Buy generic januvia online
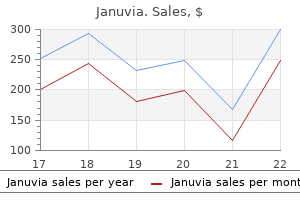
Unfortunately diabetes type 2 how to lower blood sugar buy januvia 100mg cheap, this has had limited success in the clinical setting (Rijnders et al. This combination consistently reduced viable biofilm-associated bacteria levels relative to the control therapies (Aslam et al. The concentration of tigecycline in the infected bone was noted to be higher than in the noninfected bone. Comparative activities of tigecycline and other tetracyclines against nonfermenting gram-negative bacilli, excluding Acinetobacter spp. Clinical and microbiological outcomes of serious infections with multidrug-resistant Gramnegative organisms treated with tigecycline. Combination of tigecycline and N-acetylcysteine reduces biofilm-embedded bacteria on vascular catheters. The efficacy and safety of tigecycline for the treatment of complicated intra-abdominal infections: analysis of pooled clinical trial data. Tigecycline does not induce proliferation or cytotoxin production by epidemic Clostridium difficile strains in a human gut model. Safety and efficacy of intravenous tigecycline in treatment of community-acquired pneumonia: results from a double-blind randomized phase 3 comparison study with levofloxacin. Glycylcyclines bind to the high-affinity tetracycline ribosomal binding site and evade Tet(M)- and Tet(O)-mediated ribosomal protection. In vitro activities of tigecycline against erythromycin-resistant Streptococcus pyogenes and Streptococcus agalactiae: mechanisms of macrolide and tetracycline resistance. Pharmacological and patient-specific response determinants in patients with hospitalacquired pneumonia treated with tigecycline. Activities of tigecycline and comparators against Legionella pneumophila and Legionella micdadei extracellularly and in human monocyte-derived macrophages. Evaluation of the in vitro activity of tigecycline against multiresistant Gram-positive cocci containing tetracycline resistance determinants. In vitro activity of tigecycline against isolates from patients enrolled in phase 3 clinical trials of treatment for complicated skin and skin-structure infections and complicated intra-abdominal infections. Antimicrobial susceptibility among Gram-positive organisms collected from pediatric patients globally between 2004 and 2011: Results from the Tigecycline Evaluation and Surveillance Trial. Comparative in vitro antimicrobial activity of tigecycline, a new glycylcycline compound, in freshly prepared medium and quality control. Tigecycline possibly underdosed for the treatment of pneumonia: a pharmacokinetic viewpoint. Systemic review and meta-analysis of the effectiveness and safety of tigecycline for treatment of infectious disease. Tetracycline antibiotics: mode of action, applications, molecular biology, and epidemiology of bacterial resistance. Tigecycline for treatment of pneumonia and empyema caused by carbapenemase-producing Klebsiella pneumoniae. Antimicrobial activity against Streptococcus pneumoniae and Haemophilus influenzae collected globally between 2004 and 2008 as part of the Tigecycline Evaluation and Surveillance Trial. High dose tigecycline in critically ill patients with severe infections due to multidrug-resistant bacteria. The role of tigecycline in the treatment of infections in light of the new black box warning. Tigecycline in combination with other antimicrobials: a review of in vitro, animal and case report studies. Press release: Wyeth withdraws its application to extend the marketing authorisation for Tygacil. Effectiveness and safety of high-dose tigecycline-containing regimens for the treatment of severe bacterial infections. Susceptibility of important Gram-negative pathogens to tigecycline and other antibiotics in Latin America between 2004 and 2010. Ann Clin Microbiol Antimicrob 11: 29 Fernandez-Mazarrasa C, Mazarassa O, Calvo J et al. In vitro activities of tigecycline and 10 other antimicrobials against nonpigmented rapidly growing mycobacteria. Activity of tigecycline in the treatment of acute Burkholderia pseudomallei infection in a murine model. Presence of tetracycline resistance determinants and susceptibility to tigecycline and minocycline. Tigecycline is efficacious in the treatment of complicated intra-abdominal infections. Comparison of tigecycline with imipenem/cilastin for the treatment of hospital-acquired pneumonia. Antimicrobial activity of tigecycline tested against organisms causing community-acquired respiratory tract infection and nosocomial pneumonia. Activity of tigecycline tested against a global collection of Enterobacteriaceae, including tetracycline-resistant isolates. In vitro activity of tigecycline and comparator agents against a global collection of Gram-negative and Gram-positive organisms: Tigecycline Evaluation and Surveillance Trial 2004 to 2007. Acute pancreatitis related to tigecycline: case report and review of the literature. Clinical uses of the drug 1263 in vitro activity of tigecycline, a glycylcycline antimicrobial. Comparative in vitro susceptibilities of 396 unusual anaerobic strains to tigecycline and eight other antimicrobial agents. In vitro activity of daptomycin in combination with -lactams, gentamicin, rifampin and tigecycline against daptomycin non-susceptible enterococci. Antimicrobial susceptibility of extended-spectrum beta-lactamase producers and multidrugresistant Acinetobacter baumannii throughout the United States and comparative in vitro activity of tigecycline, a new glycylcycline antimicrobial. Metabolism, excretion, and pharmacokinetics of [14C] tigecycline, a first-in-class glycylcycline antibiotic, after intravenous infusion to healthy male subjects. Pharmacodynamics of cefepime alone and in combination with various antimicrobials against methicillin-resistant Staphylococcus aureus in an in vitro pharmacodynamic infection model. In vitro activity of tigecycline against clinical isolates of Acinetobacter baumannii and Stenotrophomonas maltophilia. Clonal diversity and resistance mechanisms in tetracycline-nonsusceptible Streptococcus pneumoniae isolates in Poland. Linezolid- and vancomycin-resistant Enterococcus faecium endocarditis: Successful treatment with tigecycline and daptomycin. In vitro activity of tigecycline and comparators against Gram-positive and Gram-negative isolates collected from the Middle East and Africa between 2004 and 2011. Tigecycline for the treatment of multidrug-resistant (including carbapenemresistant) Acinetobacter infections: a review of the scientific evidence. In vitro activities of tigecycline against recently isolated Gram-negative anaerobic bacteria in Greece, including metronidazole-resistant strains. In vitro activity of daptomycin and tigecycline against coagulase-negative staphylococcus blood isolates from bone marrow transplant recipients.
Generic januvia 100mg mastercard
Resistance to streptogramins is medi ated by three possible mechanisms: drug inactivation by enzymes diabetes mellitus results in quizlet order 100mg januvia, efflux or active transport of the antibiotic out of the cell, and plasmidcoded conformational alterations in ribo somal target binding site (Nadler et al. The third is the most common expression of bacterial resistance to strepto gramins. Drug inactivation can occur in some staphylococcal and enterococcal species by production of a quinupristin inactivating hydrolase or a dalfopristininactivating acetyl transferase. Emerging resistance during the treatment of infections caused by vancomycinresistant E. The antibiotic susceptibility of glycopeptideresistant enterococci was investigated in a Tertiary Greek Hospital. Aerobic Gram-positive strains Susceptible Enterococcus faecium Staphylococcus aureus Coagulase-negative staphylococci Streptococcus agalactiae Streptococcus pneumoniae Streptococcus pyogenes Group C streptococcus Group G streptococcus Enterococcus avium Enterococcus casseliflavus Enterococcus durans Enterococcus faecalis Enterococcus gallinarum Pediococcus spp. Mycoplasma pneumoniae Enterobacteriaceae Haemophilus parainfluenzae Neisseria spp. Each compound binds to sequential sites located on the 50S subunit of the bacterial ribosome (Finch, 1996; Nadler et al. It is thought that dalfopristin blocks attachment of the substrate to both the acceptor site and the donor site of the peptidyl transferase catalytic center, thereby inhibiting the elongation phase of ribosomal replication of Grampositive organisms. It has further been speculated that quinupristin blocks pep tide bond synthesis, which prevents the extension of poly peptide chains and promotes the detachment of incomplete protein chains. Dalfopristin exerts effects in the early stages of protein synthesis, whereas quinupristin is active in the later stages. In addition, dalfopristin binding causes a confor mational change in the ribosome that subsequently increases the binding of quinupristin. Each singleuse vial provides a total of 500 mg of sterile pyrogenfree lyophilized formulation of active drug (quinupristin, 150 mg; dalfopristin, 350 mg). The formula tion should be reconstituted by slowly adding 5 ml of water with or without 5% dextrose. The vial should be then gently swirled by manual rotation without shaking to ensure disso lution of contents while limiting foam formation, and the solution should be allowed to sit for a few minutes until all the foam has disappeared. The reconstituted solution should be added to 250 ml of 5% dextrose solution (approximately 2 mg/ml). The desired dose should be administered by intrave nous infusion (preferably via a central venous catheter) over 60 minutes. Concomitant administration of hydrocortisone or diphenhydramine does not appear to alleviate venous pain or inflammation. The storage time of the diluted solution should be as short as possible to minimize the risk of microbial contamination. In patients under going continuous ambulatory peritoneal dialysis, dialysis clearances for quinupristin, dalfopristin, and their major metabolites are negligible. The high molecular weight of both components suggests that it is unlikely to be removed by hemodialysis. Accordingly, no dosage adjustment of quin upristin and dalfopristin seems required for use in patients with renal impairment or patients undergoing peritoneal dialysis (Chevalier et al. The minimum recommended treatment duration for complicated skin and skin structure infections is 7 days. In patients with hepa tic cirrhosis (ChildPugh A or B), the termination halflife of quinupristin and dalfopristin was not changed. Quinupristin and dalfopristin are converted via nonenzymatic reactions to metabolites that contribute to the antimicrobial activity, but are essentially present as the unchanged form in plasma. Because of rapid ex vivo degradation, plasma samples are usually acidified to pre vent quinupristin and dalfopristin breakdown. Drug distribution Quinupristin and dalfopristin extravascular distribution is relatively limited as assessed from the relatively low volumes of distribution at steady state (Vdss), respectively 0. Quinupristin and dalfopristin concentrations have been determined in wholetissue homogenates including liver, kid ney, spleen, blood, bone marrow, salivary glands, adrenals, and the intestinal contents (Bergeron et al. However, wholetissue con centrations are difficult to interpret, making such studies of limited interest (Mouton et al. In monkeys, concen trations of radiolabeled drug in tissue exceeded those in blood in the kidney, liver, spleen, and salivary glands. Extravascular fluid penetration was investigated in two human studies of suction blister fluid concentrations (Bergeron et al. Pharmacokinetics and pharmacodynamics 1379 due to experimental artifacts, because radiolabeled drug was recovered from the lung in animal models and efficacy has been reported in clinical trials of pneumonia (Nix, 1998).
Diseases
- Xanthic urolithiasis
- Taurodontism
- Cataract aberrant oral frenula growth retardation
- Osteosclerosis autosomal dominant Worth type
- Asphyxia neonatorum
- Prosopamnesia
- Autoimmune hepatitis
- Myocardium disorder
- Urticaria
- Metaphyseal anadysplasia
Order generic januvia from india
In vitro activity of carbapenem antibiotics against beta-lactam susceptible and resistant strains of Burkholderia pseudomallei diabetic diet education handouts purchase januvia 100 mg line. Population pharmacokinetics of meropenem in plasma and cerebrospinal fluid of infants with suspected or complicated intra-abdominal infections. In vivo selection of carbapenemresistant Klebsiella pneumoniae by OmpK36 loss during meropenem treatment. Practice guidelines for the diagnosis and management of skin and soft tissue infections: 2014 update by the infectious diseases society of America. Potent activity of meropenem against Escherichia coli arising from its simultaneous binding to penicillinbinding proteins 2 and 3. Synergistic efficacy of meropenem and rifampicin in a murine model of sepsis caused by multidrug-resistant Acinetobacter baumannii. Use of carbapenems against clinical, nontyphoid Salmonella isolates: results from in vitro and in vivo animal studies. Carbapenem resistance in Klebsiella pneumoniae not detected by automated susceptibility testing. Pharmacokinetics of meropenem in patients with renal failure and patients receiving renal replacement therapy. Single-dose pharmacokinetics of meropenem during continuous venovenous hemofiltration. Carbapenemases in Klebsiella pneumoniae and other Enterobacteriaceae: an evolving crisis of global dimensions. Meropenem population pharmacokinetics in critically ill patients with septic shock and continuous renal replacement therapy: influence of residual diuresis on dose requirements. Are interstitial fluid concentrations of meropenem equivalent to plasma concentrations in critically ill patients receiving continuous renal replacement therapy Antibiotic therapy for prophylaxis against infection of pancreatic necrosis in acute pancreatitis. Assessment of hypersensitivity reactions in patients receiving carbapenem antibiotics who report a history of penicillin allergy. Results of a randomized, multicenter trial of meropenem versus clindamycin/tobramycin for the treatment of intra-abdominal infections. An international, multicentre survey of beta-lactam antibiotic therapeutic drug monitoring practice in intensive care units. Fourth Belgian multicentre survey of antibiotic susceptibility of anaerobic bacteria. High prevalence of antimicrobial resistance in rapidly growing mycobacteria in Taiwan. Antimicrobial susceptibility of clinical isolates of Bacteroides fragilis group organisms recovered from 2009 to 2012 in a Korean hospital. Antimicrobial susceptibility and synergy studies of Burkholderia cepacia complex isolated from patients with cystic fibrosis. Systematic review and meta-analysis of in vitro synergy of polymyxins and carbapenems. In doripenem, the dimethylcarbamoyl side chain of meropenem is replaced by a sulfamoylaminomethyl group (Jones et al. Doripenem is active against a broad range of Gram-positive and Gram-negative bacteria, including aerobes and anaerobes, but Mycoplasma spp. Doripenem received market authorization from the European Medicines Agency in 2008. Routine susceptibility the in vitro activity of doripenem is summarized in Table 39. In many Grampositive cocci susceptibility to doripenem is inferred from susceptibility to another beta-lactam agent (Staphylococcus spp. Doripenem has useful activity against Streptococcus pneumo niae and other streptococci, which includes alpha-hemolytic and beta-hemolytic streptococci. Doripenem has in vitro activity demonstrated against a number of Gram-positive bacilli, although the studies have been 723 724 Doripenem Table 39. In vitro susceptibility of selected Gram-positive organisms to doripenem Organism Aerococcus viridans Bacillus spp. Corynebacterium amycolatum Corynebacterium jeikeium Corynebacterium striatum Enterococcus faecalis Enterococcus faecium Enterococcus spp. Micrococcus luteus Nocardia brasiliensis Nocardia cyriacigeorgica Nocardia farcinica Rothia mucilaginosa Staphylococcus aureus, methicillin susceptible Staphylococcus aureus, methicillin-resistant Staphylococcus aureus, vancomycin intermediate Staphylococcus epidermidis, methicillin susceptible Staphylococcus epidermidis, methicillin resistant Staphylococcus haemolyticus Staphylococcus lugdunensis Staphylococcus coagulase negative, methicillin susceptible 0. Doripenem appears to have equivalent activity to meropenem against a variety of Nocardia spp. A number of anaerobic pathogens, including Clostridium perfringens, Propionibacterium spp. The susceptibility of other clinically relevant species, such as Peptostreptococcus spp. As a general rule, doripenem has excellent activity against all Enterobacteriaceae for which these strains do not harbor an acquired carbapenem-resistance mechanism. Citrobacter diversus Citrobacter freundii Elizabethkingia meningoseptica Enterobacter spp. Enterobacter aerogenes Enterobacter cloacae Enterobacter cloacae, cefotaxime resistant Enterobacter cloacae, AmpC derepressed Escherichia coli 1 0. Moraxella catarrhalis Neisseria meningitides Pantoea agglomerans Pasturella multocida Proteus mirabilis 0. Providencia rettgeri Providencia stuartii Providencia stuartii Indole positive Proteeae (P. In vitro susceptibility of selected anaerobes to doripenem Organism Aerococcus spp. Parvimonas micra Peptoniphilus asaccharolyticus Peptostreptococcus anaerobius Porphyromonas spp. The emerging issue of Enterobacteriaceae with acquired carbapenem resistance is in section 2b, Emerging resistance and cross-resistance. Of note, few isolates among these collections harbored a detectable carbapenemase enzyme, with a variety of other mechanisms accounting for the carbapenem resistance. Doripenem does not appear to have any enhanced in vitro activity against Acinetobacter spp. Of the commonly isolated anaerobes, carbapenem resistance is most described among Bacteroides spp. This, in turn, leads to a weakened cell wall, which eventually ruptures because of osmotic pressure forces (Stratton, 2005). Emerging resistance and cross-resistance Carbapenem resistance among Enterobacteriaceae is an emerging issue. The most significant mechanisms of resistance is due to bacterial production of a carbapenemase enzyme, a betalactamase able to hydrolyze carbapenem antimicrobials. Almost all of the currently prevalent carbapenemase enzymes will hydrolyze doripenem to a significant extent. Recent history demonstrates a rapidly changing epidemiology of carbapenemase enzymes. This is driven by the emergence of new mechanisms and/or the introduction and spread of carbapenemase enzymes into vulnerable populations (Nordman et al. In regard to other carbapenemase-encoding genes, the data on the specific impact on doripenem are more limited. In other markets, the product information recommends up to 1 g every 8 hours (Shionogi, 2013). Newborn infants and children Pediatric use of doripenem was approved in Japan in 2012 (Shionogi, 2013). There are a limited number of studies on the pharmacology and safety of doripenem in pediatric populations. There are no published clinical trials to support efficacy or specific indications for its use in the pediatric populations. Single-dose pharmacokinetics was investigated in 52 healthy infants < 12 weeks old. The agent was safe and well tolerated, with pharmacokinetics similar to other carbapenems (Cirillo et al. Clinical data and Monte Carlo simulation indicate an appropriate dose of 20 mg/kg every 8 hours (Matsuo et al. Unfortunately a series of three controlled clinical trials of doripenem in children (complicated intraabdominal infections, complicated urinary tract infection, pneumonia) across Europe and the Americas was stopped before completion for commercial reasons. Results have been published from the 88 children (66 received doripenem) enrolled in the trial, before its termination.
Generic 100mg januvia visa
Influence of outer membrane mutations on susceptibility of Escherichia coli to the dibasic macrolide azithromycin signs your diabetes is out of control order 100mg januvia free shipping. Influence of body weight, ethnicity, oral contraceptives, and pregnancy on the pharmacokinetics of azithromycin in women of childbearing age. The effects of an antacid or cimetidine on the serum concentrations of azithromycin. Short-course azithromycin for the treatment of uncomplicated typhoid fever in children and adolescents. Azithromycin versus ceftriaxone for the treatment of uncomplicated typhoid fever in children. Antimicrobial susceptibility testing of historical and recent clinical isolates of Bordetella pertussis in the United Kingdom using the Etest method. In vitro synergistic effects of double combinations of beta-lactams and azithromycin against clinical isolates of Neisseria gonorrhoeae. Lack of effect of zafirlukast on the pharmacokinetics of azithromycin, clarithromycin, and 14-hydroxyclarithromycin in healthy volunteers. Impact of mass azithromycin distribution on malaria parasitemia during the low-transmission season in Niger: a cluster-randomized trial. Community treatment with azithromycin for trachoma is not associated with antibiotic resistance in Streptococcus pneumoniae at 1 year. Maintenance azithromycin therapy for bronchiolitis obliterans syndrome: results of a pilot study. Efficacy of treatment with paromomycin, azithromycin, and nitazoxanide in a patient with disseminated cryptosporidiosis. Anticryptosporidial activity of ranalexin, lasalocid and azithromycin alone and in combination in cell lines. Enhanced efficacy of single-dose versus multi-dose azithromycin regimens in preclinical infection models. Effect of expedited treatment of sex partners on recurrent or persistent gonorrhea or chlamydial infection. In vitro antimicrobial susceptibility of Propionibacterium acnes isolated from acne patients in northern Mexico. Early results (at 6 months) with intermittent clarithromycin-including regimens for lung disease due to Mycobacterium avium complex. Initial (6-month) results of three-times-weekly azithromycin in treatment regimens for Mycobacterium avium complex lung disease in human immunodeficiency virus-negative patients. Macrolide and clindamycin resistance in Streptococcus milleri group isolates from the airways of cystic fibrosis patients. Pharmacokinetic and safety profile of desloratadine and fexofenadine when coadministered with azithromycin: a randomized, placebo-controlled, parallel-group study. Multicentre evaluation of azithromycin and penicillin V in the treatment of acute streptococcal pharyngitis and tonsillitis in children. In vitro activities of azithromycin, clarithromycin, L-ofloxacin, and other antibiotics against Chlamydia pneumoniae. Predictors of chronic obstructive pulmonary disease exacerbation reduction in response to daily azithromycin therapy. What is the appropriate treatment for the management of rectal Chlamydia trachomatis in men and women The decline of pneumococcal resistance after cessation of mass antibiotic distributions for trachoma. The transplacental transfer of the macrolide antibiotics erythromycin, roxithromycin and azithromycin. Randomized, controlled, double-blind trial of daily oral azithromycin in adults for the prophylaxis of Plasmodium vivax malaria in Western Thailand. A randomized, comparative pilot study of azithromycin versus benzathine penicillin G for treatment of early syphilis. Prediction of the in vivo interaction between midazolam and macrolides based on in vitro studies using human liver microsomes. Azithromycin is associated with increased survival in lung transplant recipients with bronchiolitis obliterans syndrome. Outcome of intravenous azithromycin therapy in patients with complicated scrub typhus compared with that of doxycycline therapy using propensity-matched analysis. Antibacterial susceptibility patterns of Porphyromonas gingivalis isolated from chronic periodontitis patients. Distribution of azithromycin into brain tissue, cerebrospinal fluid, and aqueous humor of the eye. Intermittent antibiotic therapy for nodular bronchiectatic Mycobacterium avium complex lung disease. In vitro synergism observed with azithromycin, clarithromycin, minocycline, or tigecycline in association with antifungal agents against Pythium insidiosum. Long-term morbidity and mortality after hospitalization with community-acquired pneumonia: a population-based cohort study. The effect of azithromycin on intracellular Legionella pneumophila in the Mono Mac 6 cell line at serum concentrations attainable in vivo. Investigation of developmental toxicity and teratogenicity of macrolide antibiotics in cultured rat embryos. Single dose azithromycin versus ciprofloxacin for cholera in children: a randomized controlled trial. Comparison of single-dose azithromycin and 12-dose, 3-day erythromycin for childhood cholera: a randomised, double-blind trial. Replacement of clarithromycin with azithromycin in triple therapy regimens for the eradication of Helicobacter pylori: A randomized clinical trial. A multicenter, randomized, open label comparison of azithromycin and amoxicillin/clavulanate in acute otitis media among children attending day care or school. Scrub typhus during pregnancy and its treatment: a case series and review of the literature. A comparative trial of a single dose of azithromycin versus doxycycline for the treatment of mild scrub typhus. In-vitro activity of azithromycin against various Gram-negative bacilli and anaerobic bacteria. Activities of azithromycin and clarithromycin against nontuberculous mycobacteria in beige mice. Azithromycin versus doxycycline for the treatment of genital chlamydia infection: a meta-analysis of randomized controlled trials. Mycoplasma pneumoniae and Chlamydia pneumoniae in asthma: effect of clarithromycin. Susceptibility of Candida albicans biofilms to azithromycin, tigecycline and vancomycin and the interaction between tigecycline and antifungals. Antimicrobial susceptibility of 800 anaerobic isolates from patients with dentoalveolar infection to 13 oral antibiotics. Previous antibiotic exposure and antimicrobial resistance in invasive pneumococcal disease: results from prospective surveillance. Factors related to response to intermittent treatment of Mycobacterium avium complex lung disease. In vitro activity of azithromycin and tetracycline against 358 clinical isolates of Brucella melitensis. Increased hypoprothrombinemic effect of warfarin possibly induced by azithromycin.
Buy januvia us
Linezolid solution can also be administered enterally in hospitalized patients without compromise of the bioavailability (Beringer et al chronic diabetes definition purchase januvia overnight delivery. Other studies have raised concerns about the adequacy of serum levels of linezolid in critically ill patients (Morata et al. A consistent finding has been that there are high levels of pharmacokinetic variability in the critically ill, both among patients and day to day in the same patient, meaning that this group is at risk of both overdosage and underdosage and would benefit from individualized dosing according to measured 5. Pharmacokinetics and pharmacodynamics 1309 Co-administration of oral linezolid with antacids (containing magnesium hydroxide and aluminum hydroxide) does not affect absorption of linezolid (Grunder et al. Oral bioavailability was also not affected after Roux-en-Y gastric bypass surgery (Hamilton et al. The protein binding of linezolid is about 31%, which is not concentration dependent (Clemett and Markham, 2000). During the linezolid compassionate use program, population pharmacokinetics were monitored in 318 patients (Meagher et al. There was significant variability in the pharmacokinetic patterns in different patients, with higher clearance and rates of metabolism than previously documented in healthy volunteers. Cystic fibrosis patients in particular can display pharmacokinetics that are different from those observed in the general population. Drug distribution the serum levels of linezolid in relation to dose are summarized in Table 73. Some studies to assess the pharmacokinetic features of linezolid used doses of 375 and 625 mg; therefore the data have been normalized for doses of 400 or 600 mg. Linezolid concentrations have been determined in a number of fluids both in healthy volunteers and in patients with clinical infections. The ratios of linezolid in saliva and sweat relative to plasma have been shown to be 1. The concentrations of linezolid at steady state have also been determined in interstitial fluid of critically ill patients (Buerger et al. Linezolid showed good penetration into the interstitial fluid; however, significant variability was noted. A more recent study found no significant difference in the pharmacokinetic profile of linezolid in plasma and interstitium based on the severity of sepsis (Thallinger et al. Linezolid concentrations have been determined in the pancreatic fluid of two patients with pancreatic abscess (Rao et al. Linezolid was detectable in drain fluid; in one patient the postdose level was 11 mg/l, and in the other patient it was 31. Penetration of linezolid into bile was assessed in two studies of liver transplant patients with biliary T-tubes in situ. The first assessed trough concentrations in the bile of six patients and found that levels were high, with a median concentration of 21. A single patient with cholecystostomy also had linezolid measured in bile: her lowest biliary trough level was 5. A critically unwell patient with an intraabdominal drain had linezolid levels measured in peritoneal drain fluid on day 7 of therapy with a concentration of 15. Based on limited data, in obese patients linezolid concentrations appear to be lower, associated with a higher volume of distribution (see section 4d, Those requiring altered dosages). The ratio of epithelial lining fluid and alveolar cell concentrations of linezolid compared with serum levels when measured at steady state were calculated as 4. In 10 patients undergoing bronchoscopy for diagnostic procedures, linezolid levels were measured after 600 mg every 12 hours for six doses (Honeybourne et al. In another study of patients with ventilatorassociated pneumonia, linezolid concentrations in epithelial lining fluid demonstrated a mean linezolid penetration of 100% (Boselli et al. Two studies assessed the penetration of linezolid into the epithelial lining fluid of critically unwell patients receiving continuous antibiotic infusion. In the first, 12 patients with ventilator-associated pneumonia received 600 mg of linezolid as a loading dose followed by 1200 mg/day by continuous infusion. At steady state, the median serum and epithelial lining fluid linezolid concentrations were 7. Epithelial lining fluid/plasma penetration ratio was slightly higher in the continuous infusion group (106% vs. Overall, the penetration was similar to that reported in the previous studies described. Sputum penetration of linezolid has also been determined in cystic fibrosis patients and was found to be good, with a mean sputum concentration of 17. Penetration of linezolid into the pleural and mediastinal spaces was measured in two patients undergoing coronary artery bypass graft surgery, who had postoperative drains in situ. In 14 neurosurgical patients being treated with 600 mg intravenously every 12 hours, mean Cmax and Cmin linezolid levels in serum were 18. The mean ratio of linezolid concentration in aqueous humor to that in serum was 0. In patients undergoing vitrectomy, mean aqueous, vitreous, and serum levels were 6. This was exceeded by the vitreous concentration, measured 12 hours after two oral doses (4. The ratio of vitreous/ serum concentration increased over time, from an average 0. In a rabbit study of the ocular penetration of linezolid applied topically in the form of drops, concentration in the aqueous humor reached a mean peak of 0. In rabbits that received multiple doses (100 g every 15 minutes for a total of four doses), mean peak aqueous concentration was 2. In a third set of rabbits that received the multi-dose protocol and then had eye tissue harvested, the mean concentration at 1 hour was 4. This favorable result is supported by human case reports of successful treatment of keratitis with topical linezolid (see section 4, Mode of drug administration and dosage-Adults). Linezolid concentrations were measured in interstitial space fluid of healthy volunteers at steady state (Dehghanyar et al. Linezolid concentrations were measured in 12 patients undergoing total hip replacement after a single infusion of linezolid 600 mg (Lovering et al. High concentrations of linezolid were found in bone within 10 minutes (mean concentration 9. Linezolid concentrations have been shown to be high in infected tissues around joint prostheses (Kutscha-Lissberg et al. In 10 patients undergoing total knee replacement, linezolid was administered for 48 hours preoperatively at 600 mg every 12 hours. Several studies have assessed the penetration into the potentially poorly perfused bone and tissue involved in diabetic foot infections, with some variability in results. Mean peak concentrations of free linezolid in plasma, healthy subcutis, inflamed subcutis, and cancellous bone (metatarsal) were 16. Therefore, eventual penetration of linezolid into inflamed diabetic foot infection tissue does not seem significantly impaired, but time to tissue 1312 Linezolid equilibration with plasma may be delayed (Eslam et al. Six patients with mild diabetic foot infections received treatment with oral linezolid 600 mg twice daily. After multiple doses, serum and foot tissue linezolid concentrations were measured; tissue concentrations ranged from 15. For example, after oral administration of linezolid 600 mg, at steady state mean Cmax has ranged from 16. More pronounced variability was observed in the population pharmacokinetic monitoring of the linezolid compassionate use program (Meagher et al. Other clinical scenarios have also raised concern about the adequacy of linezolid serum concentrations, such as critically ill patients in the intensive care unit and morbidly obese patients (Adembri et al.
Syndromes
- Before birth, the baby has a blood vessel that runs between the aorta (the main artery to the body) and the pulmonary artery (the main artery to the lungs), called the ductus arteriosus. This opening usually closes shortly after birth. A PDA occurs when this opening does not close after birth.
- Blood sugar levels (to diagnose hyperglycemia)
- Blockage
- Decreased breath sounds
- Time it was swallowed
- Allergies to plants and other substances
- Lung collapse
- Changes in female body contours
- Bleeding
- Is the pain constant or does it come and go?

Buy januvia without a prescription
Drug-induced lifethreatening potassium disturbances detected by a pharmacovigilance program from laboratory signals blood sugar range after eating purchase genuine januvia on-line. A randomized double-blind trial of vancomycin versus teicoplanin for the treatment of Grampositive bacteremia in patients with cancer. Teicoplanin pharmacodynamics in reference to the accessory gene regulator (agr) in Staphylococcus aureus using an in vitro pharmacodynamic model. Randomized comparison of serum teicoplanin concentrations following daily or alternate daily dosing in healthy adults. Teicoplanin pharmacokinetics in intravenous drug abusers being treated for bacterial endocarditis. Daptomycin antimicrobial activity tested against methicillin-resistant staphylococci and vancomycin-resistant enterococci isolated in European medical centers (2005). Comparative efficacy of teicoplanin and cefazolin for cardiac operation prophylaxis in 3027 patients. Comparison of vancomycinand teicoplanin-induced histamine release and "red man syndrome". Efficacy of teicoplanin and autoradiographic diffusion pattern of [14C]teicoplanin in experimental Staphylococcus aureus infection of joint prostheses. Recommended initial loading dose of teicoplanin, established by therapeutic drug monitoring, and outcome in terms of optimal trough level. Significance of high trough concentration of teicoplanin in the treatment of methicillin-resistant Staphylococcus aureus infection. Teicoplanin alone or combined with rifampin compared with vancomycin for prophylaxis and treatment of experimental foreign body infection by methicillin-resistant Staphylococcus aureus. Cost effectiveness of teicoplanin plus ceftriaxone: a once daily antibiotic regimen. Loading regimen required to rapidly achieve therapeutic trough plasma concentration of teicoplanin and evaluation of clinical features. Comparison of intravenous teicoplanin with intramuscular amoxycillin for the prophylaxis of streptococcal bacteraemia in dental patients. Complete heart block in a patient with acute lymphoblastic leukaemia: teicoplanin as a possible cause and review of literature. Elimination of teicoplanin by adsorption to the filter membrane during haemodiafiltration: screening experiments for linezolid, teicoplanin and vancomycin followed by in vitro haemodiafiltration models for teicoplanin. Teicoplanin-resistant Staphylococcus aureus expresses a novel membrane protein and increases expression of penicillin-binding protein 2 complex. More accurate measurement of vancomycin minimum inhibitory concentration indicates poor outcomes in methicillin-resistant Staphylococcus aureus bacteraemia. Randomized prospective study comparing vancomycin with teicoplanin in the treatment of infections associated with Hickman catheters. Pharmacokinetics of teicoplanin upon multiple-dose intravenous administration of 3, 12, and 30 milligrams per kilogram of body weight to healthy male volunteers. Poor penetration of teicoplanin into cerebrospinal fluid in patients with bacterial meningitis. Pharmacokinetics of teicoplanin in patients undergoing continuous ambulatory peritoneal dialysis. Teicoplanin for skin and soft tissue infections: an open study and a randomized, comparative trial versus cefazolin. Comparative efficacy and safety of vancomycin versus teicoplanin: systematic review and meta-analysis. In vitro efficacy of fosfomycincontaining regimens against methicillin-resistant Staphylococcus aureus in biofilms. Treatment of Clostridium difficile-associated diarrhea and colitis with an oral preparation of teicoplanin; a dose finding study. Pharmacokinetics of teicoplanin upon multiple dose intravenous administration to normal healthy male volunteers. Prophylaxis with teicoplanin and cefuroxime reduces the rate of prosthetic joint infection after primary arthroplasty. Teicoplanin and rifampicin singly and in combination in the treatment of experimental Staphylococcus epidermidis endocarditis in the rabbit model. The effects of hypoalbuminaemia on optimizing antibacterial dosing in critically ill patients. Randomized study of vancomycin versus teicoplanin for the treatment of Gram-positive bacterial infections in immunocompromised hosts. Prophylactic antibiotics for preventing early Gram-positive central venous catheter infections in oncology patients, a Cochrane systematic review. Perioperative anti-infective prophylaxis with teicoplanin compared to cephalosporins in orthopaedic and vascular surgery involving prosthetic material. Four-week treatment of streptococcal native valve endocarditis with high-dose teicoplanin. Antimicrobial susceptibilities of enterococci isolated from hospitalized patients. Interactions between glycopeptides and beta-lactams against isogenic pairs of teicoplanin-susceptible and -resistant strains of Staphylococcus haemolyticus. Loading dose required to achieve rapid therapeutic teicoplanin trough plasma concentration in patients with multidrug-resistant gram-positive infections. Prognosis of patients with methicillin-resistant Staphylococcus aureus bloodstream infection treated with teicoplanin: a retrospective cohort study investigating effect of teicoplanin minimum inhibitory concentrations. In-vitro induction of resistance in coagulasenegative staphylococci to vancomycin and teicoplanin. Linezolid compared with teicoplanin for the treatment of suspected or proven Gram-positive infections. Serum and tissue levels of teicoplanin during cardiac surgery: the effect of a high dose regimen. Antibiotic prophylaxis in cardiac surgery: a prospective comparison of two dosage regimens of teicoplanin with a combination of flucloxacillin and tobramycin. Stevens-Johnson syndrome induced by the cross-reactivity between teicoplanin and vancomycin. Variability in teicoplanin protein binding and its prediction using serum albumin concentrations. Multicenter prospective observational study of the comparative efficacy and safety of vancomycin versus teicoplanin in patients with health care-associated methicillinresistant Staphylococcus aureus bacteremia. Population pharmacokinetics and dosing optimization of teicoplanin in children with malignant haematological disease. The initial development program started in the 1980s was terminated owing to treatment failures in endocarditis with 2 mg/kg and the occurrence of potential drug-induced myopathy. The official dosage recommendations are 4 mg/kg or 6 mg/kg once daily; however, currently much higher doses are used in clinical practice. It is a cyclic lipopeptide comprising 13 amino acids with a water-soluble hydrophilic core and a lipophilic tail. The mechanism of action depends on a fast depolarization of the bacterial cytoplasmic membrane, resulting in a rapid concentration-dependent bactericidal effect. Despite the fact that daptomycin is only effective against Gram-positive microorganisms, the drug has been evaluated in combinations with other antibiotics for Gram-negative pathogens. Several studies indicate enhanced activity of colistin when combined with daptomycin for Acinetobacter baumannii (Phee et al. Another study showed some synergistic effect when daptomycin was added to aztreonam or ceftazidime (LaPlante and Sakoulas, 2009). Susceptibility data against anaerobic Gram-positive bacteria and unusual species are shown in Table 45. Although streptococcal susceptibility to daptomycin is favorable compared with most antibiotics that are active against Gram-positive bacteria, one should keep in mind that penicillin (see Chapter 3, Benzylpenicillin [Penicillin G]) 868 Daptomycin Table 45. Daptomycin current Clinical & Laboratory Standards Institute breakpoints (mg/l) indicating susceptibility to S. Antimicrobial activity of daptomycin against Gram-positive anaerobic bacteria, Corynebacteria, and unusual Gram-positive bacteria.
Order januvia with mastercard
After oral dosing metabolic disease ketonuria januvia 100 mg low cost, a very high concentration was achieved in pulmonary, prostatic, epididymal, tonsillar, and skin tissue, tear fluid and aqueous humor, as well as periodontal and synovial tissues. No dosage adjustment is needed in patients with cirrhosis (Periti and Mazzei, 1987; Puri and Lassman, 1987). In patients with alcoholic cirrhosis, the increase in renal clearance of roxithromycin offsets the reduction in hepatic clearance, and no dosage modification is considered necessary in most patients (Periti and Mazzei, 1987). Dosage adjustment for roxithromycin is usually not required with conventional doses, but closer than usual clinical monitoring of the older patient has been advocated (Periti et al. Roxithromycin accumulates in the cells to higher levels than erythromycin (Carlier et al. Roxithromycin is concentrated in human monocytes (Hand and King-Thompson, 1989), neutrophils, and macrophages (Labro et al. Drugs to use with caution (require dose reduction and/or a therapeutic monitoring) Benzodiazepines Bromocriptine Theophylline Digoxin Fentanyl Adapted with permission from Periti et al. Contraindicated drugs Astemizole Cisapride Ergotamine and ergot derivatives Terfenadine 5c. The high level of tissue diffusion is considered an advantage for the treatment of serious infections, including those in the respiratory tract; however, increasing rates of resistance in some regions limit the use of roxithromycin in some countries (Bergogne-Berezin, 1987; Chastre et al. However, conclusions with respect to tissue concentrations should be drawn with great caution (Mouton et al. Conversely, co-administration of inducers of cytochrome P4503A4, such as rifampicin or rifabutin, may cause a reduction in macrolide plasma levels, which can lead to therapeutic failure or to selection of resistant strains. Roxithromycin does not influence the pharmacokinetics of lovastatin, such that no dosage alteration is needed when these agents are given concomitantly (Bucher et al. Excretion Liver metabolization of roxithromycin is limited (~25% of the dose), the main metabolite being the decladinose derivative (Puri and Lassman, 1987; Zhong et al. About 30% of the drug eliminated in the feces consists of inactive metabolites (Periti and Mazzei, 1987; Puri and Lassman, 1987). Gastrointestinal adverse effects Gastrointestinal adverse effects are the most common side effects (Periti et al. In adults, the gastrointestinal tolerance of roxithromycin compares favorably with those of doxycycline and erythromycin ethylsuccinate. Roxithromycin therapy has caused vomiting in a few children (Kafetzis and Blanc, 1987). Drug interactions Drug interactions with macrolides can be a significant problem, which in some cases can seriously limit their use in at-risk patients. The main mechanism involved in these interactions is the ability of macrolides to bind to cytochrome P450 (group 3A4), thereby impairing the subsequent metabolization of other substrates of the same cytochrome (Periti et al. The elimination of these drugs when co-administered is therefore reduced, causing a potential risk of toxicity (Periti et al. Although roxithromycin is a 14-membered lactone ring macrolide, it is unlike erythromycin in that it does not interfere with the metabolism of theophylline and carbamazepine 6b. Concomitant acute renal failure and hepatotoxicity have been associated with roxithromycin therapy (Akcay et al. Hypersensitivity reactions Allergic reactions, including eosinophilia, fever, and skin eruptions, are rarely reported for macrolides. Other adverse reactions Reversible and mild itching and headache are other side effects observed in more than 1% of patients (Worm et al. In those countries where roxithromycin is used regularly, it is generally for respiratory tract infections, especially mild to moderate cases of community-acquired pneumonia, often in combination with a beta-lactam agent. Respiratory tract infections Roxithromycin is an alternative to erythromycin for the treatment of pharyngitis. In patients with group A betahemolytic streptococcal pharyngitis, its efficacy is similar to or inferior to that of erythromycin (Herron, 1987; Melcher et al. Roxithromycin has been effective in the treatment of sinusitis, otitis media, bronchitis, and pneumonia caused by pathogens such as S. Outcomes were similar with clinical cures/improvements of 82% and 78%, respectively (Mira and Benazzo, 2001). Roxithromycin (150 mg daily for three months) appears to be more effective than placebo in the treatment of chronic rhinosinusitis (Wallwork et al. Macrolides have long been considered as an alternative to beta-lactams for the treatment of respiratory tract infections. However, the increasing rates of resistance to macrolides among common respiratory pathogens, other than Myco plasma and Chlamydophila spp. In addition, the beneficial effects of macrolides in the treatment of mild respiratory infections are increasingly being questioned. Compared with broad-spectrum fluoroquinolones, roxithromycin appears less effective in the treatment of respiratory infections. Skin infections Roxithromycin can be effective for impetigo and erysipelas caused by susceptible S. However, roxithromycin in these scenarios offers little advantage over clarithromycin or azithromycin (Parsad et al. A 4-week administration of roxithromycin proved effective in decreasing inflammatory acne (Ferahbas et al. Lyme disease Limited data suggest that roxithromycin can be effective against borreliosis and Lyme arthritis (Pedersen and FriisMoller, 1991), but therapeutic failures have also been reported (Weber, 1996). The efficacy is much lower than would be anticipated based on in vitro susceptibility data (Hansen et al. Overall, macrolides, including roxithromycin, are considered second-line therapy behind beta-lactams and tetracyclines for this disease owing to their lower rates of efficacy (Loewen et al. Other authors have also used a quinolone, such as ciprofloxacin, plus roxithromycin as chemoprophylaxis in neutropenic patients with some success (Verhoef, 1993). Sexually transmitted diseases In the treatment of nongonococcal urethritis in males, roxithromycin in a dosage of 150 mg every 12 hours cured 97% of C. Chlamydial conjunctivitis in newborns and adults has also been treated with some success with oral roxithromycin (Stenberg and Mardh, 1991). Coronary artery and other arteriovascular diseases Chlamydia pneumoniae has been found present in atherosclerotic lesions and therefore is suggested to play a role in cardiovascular diseases. Macrolides have been theorized to play a protective role against coronary artery disease, as a result of their antichlamydial or anti-inflammatory effect on atheromata. Studies with roxithromycin for this indication yield contradictory results (Gurfinkel et al. Until recently, no large randomized trials centering on coronary artery disease had been conducted with roxithromycin (Muhlestein, 2003), but studies with azithromycin (Grayston et al. A meta-analysis of studies examining potential macrolide benefit in the secondary prevention of coronary artery disease did not support the routine use of anti-chlamydial therapy (Etminan et al. Among the 868 patients followed up at 12 months, there was no difference in mortality (6. Roxithromycin was shown to be less effective than clarithromycin in one triple-therapy study (Svoboda et al. In a quadruple-therapy study of omeprazole, amoxicillin, metronidazole, and roxithromycin, however, cure rates were as high as 95% (Okada et al. Chemoprophylaxis in neutropenic patients In a prospective, randomized, open trial, the efficacy of oral roxithromycin (150 mg 12-hourly) as additional chemoprophylaxis on top of ofloxacin was evaluated in 131 adult patients with acute leukemia or receiving adult bone marrow transplants. Relative to patients given ofloxacin alone, fewer patients receiving both drugs developed bacteremia caused by S.
Purchase discount januvia on-line
A 14-year-old child developed recurrent acute interstitial nephritis induced by azithromycin administration (Soni et al diabetes mellitus type 2 bmj best januvia 100 mg. Azithromycin rarely causes neuropsychiatric effects including delirium, catatonia, hallucinations (Schiff et al. Data suggest that the infant gut is particularly affected by macrolides during the first 2 weeks of life. A potential mechanism for the gastrointestinal effects is macrolide-induced endogenous release of motilin, which stimulates motilin receptors and has a prokinetic effect on the gut. Azithromycin has a number of indications, particularly for respiratory tract infections, where macrolides have long been considered an alternative to beta-lactams. However, the increasing rates of macrolide resistance, particularly among respiratory pathogens (see section 2bm Emerging resistance and cross-resistance), require some caution by physicians when prescribing, such that macrolide usage for these indications should be limited to countries where resistance rates remain low. In addition, chronic use of macrolides for their immunomodulatory properties needs to be balanced with the increased risk of selection of macrolide-resistant bacteria at both the individual and population level. In rat embryo models, macrolides significantly inhibited all growth and developmental parameters dose dependently, compared with controls (Karabulut et al. Clarithromycin caused more developmental toxicity, whereas azithromycin had more teratogenicity potential and spiramycin had the lowest levels of toxic and teratogenic effects observed. Observational studies have suggested that gestational exposure to azithromycin is not associated with an increased risk of congenital malformations (Bar-Oz et al. Upper respiratory tract infections Azithromycin is proposed as second-line therapy and in penicillin-allergic patients for tonsillopharyngitis in children and adults. Azithromycin (10 mg/kg/day for 3 days during each of 3 consecutive weeks) may be considered for the eradication of atypical organisms (M. Oral azithromycin is equivalent to intravenous cefazolin for preventing surgical site infection in patients undergoing tonsillectomy (Otake et al. Azithromycin is indicated in the treatment of acute otitis media (in children) and acute sinusitis caused by S. Azithromycin 500mg once per week for 3 months may benefit patients with chronic sinusitis without nasal polyps (Rudmik and Soler, 2015). Lower respiratory tract infections Azithromycin is indicated for acute exacerbations of chronic bronchitis caused by S. A 3-day course of azithromycin is as effective and well tolerated as a 10-day course of clarithromycin for treating lower respiratory tract infections (Bradbury, 1993). In patients with acute bronchitis of a suspected bacterial cause, azithromycin tended to be more efficacious than amoxicillin or amoxiclav. In clinical practice, the choice of azithromycin versus amoxicillin or amoxiclav is often based on considerations such as cost, convenience, and treatment compliance. Two randomized studies have compared azithromycin versus levofloxacin or moxifloxacin in the treatment of acute exacerbations of chronic bronchitis. Clinical resolution rates were 88% for moxifloxacin and 86% for azithromycin, with similar bacteriologic eradication rates: 95% for moxifloxacin and 94% for azithromycin, although the H. However, it should be noted that a dosing regimen of azithromycin 500 mg initially, followed by 250 mg for 4 days, was ineffective for eradicating H. However, there is insufficient evidence to support the use of antibiotic therapy in mild exacerbations (Vollenweider et al. In comparison, guidelines from Europe recommend amoxicillin or penicillin for the same indication (Lim et al. The presence of comorbidities, such as chronic heart disease, lung, liver, or renal disease, or diabetes mellitus, or alcoholism, malignancy, asplenia, immunosuppressing conditions, or the use of immunosuppressant drugs, requires the use of a respiratory fluroquinolone or a beta-lactam plus azithromycin (Mandell et al. Among older patients hospitalized with pneumonia, antimicrobial therapy that included azithromycin (compared to other antibiotic therapy) was associated with reduced 90-day mortality (Mortensen et al. For patients requiring intensive care admission, guidelines recommend a minimum of a beta-lactam plus a macrolide or a quinolone (Mandell et al. Antibiotics with antiinflammatory properties, such as the tetracyclines and macrolides, are the agents of choice for pustulopustular acne (Sandoval et al. Following the success of azithromycin for the treatment of syphilis, a single dose of oral azithromycin 30 mg/kg was compared to the standard intramuscular 50 000 units/kg benzathine benzyl penicillin for the treatment of yaws in children, and found to be noninferior (Mitja et al. In a subsequent study, mass treatment with single dose azithromycin reduced the prevalence of active yaws from 2. This study suggests that an integrated approach to the control of yaws and trachoma may be possible in co-endemic areas. Pertussis Azithromycin is preferred for the treatment of pertussis in patients aged < 1 month, and is an alternative to other macrolides in older children and adults, although data on the safety and efficacy of azithromycin use among infants aged < 6 months are limited (Salim et al. For postexposure prophylaxis, the benefits of administering an antimicrobical agent to reduce the risk of pertussis should be weighed against the potential adverse effects of the drug. The recommended antimicrobial agents and dosing are the same as those for the treatment of pertussis. Skin and skin structure infections Azithromycin is indicated for uncomplicated skin and skin structure infections due to S. Doxycycline-resistant strains of Orientia tsutsugamushi remain susceptible to azithromycin in vitro (Strickman et al. A randomized trial demonstrated that azithromycin for 3 days (1 g initially, followed by 500 mg once daily for 2 days) (Phimda et al. A single 500 mg dose of azithromycin may also be efficacious in mild scrub typhus (Kim et al. A retrospective, propensity score-matched, case-control study of patients with severe or complicated scrub typhus showed that azithromycin was as efficacious as doxycycline (Jang et al. Doxycycline is not recommended in children under 8 years and azithromycin is considered a safe and efficacious treatment option in this age group (Palanivel et al. Azithromycin is commonly used as an alternative to doxycline for scrub typhus in pregnancy although evidence supporting its use is limited (Kim et al. In a small randomized trial, azithromycin treatment led to lymph node regression at 30 days more frequently than placebo (Bass et al. Erythromycin or doxycycline is recommended for the treatment of bacillary angiomatosis (Stevens et al. Azithromycin is an appropriate option for tularemia during pregnancy in regions where the infecting strains of Francisella tularensis have no natural resistance to macrolides (Dentan et al. North American strains are generally sensitive to macrolides, in contrast to European isolates (Johansson et al. Azithromycin may be used for the treatment of toxoplasmosis, particularly in immunocompetent patients (Wei et al. Azithromycin treatment of toxoplasmosis during pregnancy can reduce the sequelae rate among infected infants at 1 year of age (Foulon et al. Guidelines recommend either single-dose azithromycin (1 g) or doxycycline (100 mg twice daily for 7 days) for the treatment of uncomplicated chlamydial genital or pharyngeal infection, although single-dose regimes have improved compliance (Alliance, 2015; Lanjouw et al. A 2002 meta-analysis of randomized controlled trials reported a similar cure rate for azithromycin compared to doxycycline (98% vs. Nearly all of the studies in the meta-analysis used culture or immunoassay to determine microbiological cure rates. Subsequent evidence has led to questioning of the efficacy of azithromycin for the treatment of urogenital chlamydial infections. A partner treatment study of persons treated with azithromycin found that among women who reported having no sex after treatment, 8% had persistent infection at follow-up (Golden et al.
Order januvia 100mg
Daptomycin (6 and 12 mg/kg/day) with and without 2 g of ceftriaxone every 24 hours was evaluated diabetes signs wiki cheap 100 mg januvia overnight delivery. Daptomycin (6 mg/kg) with ceftriaxone and daptomycin (12 mg/kg) alone and in combination with ceftriaxone displayed significantly more activity than daptomycin (6 mg/ kg) alone from 48 to 96 hours (p 0. The addition of ceftriaxone significantly enhanced the activity of daptomycin (6 mg/kg) against both strains and improved the activity of daptomycin (12 mg/kg) against one of the two strains at 96 hours. The combination of daptomycin with oxacillin improved the activity as compared with daptomycin monotherapy (doses equal to human doses of 6 mg/kg) as well (Yang et al. More data, especially clinical, are needed to conclude whether this combination is beneficial. The combination of daptomycin plus ceftaroline also resulted in enhanced killing over monotherapy of one of the drugs in an in vitro endocarditis model with simulated endocardial vegetations (Werth et al. An antagonistic effect between daptomycin and rifampicin and gentamicin has been shown. Clinical uses of the drug 893 regimens had more activity compared with the vancomycincontaining regimens (p = 0. Adding rifampicin or gentamicin to the daptomycin antagonized or delayed the bactericidal effect of daptomycin within the first 24 hours after start of treatment (LaPlante and Woodmansee, 2009). These results were supported by another study in rats showing that the combination of daptomycin with gentamicin was as effective in reducing the density of bacteria in valve vegetations as was daptomycin alone (p = 0. The combination of daptomycin with rifampicin was less effective than daptomycin alone (p < 0. A high incidence of renal dysfunction was attributed to the addition of gentamicin for the first 4 days of therapy in the comparator group, who received vancomycin and/or betalactam therapy (Fowler et al. First, although this trial was randomized, it was open label with a blinded assessment of the clinical outcome. Thus although bias in assessing treatment efficacy may have been controlled, bias in reporting and acting on adverse events was not. Second, the study population was rather heterogeneous-a key focus of the study was staphylococcal endocarditis, yet only 29% (53 of 181) of patients who were initially thought to have endocarditis at enrollment were confirmed to have this as a final diagnosis, with a wide variety of nonendocarditis etiologies identified. Although the study aimed to recruit 90 evaluable patients in each treatment arm (to assess a potential treatment difference [delta] of 20%), only 79 (daptomycin) and 60 (comparator) patients were fully evaluable, and, surprisingly, at least one patient who did not have S. Key outcomes of "clinical failure" and "microbiological failure" were not clearly described, and the definitions of complicated endocarditis and bacteremia were perplexing. Thus clinicians using this agent should be aware that if patients appear to be failing treatment, the emergence of resistance should be carefully assessed. Compared with vancomycin, the use of daptomycin was not significantly associated with treatment failure. These studies all reported a better outcome for daptomycin compared with vancomycin (Moore et al. The rate of clinical failure at 30 days was significantly lower in the daptomycin arm compared with the vancomycin arm (20. Both 30-day mortality and persistent bacteremia were significantly lower in the daptomycin group compared with the vancomycin group (3. In all retrospective studies, many patients treated with daptomycin were previously treated with vancomycin. Overall treatment success was 86% (n = 225/262), 894 Daptomycin and treatment success for patients taking concomitant betalactams was 86% (n = 105/122). The entry criteria for the studies differed, but all three meta-analyses suggested a survival benefit of linezolid over daptomycin. In addition, significant methodological limitations to the underlying literature have been identified in these studies. The limitations of prior studies included variable case definitions, limited sample size, heterogeneous patient populations, wide variation in outcome measures, insufficient daptomycin dosing, and documented but unadjusted treatment selection bias (McKinnell and Arias, 2015). A relatively large retrospective study (N = 644) has also been performed comparing daptomycin (6 mg/kg) and linezolid, but it reported opposite results (Britt et al. Although this study has been performed on patients treated only with daptomycin or linezolid-not those who received sequential treatment- there might be some bias between the treatment groups. The cohort of patients treated with linezolid may actually have been sicker than patients treated with daptomycin (McKinnell and Arias, 2015). Therefore, a definite conclusion for the comparison between daptomycin and linezolid cannot be drawn. The overall sustained clinical success rate in patients followed for up to 2 years was 86. Two studies in patients with endocarditis compared daptomycin with standard care, and the results were in disagreement. Adding ceftaroline to daptomycin, as has been suggested in in vitro studies (Barber et al. Daptomycin has not been studied in patients with prosthetic valve endocarditis (Package Insert, 2007). All patients with nonsusceptible isolates relapsed or failed therapy (Sharma et al. A patient with native valve endocarditis caused by a vancomycin "heteroresistant" strain of E. The infecting organism exhibited in vivo emergence of a vancomycin-susceptible subpopulation lacking the vanA gene cluster. Treatment with a combination of high-dose daptomycin, gentamicin, and high-dose ampicillin cleared the infection (Arias et al. Antibiotic activity depends on biofilm maturity and bacterial strain (Bauer et al. However, studies with combinations of antibiotics indicate that the activity of daptomycin on S. Time-kill studies indicate that daptomycin plus rifampicin was superior over vancomycin plus rifampicin for E. One study showed the effect of daptomycin alone or combined with azithromycin on S. Daptomycin alone at concentrations of 2 mg/l and 5 mg/l had no effect on the biofilm, and the addition of azithromycin also had no effect (Presterl et al. The low dosage of daptomycin was the least effective treatment and did not protect against the emergence of resistant strains. There were no differences between the two dosages of daptomycin plus cloxacillin in any situation, and both protected against resistance. The overall effect of the addition of cloxacillin to daptomycin was a significantly greater cure rate (against adhered bacteria) than that for daptomycin alone. Daptomycin doses that were equal to human doses of 6 mg/kg and 10 mg/kg were used. Daptomycin monotherapy 896 Daptomycin performed better than vancomycin and linezolid. In combination with rifampicin, both dosages of daptomycin were significantly better than the combinations with vancomycin and better than monotherapy. The human-simulated 10 mg/ kg dose achieved better cure rates at 11 days compared with the human-simulated 6 mg/kg dose (p < 0. Compared with vancomycin, daptomycin was more active, and the addition of gentamicin resulted in a more pronounced increase in cure rate in the daptomycin group (Furustrand Tafin, 2011). The difference in effect between the endocarditis model and the foreign-body model might be due to the infecting microorganism or to the model or type of infection itself. Vancomycin and daptomycin as single therapies were ineffective, but both combinations were significantly more effective than the corresponding monotherapy.
Discount 100 mg januvia fast delivery
Therefore diabetes insipidus urine output buy januvia 100mg low price, specific testing for resistance to minocycline could be warranted for certain pathogens (Chopra and Roberts, 2001). Resistance now occurs in increasing numbers of bacteria, which limits the use of antimicrobial agents. The values are condensed from studies in which the majority of organisms tested were isolated from patients, and therefore include strains with acquired tetracycline resistance. Overview of the susceptibility of various pathogens that are clinically relevant for minocycline use. Recent studies suggest reasonable in vitro activity against some strains of Acinetobacter baumannii, and clinical studies using minocycline in combination with other agents (especially carbapenems) have shown efficacy of the combined therapies against Gram-negative rods in some cases (see section 7, Clinical uses of the drug) (Tan et al. Some strains of Stenotrophomonas maltophilia and Aeromonas hydrophila are inhibited by clinically attainable concentrations of minocycline (Petersen et al. Against a number of specific clinical pathogens, including Burkholderia pseudo mallei (Thibault et al. In vitro, a synergistic inhibitory effect on Vibrio chol erae has been noted with cefazoline or cefotaxime in combination with minocycline, although the clinical relevance of this observation is uncertain (Su et al. Although minocycline has been noted to have some in vitro antiviral activity against various viruses in some animal models, this has little clinical relevance (Nagarakanti and Bishburg, 2016). Similar to corticosteroids, minocycline should not be given to patients with suspected rabies due to concerns about aggravating the disease (Appolinario and Jackson, 2015). Minocycline is active against a variety of intracellular microorganisms, including Mycoplasma pneumoniae (Ikejima et al. A recent review suggested that this in vitro activity is supported by reasonable clinical activity against these pathogens when minocycline has been used instead of doxycycline (Carris et al. These genes code either for efflux pump proteins or ribosomal protection proteins. Most of the efflux proteins confer resistance to tetracycline, but not to minocycline, with the exception of the protein coded by the Gram-negative tet(B) gene, which confers resistance to both, as do the ribosomal protection proteins. Ribosomal protection genes have now been identified in Gram-positive and Gram-negative pathogens (Beabout et al. Susceptibility patterns of clinical isolates vary from region to region (Hoban et al. Although minocycline is a commonly used agent for acne (see section 7, Clinical uses of the drug), resistance rates as high as 25% have been reported for propionibacteria. These resistance rates are owing to mutations rather than the acquisition of tet genes (Ross et al. Resistance to tetracyclines in general is discussed more extensively in the tetracycline and doxycycline chapters (Chapter 57, Tetracycline; Chapter 68, Doxycycline). Minocycline shows some activity against various protozoan parasites, such as Toxoplasma gondii, Giardia lamblia, Tricho monas vaginalis, Leismania major, and Entamoeba histolytica (Edlind, 1989; Chang et al. Minocycline is more lipophilic than tetracycline and this may improve its penetration into the cells of these parasites (Katiyar and Edlind, 1991). In a recent study assessing the pharmacokinetics and anti-Wolbachia efficacy in a murine Brugia malayi model of minocycline versus doxycycline, minocycline was thought to deplete Wolbachia more effectively than doxycycline (99. This may have relevance to the treatment of lymphatic filariasis and onchocerciasis (both parasitic helminth diseases which cause severe morbidities such as elephantiasis, skin disease, and blindness), since targeting the endosymbiotic bacterium, Wolbachia, may deliver macrofilaricidal activity and a block in microfilarial production (Sharma et al. The binding is reversible, providing an explanation of the bacteriostatic effect of the tetracyclines (Chopra et al. Additionally, tetracyclines inhibit protein synthesis in mitochondria through their binding to 70S ribosomes, which explains their antiparasitic activity in protozoa-containing mitochondria. A number of protozoa lacking mitochondria, nevertheless, are susceptible to tetracyclines (Endlind, 1991). Tetracyclines may also cause alterations in the cytoplasmic membrane, thereby allowing leakage of nucleotides and other compounds from the cell. In addition, tetracyclines appear to inhibit adhesion of bacteria to human cell surfaces and so render the bacteria less pathogenic. These drugs probably inhibit the synthesis of a specific protein that becomes embedded in the bacterial cell surface (Chopra and Hacker, 1986; Schifferli and Beachey, 1988). Pregnant and lactating mothers As with other tetracyclines, minocycline should be avoided in pregnancy. The oral formulation is available as a capsule, a coated tablet (containing 50 or 100 mg), and as powder for suspension. For periodontal disease and acne, respectively, microspheres and extended-release capsules have been developed (Song et al. Adults the oral dosage for adults consists of an initial loading dose of 200 mg followed by a maintenance dose of 100 mg every 12 hours. The adult dosage of the drug is 200 mg initially, followed by 100 mg every 12 hours. Each dose has to be dissolved in 500 or 1000 ml of glucose or saline fluid for slow i. Because only a small amount of the drug is excreted in urine, it could be expected that only minor dosage adjustments are required in patients having impaired renal function. Some investigators found that minocycline excretion was not significantly reduced in patients with renal failure and that minocycline did not accumulate in the serum (Carney et al. Although these results suggested that minocycline may be used safely in the presence of mild renal failure, the drug should be used cautiously. An increase of catabolic activity has been reported in patients with endstage renal disease and in healthy subjects after the administration of large doses (Devulder et al. The normal recommended dose per day should not be exceeded, because the protein catabolic effect of the drug is dose-dependent. In patients with renal impairment, a resultant small increase in urea production may be sufficient to aggravate uremia (Carney et al. Minocycline pharmacokinetics are not modified by hemodialysis, forced diuresis, or peritoneal dialysis (Carney et al. Addition of minocycline to peritoneal dialysis fluids is not recommended because they are well absorbed from the peritoneal cavity (Kunin, 1967). Newborn infants and children Minocycline should generally not be given to children under nine years of age because of the risk of permanent tooth discoloration. When the drug is administered to a child, the No changes in relation to minocycline pharmacokinetics were observed in patients with liver cirrhosis (Jonas and Cunha, 1982). Some animal studies suggest a possible mild neuroprotective effect by minocycline in hepatic encephalopathy. Bioavailability Minocycline is essentially completely absorbed from the stomach, the duodenum, and the jejunum after oral administration. The absorption does not seem to be significantly impaired by administration with food or milk (Smith et al. The serum half-life of minocycline is approximately 16 hours after single dose administration (Bernard et al. Newer formulations of minocycline appear to have bioequivalence to older products. In a crossover, randomized, single-blinded study in 12 fasting healthy adult male and female volunteers, the bioequivalence of two capsule formulations containing 100 mg minocycline was assessed, with no differences found between the new formulation and the reference compound (Setiawati et al. Drug distribution the drug is highly lipophilic and has an excellent distribution in tissues (Saivin and Houin, 1988). The drug may be detected in serum for up to 48 hours after this single oral dose (Steigbigel et al. After this dose, a serum level of about 1 g/ml is still detectable after 24 hours (Cartwright et al. If after an initial oral dose of 200 mg a dose of 100 mg every 12 hours is continued, serum levels are maintained in the range of 2. When an oral dose of 100 mg minocycline was given twice daily, peak serum levels were reached after 5 days, and these were significantly higher in women (mean 3. A significant inverse correlation has been demonstrated between body surface area and serum concentrations (Bernard et al. When a 100 mg dose of minocycline dissolved in 200 ml of 5% dextrose in water is infused over 30 minutes, a mean peak serum level of 8.


