully evaluate each patient prior to embarking on any intervention to address failure. Using this data as justification for conversion to duodenal switch in failing patients should be done with caution. This may also be effective at relieving undesirable symptoms from the sleeve including reflux, stricture, and obstruction. All patients had improvements in weight loss following conversion and those who had reflux were all able to discontinue reflux medication. Similar to the duodenal Managing Failure To date, the options for managing inadequate weight loss, weight regain, or suboptimal resolution of the comorbidities following sleeve gastrectomy have been poorly studied and data is limited. It is, however, intuitive that those patients who are not complying with dietary and exercise recommendations may be able to get back on track if they are willing to change these behaviors. It is important to ensure failing patients are compliant before offering them a surgical intervention. This is especially true since a noncompliant patient is unlikely to benefit from any surgical intervention and should not be exposed to the risks of another operation. Several surgical options have been described to help failing patients lose further weight following sleeve gastrectomy. They can be divided into two groups: conversion to another type of bariatric procedure and revising the gastric sleeve to correct an anatomical complication. Adding an adjustable gastric band to a sleeve gastrectomy patient who failed has also been described. All but one of the patients was successfully operated on laparoscopically and the overall complication rate was 8. Davies Revising a Sleeve Gastrectomy During the evaluation of patients after sleeve gastrectomy, it is important to examine the anatomy and size of their pouch as a possible contributor to their inadequate results. Early sleeves were often made without or with large (>40 French) bougies making excessively large pouches. Larger amounts of gastric antrum were often left and/or the fundus was adequately excised. Even if these large pouches were not intentionally left, some patients develop generalized or segmental dilation of their pouches with time. Revising initial sleeve gastrectomies has been a popular option in failing patients since it preserves many of the beneficial aspects of the sleeve (no inaccessible gastric remnant, lower risk of bowel obstruction and ulceration, less nutritional disturbances, no intracorporeal anastomosis). This was reported initially for patients with dilated pouches and was found to provide improvement in weight loss following sleeve revision [21]. If you have a patient who fails following sleeve gastrectomy and their evaluation shows a problem with the pouch itself, this may be a contributing factor. Antral or proximal dilation is best resected using a 32 French bougie to calibrate the sleeve. Any hiatal hernia or thoracic migration should be addressed with repair, crurual closure, and plication if there is enough stomach for a Hill repair. Obstruction at the angularis can often be managed with pneumatic balloon dilation; however, if this fails strictureoplasty and seromyotomy are options. Conclusion In summary, a thorough evaluation of each patient who fails to achieve the goals of sleeve gastrectomy is necessary to plan the appropriate intervention to address the root cause. Gastric plication has not been reported as a revisional option for sleeve gastrectomy patients, but it may play a role in the future. If the pouch has antral, fundal, or segmental dilation, then segmental revision of the sleeve with or without plication may improve weight loss. Whenever revising a sleeve, strong consideration should be given to suture inversion of the staple line, larger staple size, and buttressing to hopefully reduce the higher risk of leak. The current literature base on revising the sleeve gastrectomy for weight loss failure is limited and difficult to make conclusions from. Results beyond the first year are not available and weight loss may be minimal, transient, or at the cost of malabsorptive complications. Upper gastrointestinal contrast study and endoscopy confirm that she has a stricture in the mid portion of her pouch with dilation of the fundus. Prediction of successful weight reduction after bariatric surgery by data mining technologies. Laparoscopic sleeve gastrectomy performed with intent to treat morbid obesity: a prospective singlecenter study of 261 patients with a median follow-up of 1 year. Predictive factors of excess body weight loss 1 year after laparoscopic bariatric surgery. International Sleeve Gastrectomy Expert Panel Consensus Statement: best practice guidelines based on experience of >12,000 cases. Improved obesity reduction and co-morbidity resolution in patients treated with 40-French bougie versus 50-French bougie four years after laparoscopic sleeve gastrectomy. Sleeve gastrectomy as sole and definitive bariatric procedure: 5-year results for weight loss and ghrelin.
Buy albenza 400mg overnight delivery
For example medicine dropper albenza 400 mg without prescription, all the patient who lost more than 80 % of their excess body weight after metabolic surgery (the cases) are compared to the same number of patients who did not lose that much weight (the controls). The medical records are then reviewed to see what the odds of preoperative diabetes were in the respective groups. A case-control design is used mostly when the outcome of interest occurs infrequently. When events are rare, a retrospective cohort study would have to enroll a prohibitively large number of patients in order to ensure that enough events occur to permit statistical analysis. An important limitation of the casecontrol design is that it does not permit one to make any statements about the prevalence of the predictor in the general population. Therefore, the results of a case-control study can be described in terms of odds ratios but not absolute or relative risks. However, there remains a role for systematic reviews of existing literature and for reporting anecdotal evidence. Meta-analysis in particular is an important method of combining multiple studies in a systematic fashion to draw conclusions that any one study alone could not support. As such, a meta-analysis has the ability to propagate the inherent problems of the initial studies, including publication bias. Lastly, there will always be a need for individual surgeons to report their experiences with novel operative techniques or disease processes in the form of case reports or small series. These studies are not designed to produce statistically significant results or yield definitive conclusions; rather, they serve as the inspiration and foundation for future research efforts. This includes the setting (the country; whether it was a multiinstitutional versus single institution study; whether those institutions are primarily rural or urban, community hospitals or tertiary referral centers; whether underserved minorities are likely to be included in the sample), the dates of the study, the age and sex of the patients (studies based on Medicare data. Studies often list inclusion criteria, which are a set of rules by which the study authors selected patients, followed by exclusion criteria, which eliminate patients from the sample. Inclusion and exclusion criteria should be determined prospectively rather than in an ad hoc fashion (which introduces bias), and the reader should be provided with enough information to decide if these criteria were based on sound logic and clinical precedent. The conclusions of the study can only fairly be applied to patients similar to those studied. The authors may by inference form a broader conclusion but should state that they are doing so. For example, the conclusions of a multi-institutional study from California can probably be applied to patients in New York. However, a study based on Medicare data is unlikely to yield conclusions that can be rightly applied to the population of 30- to 40-year-olds. In this case, the hypothesis may be reasonably formulated as "we predict that it will be possible to identify factors associated with readmission" or "we predict that certain patient comorbidities and postoperative complications will be associated with readmission. Researchers are often taught to picture first the ideal study to test their hypothesis and then modify that ideal to fit practical constraints. Not uncommonly, these modifications result in a study that only tests an approximation of the initial hypothesis. Predictors and outcomes that are unambiguously defined- patient age or mortality, for example-are unfortunately the exception. Things that are of equal clinical interest such as surgeon training, postoperative complications, and patient satisfaction are often subjective in their nature. It is important that the study describes the method in which the predictor, outcome, and important potential confounders were measured. If the outcome of interest is postoperative pneumonia, the study should state clearly how pneumonia was defined. Some measurement problems may be intrinsic to the data source used by the study authors. Retrospective observational studies, especially those that make use of a large clinical or administrative database, are limited to data that have been recorded without the study goals in mind. Large databases also often make use of broad definitions for the sake of simplicity and for the purposes of including a wide array of patients and procedures. Administrative databases pose a particular risk because they are based on billing rather than clinical information. Clinical conditions must be deduced from claims information, a process that is usually only moderately successful. Patient-centered outcomes such as a patient satisfaction and quality of life are an increasingly important part of clinical research. Most of the time, the title alone should be an indication of what question the authors set out to answer. Most hypotheses come in the form of the relationship between a predictor (the independent variable) and an outcome (the dependent variable). For example, a study may hypothesize that using a retrocolic roux limb during gastric bypass is associated with fewer cases of internal hernia. In this example, the surgical approach is the predictor and the rate of internal hernia occurrence is the outcome. Other validated survey instruments exist that are specific to certain patient groups, medical conditions, and procedures. In survival analysis, a researcher can make use of these data to perform a robust analysis, even if overall follow-up rates are disappointing. The result of any study-whether it is positive or negative-is the product of one of four things: chance, bias, confounding, or truth. A published study should contain enough information to allow the reader to decide how much is truth and how much could be explained by the other three. Study patients are frequently lost to follow-up or have important pieces of information missing from their record. It is important that a study acknowledges if there were problems with missing data. Missing data may introduce a substantial source of bias if the data are missing not in a random fashion but because of a specific reason. There are several techniques for dealing with missing data and the authors of a study should be explicit about which they used. If the missing data represent potential confounders that should be included in a regression model, they may choose to exclude any patients who lack a record of those confounders or omit those confounders from the model entirely. The former may introduce bias and the latter may have a negative impact on how well the study captures the effect of the predictor on the outcome. If the confounder is particularly important, its absence from the model may invalidate the results. Lastly, the authors may make an informed assumption about what that data would have looked like and use these values in the analysis. Survival (or time-to-event) analysis represents a subset of statistics that deals with missing data in a special fashion. In survival analysis, the outcome of interest is not a timespecific data point (like 30-day mortality or weight loss at 2 years) but rather the amount of time it takes a patient to reach a certain point (like time to death or time until hernia recurrence). Invariably some patients will be lost to follow-up prior to this event occurring or will not have had an event at all by the conclusion of the study. However, it will be known how much time the patient was followed without an event Chance Statistics is fundamentally the science of distinguishing meaningful results from random chance. If we flip a coin ten times and it lands on heads all but twice, should we conclude that the coin is weighted If the treatment group loses an average of fifteen pounds and the control group loses seven, did the treatment really work Mistaking the effects of chance for a meaningful result is known as an alpha error. Results are believed to be meaningful if they reach a level of statistical significance. Theoretically, any result could be the product of chance (flip a coin enough times and eventually, you will encounter a streak of fifty heads in a row) and so by convention, the bar for statistical significance (the p value) is set at 0. Fischer in 1933 and has endured partly by convention and partly because many researchers feel it makes intuitive sense (perhaps, most people can accept a coin landing on heads five times in a row, but after the sixth time, they start to get suspicious-the p value for six straight heads or tails is 0. Alpha error can be reduced by increasing the size of the sample and/or by working with data that are likely to follow a predictable distribution. However, it is important to remember that there is nothing magical about a threshold of 0. The potential for random chance to be mistaken for a meaningful result always exists.

Best buy for albenza
Review quality standards treatment wetlands cheap albenza, accreditation, and data collection requirements among various bariatric surgery programs. Throughout the history of surgical intervention, surgeons have been keenly interested in improving patient safety, and in almost every surgical field improvements have been made. Metabolic and bariatric surgeons, criticized for offering operations to patients who suffer from the "lifestyle" disease of obesity, have by necessity embraced accreditation as a pathway to provide a structure of programmed longitudinal care. Collecting data, reporting of outcomes, and using outcomes for improvement within the structure of accreditation serve to garner the support of hospitals, staff, and colleagues for these efforts and provide an economic context for the inclusion of integrated health staff in the longitudinal pathway of care. In the history of surgery, there may not have been a more focused or successful effort, resulting in a reduction of mortality from 0. Their findings included all consecutive coronary artery bypass grafts (isolated) within all centers and by all surgeons in Vermont, Maine, and New Hampshire from 1987 to 1989. After the announcement of these findings, a decline occurred in the variation; the first inflection was in just making the programs and centers aware of the results (Hawthorne effect) [4]. Sharing of best practice and structured improvement process led to further gains, driving the mortality to its lowest level of under 2 % by 2001. The History of Quality in Bariatric Surgery One of the most critical elements of quality seems selfevident, but it is to know your own outcomes. First, they do not believe the information; then, they question whether it is adjusted for the level of risk of the patient; and finally, they accept it and immediately begin to try and figure out how to improve. In addition, accumulating high-quality data through well-designed prospective, randomized studies that includes strict study design, data collection, and publication occurs in such a long cycle of time that it may become irrelevant to some degree in terms of the use of data to impact quality immediately and improve care for individual patients at the local level of care in real time and on an ongoing basis. In addition, once results of these trials are published, the individual surgeon/program has to know of the data and be able to integrate it into their own course of care-a daunting task for busy clinical practitioners. While level 1 data remains the gold standard, questions about cost and applicability to community practice have been raised leading to a movement led by the Institute of Medicine to define and revise the clinical trial infrastructure [7]. We had full financial support from one of the staple companies for the first two years. Subsequent support was to come from participating surgeons who were voluntary members and had the additional expense of their satellite program of data collection and reporting. A professor from Preventive Medicine provided advice regarding statistical work and consultation for the graduate student. Direct access to the Registry data was limited to those working in the central office. I wrote a section for surgeons and Kathleen wrote a section for the people who were collecting and reporting data. At this early stage, community surgeons may not have seen a clear need to participate in data collection. However, a confluence of events forced bariatric surgery into the glare of public opinion, accelerating the need for a national approach to quality. This one controversial change in approach to the procedure heralded the acceleration of adoption by patients who were seeking help for obesity-in part because of the publicity that surrounded the laparoscopic gastric bypass of Carnie Wilson, 14 Quality in Bariatric Surgery 70 63. In the early part of that decade, general surgeons-many of whom had never practiced bariatric surgery-took a weekend course and, with little training or program structure, started offering the procedure. What had been heralded as a step forward quickly led to a host of complications and deaths that threatened to swamp the nascent specialty and close down access to care. Payers, employers, and others began to drop the procedure as the cost of surgery mounted. In one single year (2005), the entire State of Florida lost all effective access to care unless a patient was able to self-pay for a procedure. Malpractice claims jumped, causing insurance to become extremely expensive if it was available. Bariatric surgery, and the patients who need surgical therapy for obesity and related disease, was in crisis and patients were on the verge of losing all access to the procedures. Payers were not pleased with the red ink they saw from the increase in complications. Faced with increasing demand by employers and patients, they stepped up to manage the situation. Payers had experience in managing high-risk specialties, having had to manage transplantation networks for many years. In conjunction with employers, they began designing similar systems to try and control access to bariatric surgery. In Las Vegas, several unions and employers expressed concerns regarding data indicating expensive complications for an elective surgical procedure. Nine programs responded and three were invited to come to Las Vegas to meet with Mr. Two programs were selected and then the negotiation of the actual contracts took place. By early 2005, this prototype of the payer/employer-driven center of excellence was in place and patients were being referred only into this network. There was a contraction in access to bariatric surgery, particularly in rural areas. The routine reporting and compiling of outcomes from bariatric surgical patients will provide an opportunity to assess and verify risks and benefits of therapy, which can potentially resolve many of the conflicts over the role of surgery in severe obesity. The result, however, was that as the terms of office of the original board members expired, they were rotated off. This included the use of funds for development of the program, the strategy of the programs development, and contracting for release of data to outside parties. These decisions had secondary consequences to programs that were outside the oversight of the society. Data collection was made by an independent clinical reviewer and not by someone who participates in the bariatric program. Data began to accumulate on these centers that showed similar outcomes at lower volumes within the context of an accreditation program. Blackstone Study Group (detailed previously) pioneered the model that was adapted in Michigan. Hospitals and surgeons convene to review and interpret the data, identify best practices, and implement them across the region. The actual process for implementation is done on the local level based on the resources available. The data is collected through a central data management center with independent third-party abstractors. Gradually in Michigan, even surgeons who were initially skeptical or reluctant have come around to be supportive. One surgeon said, "quality and performance are going to drive our collective future, it is nice to have guidance and ownership in the process. Using the initial quality matrix, programs were accredited based on structural and process elements only, not on outcomes. Centers who achieved national accreditation might not have good outcomes or excluded programs might have excellent outcomes. Those programs with poor outcomes were not required to have a mechanism to examine the data and improve. The database had not provided any risk-adjusted data in feedback back to the programs that entered the data since its implementation in 2007. In addition, it was difficult for new programs to get started and they went through their entire learning process before they entered the program rather than being able to utilize the best practices of the program from the beginning. The volume requirement became difficult to maintain in many programs as the economy worsened. In fact, as the volumes started to come down around the country in response to the recession, more than 35 % of programs were not going to qualify in the next round of accreditation. Finally, because of the volume requirement very little, if any, data existed on safety with lower volumes. They were established in an era where expert opinion rather than peer-reviewed data was used to justify them. These had not been systematically reexamined for relevancy and were often expensive additions to program structure, especially for rural and smaller hospitals. The extent to which these requirements impact quality and patient safety was unknown.

Order albenza online
This risk is influenced by common comorbid conditions including diabetes medicine kidney stones order line albenza, hyperlipidemia, chronic inflammation, and a prothrombotic state. Diagnosed or occult coronary artery disease will increase the risk in bariatric surgery. The exact prevalence of coronary disease in bariatric surgery candidates is unknown, but acute cardiac complications following bariatric surgery are well known and occur in 0. The Revised Cardiac Risk Index [12] identifies risk factors for perioperative complications in the general population as specific predictors for cardiovascular complications after surgery. These risk factors are derived from studies of large numbers of patients undergoing elective noncardiac surgical procedures. The risk of a cardiovascular complication increases with the number of risk factors present. Although such an index has not as yet been established for patients with extreme obesity, it is likely that these risk factors should be used in decision-making regarding the need for additional cardiovascular studies. It is quite likely that young patients who are not superobese and who have no risk factors do not need routine detailed cardiovascular testing. In bariatric patients with multiple risk factors, additional cardiovascular testing is indicated in order to initiate treatments to reduce risk and to better prepare for perioperative management and resource allocation. There are no guidelines for the necessity of additional noninvasive cardiovascular testing in severe obesity. Recommendations are derived from the published guidelines for cardiac evaluation for noncardiac surgery [12]. A functional assessment of exercise capacity is an essential part of the evaluation. A patient with known coronary artery disease and on treatment in a regular physical exercise program may be of less cardiovascular concern than a patient with risk factors who has a very limited functional capacity. Aerobic exercise capacity has been studied in bariatric surgery candidates and the findings are striking in that aerobic fitness levels in extreme obesity are similar to those seen in patients with varying degrees of heart failure [13]. Exercise testing is also a possible predictor of major postoperative complications as they appear to cluster in patients with major limitations in maximal oxygen consumption [2]. Cardiovascular physiologic changes associated with extreme obesity are summarized in Table 17. Exercise testing is an important component of noninvasive cardiac testing, because it may demonstrate symptoms and signs of ischemia in patients with occult and asymptomatic disease that is clinically significant. As many bariatric surgery candidates are not able to exercise because of extreme obesity, dobutamine may be substituted for exercise to produce cardiovascular stress. Stress echocardiography is a more accurate method of assessing cardiac structure and function in extreme obesity. When external ultrasound quality is limited by echocardiography windows and adequate images, consideration should be given to transesophageal ultrasound with stress administered to achieve an adequate heart rate. The accuracy of thallium scanning is reduced in patients with extreme obesity and is of little value. Thrombosis Obesity is also a risk factor for arterial and venous thrombosis through a variety of mechanisms involving substances secreted by adipose tissue, direct effects on the coagulation factors, oxidative stress, and the association with chronic inflammation. Obesity is associated with increased production of pro-oxidant substances that promote endothelial dysfunction and platelet aggregation, which promotes thrombosis. The prothrombotic conditions associated with obesity contribute to the cardiovascular risks in obesity and the cardiovascular complications following bariatric surgery. These metabolic changes form the rationale for aggressive pharmacotherapy for thrombosis prevention during the perioperative period. The prothrombotic tendencies in obesity improve with weight loss, another exciting area in bariatric surgery outcomes [14]. Many bariatric surgery candidates are taking oral agents for long-term anticoagulation for indications related to cardiovascular disease treatment or prevention. Patients with chronic atrial fibrillation or prosthetic heart valves will require anticoagulation during the preoperative period, transition to heparin or low-molecular-weight heparin before surgery, and aggressive perioperative prophylaxis with heparin or low-molecular-weight heparin with transition to full anticoagulation while under close surveillance. Heparin and low-molecular-weight heparin should be dosed on the basis of patient body weight. The ability to identify high-risk patients during the preoperative preparation allows for more intense focus and attention to these patients as they proceed through the evaluation phase, better decision-making regarding fitness for surgery, and better preparation for surgery and the necessary resources for the perioperative period. Close collaboration between the surgeon, the bariatric physician, and specialists is essential for patient selection and optimal outcomes. The study of the efficacy of bariatric risk reduction during the preoperative period is a new and important area of study in bariatric surgery. Little is known regarding the effects of intensive psychological counseling, behavioral treatment, or patient education, used either before surgery, or as an adjuvant treatment. Additional studies are needed to see if patients with behavioral or mental health conditions that reduce the likelihood of a successful weight-loss result can be improved with more intensive mental health treatment. Supervised weight loss in the preoperative period has been used as a method of risk reduction by bariatric programs. The catabolism associated with the use of hypocaloric diets or very low calorie diets does not contribute to nutritional or wound healing problems affecting surgical outcomes. A recent study of 881 patients from Geisinger Medical Center [19], where supervised preoperative weight loss is strongly encouraged during the 6 -month preoperative program, found that 67 % of the patients were able to lose more than 5 % of excess body weight and 48 % were able to lose more than 10 % of excess body weight. Weight loss of this magnitude in extreme obesity will improve physiology by lowering blood pressure, improving glucose control, inducing spontaneous diuresis in those with expanded extracellular fluid volume, and improving pulmonary gas exchange. Risk-Benefit Analysis the decision to offer bariatric surgery, when to proceed with surgery, and which operation to offer should be driven by the preoperative comprehensive assessment. Risk issues to be carefully considered include the operative risks based on patient health factors and an analysis of predictors of a successful long-term weight-loss result. For a high-risk patient who does not appear motivated and capable of the necessary lifestyle changes, the surgical risks may be deemed greater than the anticipated benefit. The advent of institutional and administrative databases as well as clinical registries have allowed for the identification of patient factors that increase the surgical risks of bariatric surgery. There are several bariatric risk scoring tools that are now available to assist bariatric programs in identifying high-risk patients. Dalencourt the effects of preoperative weight loss on outcomes in bariatric surgery have been studied in a number of small observational studies with inconclusive results. The favorable effect of preoperative weight loss on 30-day complication rates was recently demonstrated in a multicenter, randomized controlled trial of 273 patients comparing a 2-week very low calorie diet with usual diet [21]. Additional controlled studies investigating the beneficial effects of preoperative weight loss and its effect on patient physiology and surgical complications are needed. Shortterm preoperative weight loss is achievable in bariatric surgical candidates using hypocaloric diets, very low calorie diets, pharmacotherapy, less invasive endoscopic procedures, or various combinations of these therapies. The ability to identify high-risk bariatric candidates and to intensify risk reduction treatments should favorably influence surgical results. In a patient with extreme obesity for 20 years, surgeons can expect diminished cardiac reserve related to structural and functional changes in the heart. Which patient requesting bariatric surgery is least likely to be successful in achieving long-term weight loss after bariatric surgery Major complication rates following bariatric surgery are similar to complication rates following cholecystectomy. In the era of expanding bariatric surgery treatment to more of the population who may benefit from this treatment, bariatric programs need to refine and reformat preoperative patient assessment techniques and treatments in order to identify early patients who are at risk for early surgical complications and later struggles with health and weight loss. Early identification of these patients will increase the program focus on these patients and the development of risk reduction strategies. The unique knowledge and skill of the experienced bariatric surgeon, the close collaboration with the multidisciplinary bariatric program personnel, and strategic input from consultants should be components of the important task of patient selection for surgery. Physical activity levels of patients in the longitudinal assessment of bariatric surgery study. Psychological evaluation of bariatric surgery candidates: a survey of present practices. Cardiovascular evaluation and management of severely obese Question and Answer Section Questions 1. The following are risk factors for operative mortality after bariatric surgery except: A. Outcomes of preoperative weight loss in high risk patients undergoing gastric bypass surgery. Van Nieuwenhove Y, Dambrauskas Z, Campillo-Soto A, van Dielen F, Wiezer R, Janssen I, et al.
Purchase 400 mg albenza free shipping
After that meeting medications every 8 hours purchase albenza 400mg free shipping, initial interest in possible collaboration was confirmed by both parties. A subsequent meeting was held with the Board of Regents Committee on Research and Optimal Patient Care in October 2012. Based on the recommendation by the Committee, the Board of Regents during that annual clinical congress in 2012 voted unanimously to endorse the process of integration of the two programs. In November and December, an extensive series of webinar town halls were presented to a 14 Quality in Bariatric Surgery 165 large segment of the leadership with broad consensus that the society was moving in the correct direction. The data was used to provide initial information to the Committee and Executive Council about the relative strength of volume as compared to a composite measure for judging the safety record or a program that participated in the network. In January, at the Executive Council retreat, these proposals were evaluated in detail. The most important task ahead was integration of the culture of the two partners in quality. They had to be able to rigorously examine every aspect of the current quality paradigm in both societies in order to propose a system of quality. There could be no "sacred cows" and each aspect of the previous programs had to be examined. In other words, the beginning of the acculturation could not be political and it had to be patient centric. This step would include change for both groups and change is perhaps on a large scale one of the most difficult integrations to manage. Blackstone Four initial committees were formed, with each society nominating one-half of the committee members and with a shared cochairmanship. Once an initial draft was made, critical issues were identified and the larger committee met repeatedly over the next 4 months to work through pivotal issues like minimum qualifying volumes. Each step of the process was examined and voted on by both the Standards Committee members and members of the oversight committee prior to being changed within the document. The qualifying minimal volume issue was one of the most discussed with a final agreement that 50 cases per year was adequate to ensure sufficient experience for accreditation in all patients regardless of acuity. Programs were able to become part of the system for low-acuity patients at 25 cases per year. In addition, new programs could enter the registry as a data collection center, allowing them to accumulate their data and taking advantage of best practice available within the system from the first case forward. Other difficult issues, including individual surgeon verification, were discussed at length. The council voted to send it for public comment but did not endorse it, waiting instead for the public comments and revisions that would ensue based on those comments. More than 1,300 public comments were received and the input sorted into categories. At this point, additional members of the Executive Council were added to each committee to include a broader representation, and each area of input from the membership was carefully considered and amendments were made to the initial draft. The response to this draft was less robust, as expected when many of the issues raised by the first draft had been clarified. Introduction the most important element in establishing a culture of safety is leadership. Currently, the standard for practice of metabolic and bariatric surgery in the United States is to participate within a nationally accredited program. The goal of the local committee is to deliver superior patient experience and safe outcomes with long-term effectiveness in all patients in the program who chose metabolic or bariatric surgery. Each member of the committee not only can contribute their efforts to instill the habits of quality within the program but also has the ability to continuously evaluate their own efforts (through review of their own data in the registry) as well as compare to surgeons both locally and nationally. Analysis of outcomes can lead to evaluation of technical, structural, and process aspects of the program and drive changes that improve care. The committee members embracing the quality process establish a continuing learning community within the program. The committee provides the ideal group to meet the challenges of the new medical environment: improved patient safety, enhanced patient experience, growing access, and maximizing revenue while minimizing cost. A leader sets direction, aligns people around common goals, and motivates and inspires the team to reach them. A manager plans and sets a budget, organizes staffing, and controls activity and solves problems [22]. The responsibility for a successful effort is a shared responsibility of the entire committee. Many opportunities for improvement in safety and patient care will come from the data but also can arise from within the team. All surgeons who operate within the program should optimally participate in every meeting of the local committee. Once accurate data is collected, it can be analyzed to provide information that can be turned into improvement in quality. The science of measuring variability and predicting the future performance of a facility or hospital has advanced. The important question is explaining what in a given process produces the variation Iezzoni attributes variation to her "algebra of effectiveness," meaning variation in outcomes is attributed to one of three factors: chance, case mix, and quality of care [25]. This model has evolved as the understanding of contributory processes has evolved. Representatives to the task force were appointed by each society and a combined statement of credentialing recommendations was published under the leadership of William B. Risk Adjustment (Antecedent Conditions) A key element in reducing variation is to understand the risk of the population and determine the case mix. The program will need to decide what level of risk the group is willing to accept. Exceptions to the board certification requirement can be made on a case-by-case basis State medical licensure in good standing Completion of an accredited bariatric surgery fellowship. The absolute number of proctored cases is left up to the local credentialing committee. It is recommended that practitioners performing endoluminal bariatric procedures should be credentialed to perform bariatric surgery, and if not, they should be an active member of an accredited, structured bariatric surgery program Table 14. Blackstone impact how to address the structure and process parts of the quality paradigm. What is the level of expertise of the surgeons and integrated health staff, and what procedures do they have the experience or expertise to perform What is the risk of the procedures that will be performed, and which ones should the program provide to patients What is the level of support that the program must have for special groups (adolescent patients, elderly, super morbid obese patients, transplant patients, etc. What is the risk the patient brings with them, and how can you manage that risk during the perioperative period Special Groups of Patients Against the backdrop of established structure and process of care is the provision of surgical care to special groups of people: patients seeking revisions of a previous bariatric procedure, adolescent and elderly patients, extremely large patients, patients with high metabolic acuity, transplant patients, high psychological acuity (schizophrenic/bipolar or severe personality disorders), patients paying cash, patients who become pregnant after surgery, and research patients seeking new procedures. Each of these special groups of patients should be reviewed in the context of the program structure and process to see what protocols and processes need to be put in place for their optimal management if surgery will be offered to them. The recently published standards provide for programs doing as few as 25 stapled cases per year to restrict operations to a lower-risk patient group and still participate in the program. The solutions for each patient group will differ from program to program, but having a specific plan for these groups and adhering to it will provide an opportunity to link best practices with others providing similar care. Expertise Expertise is required not only in surgeons but also in the integrated health staff. Credentialing of surgeons using the recommended requirements discussed earlier will establish a consistent level of surgeon expertise within the program. Networking with other programs will also help your program define these roles and the proper credentials for them. Patient Risk In order for risk adjustment to accurately predict future adverse events, complications must occur with sufficient frequency to be analyzed statistically. In addition, the complications need to occur in a predictable pattern, as in cardiac surgery. There are several older trials in bariatric surgery that have completed a correlation analysis to identify risk factors associated with mortality or other complications in bariatric surgery using primarily an open cohort or mixed patient cohort. The effect on mortality of the open approach is so profound [28] that when these are mixed, a different picture of risk emerges than when a solely laparoscopic cohort is used. If your program is offering open procedures, then you need to compare the data and think about patient risk in this context. The variability of these analyses also speaks to the low frequency of serious complications, the lack of consistent correlation of specific risk factors with these complications, and, to some extent, variable statistical analyses and approaches.


