Cheap tricor 160 mg otc
Sedation for oocyte retrieval using target controlled infusion of propofol and incremental alfentanil delivered by nonanesthetists cholesterol levels chart mayo clinic cheap tricor american express. Propofol versus thiopental sodium as anaesthetic agents for oocyte retrieval: A randomized controlled trial. Propofol concentration in follicular fluid during general anesthesia for transvaginal oocyte retrieval. The effect of propofol on parthenogenetic activation, in vitro fertilization and early development of mouse oocytes. The effect of propofol anaesthesia on oocyte fertilization and early embryo quality. Assay for midazolam in liquor folliculi during in vitro fertilization under anesthesia. The pain-relieving effect of electro-acupuncture and conventional medical analgesic methods during oocyte retrieval: A systemic review of randomized controlled trials. Effect of general anesthesia on fertilization and cleavage of human oocytes in vitro. General anesthesia versus monitored anesthesia care with remifentanil for assisted reproductive technologies: Effect on pregnancy rate. Propofol anaesthesia for ultrasound-guided oocyte retrieval: Accumulation of the anaesthetic agent in follicular fluid. Does spinal analgesia have advantage over general anesthesia for achieving success in in-vitro fertilization Epidural block: A preferred method of anesthesia for ultrasonically guided oocyte retrieval. Pregnancy outcome using general anesthesia versus spinal anesthesia for in vitro fertilization. Modifying effects of epidural analgesia or general anesthesia on the stress hormone response to laparoscopy for in vitro fertilization. Acupuncture-From empiricism to science: Functional background to acupuncture effects in health and disease. Acupuncture: Neuropeptide release produced by electrical stimulation of different frequencies. Effects of acupuncture on rates of pregnancy and live birth among women undergoing in vitro fertilisation: Systemic review and meta-analysis. Acupuncture and herbal medicine in in vitro fertilisation: A review of the evidence for clinical practice. In the beginning, the numbers of children were small, but then national and international registers were established. Parental factors are the most likely ones (1), but multiple pregnancies and their consequences have appeared to be the most common. A significantly increased risk of premature delivery was found between twins and singletons. In addition to premature births, congenital anomalies are also more common in twin pregnancies (9). Congenital heart disease is more common among twins than among singletons (11,12). In the large Danish register study (8), the total malformation rate (minor and major, 73. Patent ductus arteriosus, which is typical of premature birth, was very common among twins. An increased risk of anencephaly among twin infants born after assisted reproduction was also found (13). Risk of premature birth is further enhanced in other conditions predisposing to prematurity, such as uterine malformations. Twin pregnancies should not be induced among individuals who have any known increased risk factor of premature deliveries. Impaired glucose tolerance and pregnancy-induced diabetes (20) are more common during multiple pregnancies. Obesity further increases the risks of gestational diabetes and hypertension (22). Increasing the risk of diabetic complications by inducing a twin pregnancy due to transferring more than one embryo is not acceptable. These women often have cardiac anomalies and hypertension, and it is not justified to make these pregnancies more risky by transferring more than one embryo at a time. The likelihood of operative delivery with possible complications is higher in multiple pregnancies (8), which is another maternal indication not to transfer more than one embryo at a time (30). This urged clinicians to try to improve the treatment results by transfer of multiple embryos. A pregnancy resulting in at least one live birth was encountered in 142 of the 331 women (42. Pregnancy outcome was not affected when blastocysts were transferred, as shown in an analysis of couples undergoing single-blastocyst transfer (n = 52, live birth rate 53. In real life, it has not only been equally effective as double-embryo transfer, but has also been economically substantially cheaper than double-embryo transfer with all its complications (39,40). Effective cryopreservation methods have probably greatly reduced the need for strict selection (42,43). All of the obtained embryos can be transferred anyway, but a longer time may be required for achieving a pregnancy. At the same time, the proportions of children weighing less than 2500 g or born prematurely have significantly decreased, hence bringing about better health for the infants (45). The criteria presented in all the above-mentioned articles include the age of the female partner, the number of earlier unsuccessful cycles, and embryo quality. Regarding cleavage-stage embryos, the criteria are: less than 20% fragmentation; the embryo fills an even zona; no multinuclear blastomeres; four cells on day 2; and eight cells on day 3. A computer-assisted scoring system proved to be better than the conventionally used one (47). Using gene expression or biochemical information from cumulus cells may become more widely used (48,49). Sequential fresh and frozen embryo transfers increase the rate of pregnancy per transfer (43). Methods such as time-lapse follow-up in embryo selection (51) and measurement of serum concentration of human chorionic gonadotropin- (52) are helpful in selecting the best embryo for transfer. The earlier results have been confirmed by many recent surveys in Europe, Japan, and the U. However, the cumulative pregnancy rate among women over 40 years of age is actually similar if she cumulatively receives all of her embryos either one or two at a time. In addition, if the embryo is intact after thawing, a single frozen embryo should be transferred. These risks are largely caused by the high incidence of premature birth, but also congenital anomalies are increased among twins. Are major defects in children conceived in vitro due to innate problems in patients or to induced genetic damage Impact of single embryo transfer policy on perinatal outcomes in fresh and frozen cycles- Analysis of the Japanese Assisted Reproduction Technology registry between 2007 and 2012. Elective single-embryo transfer improves cumulative pregnancy outcome in young patients but not in women of advanced reproductive age.
Order discount tricor online
Failure of oocyte retrieval during in vitro fertilization: A sporadic event rather than a syndrome cholesterol ratio or total purchase cheap tricor online. Empty follicle syndrome due to human errors: Its occurrence in an in-vitro fertilization programme. Dual trigger with gonadotropin-releasing hormone agonist and standard dose human chorionic gonadotropin to improve oocyte maturity rates. Human chorionic gonadotropin-induced ovarian hyperstimulation syndrome is associated with up-regulation of vascular endothelial growth factor. Expression of vascular endothelial growth factor and its receptors in the human corpus luteum during the menstrual cycle and in early pregnancy. Luteolysis induced by a gonadotropin-releasing hormone agonist is the key to prevention of ovarian hyperstimulation syndrome. Lower levels of inhibin A and pro-alphaC during the luteal phase after triggering oocyte maturation with a 83. Impact of final oocyte maturation using gonadotropinreleasing hormone agonist triggering and different luteal support protocols on endometrial gene expression. Gonadotropin-releasing hormone agonist combined with a reduced dose of human chorionic gonadotropin for final oocyte maturation in fresh autologous cycles of in vitro fertilization. Vaginal micronized progesterone versus intramuscular progesterone for luteal support in women undergoing in vitro fertilization-embryo transfer. Ovarian hyperstimulation syndrome prevention by gonadotropinreleasing hormone agonist triggering of final oocyte maturation in a gonadotropin-releasing hormone antagonist protocol in combination with a "freezeall" strategy: A prospective multicentric study. Triggering ovulation with gonadotropinreleasing hormone agonist in in vitro fertilization patients with polycystic ovaries does not cause ovarian hyperstimulation syndrome despite very high estradiol levels. Factors that predict the probability of a successful clinical outcome after induction of oocyte maturation with a gonadotropin-releasing hormone agonist. Early ovarian hyperstimulation syndrome is completely prevented by gonadotropin releasing-hormone agonist triggering in high-risk oocyte donor cycles: A prospective, lutealphase follow-up study. Maternal and neonatal outcomes after gonadotropin-releasing hormone agonist trigger for final oocyte maturation in patients undergoing in vitro fertilization. Low-dose human chorionic gonadotropin versus estradiol/ progesterone luteal phase support in gonadotropinreleasing hormone agonist-triggered assisted reproductive technique cycles: Understanding a new approach. Triggering of final oocyte maturation with gonadotropin-releasing hormone agonist or human chorionic gonadotropin. Additionally, genetic analyses of embryos sometimes require a delay that might preclude fresh transfer, necessitating cryopreservation. Centers for Disease Control and Prevention reported 73,571 fresh autologous embryo transfers, 46,779 autologous transfers of thawed embryos, 8597 fresh transfers of fresh embryos derived from oocyte donation, and 9499 transfers of thawed embryos derived from donor oocytes (1). About half of human fertilized oocytes do not develop to the blastocyst stage, and those that do form blastocysts are often genetically abnormal. The ploidy of each embryo is used to decide which embryos are eligible for transfer. Techniques for embryo biopsy and genetic testing have recently advanced, and it appears that the recent techniques increase the probability of selecting a viable embryo that will implant compared to selection based on embryo morphology alone. Genetic analysis of the biopsied tissue can require several hours and the biopsies are typically shipped overnight to a laboratory for analysis. Therefore, the transfer of biopsied embryos is typically delayed by one day or longer, depending on techniques and circumstances. The resulting delay may be suboptimal for various reasons, and many centers have elected to cryopreserve the embryos while genetic test results are obtained and used to form decisions. Enhanced follicular development results in supraphysiologic levels of estradiol and other hormones. Supraphysiologic estradiol and progesterone levels also follow the ovulatory trigger. Under this hypothesis, viable but slowly developing transferred embryos fail to implant because the endometrial receptive phase might expire before the embryo is able to initiate viable trophoblast invasion. A randomized trial found greater implantation and clinical pregnancy rates per transfer in normal-responder patients who had entire cohorts of bi-pronuclear oocytes cryopreserved for subsequent thaw and transfer of two resulting blastocysts compared to patients who had two fresh blastocysts transferred (9). That study focused only on endometrial receptivity and therefore only on cycles receiving an embryo transfer. A subsequent meta-analysis of three randomized trials compared ongoing pregnancy rate per randomized subject through the first transfer attempt, and reported a risk ratio of 1. However, since that report was published, one of those three randomized trials was withdrawn. One of those studies (11) featured a sub-analysis that found that the difference could be explained by day-6 blastocysts having much greater implantation rates in thaw transfers than in fresh transfers, while the day-5 blastocysts were roughly comparable between thaw and fresh transfers. However, premature progesterone elevation is not associated with a detrimental effect in oocyte donation cycles (14), suggesting that the detrimental effect is through impaired endometrial receptivity, and not a detrimental effect on the embryo cohort. Embryo cryopreservation circumvents the effect of premature progesterone elevation in autologous patients (16), and premature progesterone elevation in the stimulated cycle is even predictive of success in subsequent thaw cycles (17). The impaired endometrial receptivity in fresh autologous transfers following premature progesterone elevation is largely mitigated in cycles with excellent embryo cohorts (18), apparently due to rapidly developing embryos compensating for advanced endometrial development (8). Unfortunately, reduced live birth rates have been reported with fresh autologous embryo transfer following agonist trigger (23). This might be largely addressed in very high responders by applying intensive luteal support (24,25). Alternatively, supraphysiologic progesterone levels depress ciliary beat frequency by approximately half compared to controls (33), potentially elevating the risk of implantation in an inappropriate location. This is unnecessary with the option of agonist trigger and cohort cryopreservation. Compromised endometrial receptivity, indicated by early rising progesterone levels (76,77), for example, should not motivate premature trigger if the embryos will all be frozen for later use. Moderately extended stimulation of autologous patients might result in supernumerary embryos for additional transfers without the need for additional retrievals, while in oocyte donors might result in sufficient oocytes to support additional recipients. Cryopreservation of oocytes or embryos allows autologous pregnancy potential to be preserved indefinitely, even while ovarian reserve declines naturally or through medical interventions. This includes cancer treatment regimens with chemotherapy, surgery, or radiation therapy that can impact the ovary and for conditions such as endometriosis or other benign pathology. The recent increased usage is related to the confluence of three methodological improvements. The first of these improvements was trophectoderm biopsy of the outer cells of a blastocyst, a technique reported to cause less embryonic damage than cleavage-stage biopsy (81). The second improvement was the ability to routinely test for the presence of all 46 chromosomes (3,82), rather than previous analyses of about 10 select chromosomes by fluorescence in situ hybridization. The last of these improvements was blastocyst vitrification (83), which allowed good success rates in transfers that were delayed while genetic analyses were completed. A retrospective study compared patients who, following a failed fresh blastocyst transfer, opted for either another fresh transfer or else a segmented cycle (84). Furthermore, there have been reported reductions in certain perinatal risks with transfer of frozen embryos when compared to fresh autologous transfer, as discussed previously (48). However, the relative risk of large for gestational age has been reported to be 1. The improved implantation rates conferred with cryopreservation (9) and genetic screening (68) support routine elective single-embryo transfer. Multiple birth is associated with numerous increased obstetric and pediatric risks, including greater incidence of preterm delivery, pre-eclampsia, gestational diabetes, and pediatric complications of prematurity (69,71). Iatrogenic multiple births increase costs per delivery and for society as a whole, with annual costs estimated to exceed $6 billion in the U.
Buy 160mg tricor
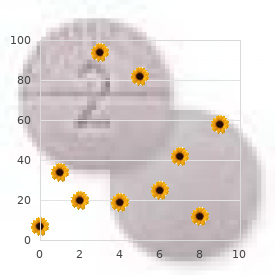
Later evidence indicated that the chamber contained inflammatory proteins cholesterol medication debate discount tricor 160 mg free shipping, perhaps explaining the failure. A small number of human embryos had been flushed from human oviducts or uteri after sexual intercourse, providing slender information on these earliest stages of human embryology. It was time to attain human fertilization in vitro, in order to move close to working with infertile patients. Ethical issues and moral decisions would emerge, one after the other, in full public view. Matters such as cloning and sexing embryos, the risk of abnormalities in the children, the clinical use of embryo stem cells, the ethics of oocyte donation and surrogate pregnancy, and the right to initiate human embryonic life in vitro would never be very far away. These issues were all acceptable, since I was confident that studies of human conception were essential for future medicine, and correct ethically, medically, and scientifically. The increasing knowledge of genetics and embryology could assist many patients if I could achieve the beginnings of human in vitro fertilization xvii human fertilization and grow embryos for replacement into their mothers. Despite this scarcity, one or two of those matured and fertilized in vitro possessed two nuclei after insemination. I devised a cow model for human fertilization, using in vitro-matured oocytes and insemination in vitro with selected samples of highly active, washed bull spermatozoa extracted from neat semen. It was a pleasure to see some fertilized bovine eggs, with sperm tails and characteristic pronuclei, especially using spermatozoa from one particular bull. A colleague had stressed that formalin fixatives were needed to detect sperm tails in eggs. Barry Bavister joined our team to study for his PhD and designed a medium of high pH, which gave excellent fertilization rates in hamsters. Finally, while browsing in the library of the Physiological Laboratory, I read a paper in the Lancet that instantly caught my attention. Steptoe of the Oldham and District General Hospital (18), it described laparoscopy, with its narrow telescope and instruments and its minute abdominal incisions. He could visualize the ampulla and place small amounts of medium there, in an operation lasting 30 minutes or less and maybe even without using anesthesia. This is exactly what I wanted, because access to the ampulla was equivalent to gaining access to ovarian follicles. Despite advice to the contrary from several medical colleagues, I telephoned him about collaboration and stressed the uncertainty in achieving fertilization in vitro. He responded most positively, just as Molly, Howard and Georgeanna, and Victor had done. Its dozen or more oocytes were matured in vitro for 37 hours, then Barry and I added washed spermatozoa suspended in his medium. To our delight, spermatozoa were pushing through the zona pellucida, into several of the eggs. One fertilized egg had fragments, as Chang had forecast from his work on oocyte maturation and fertilization in vitro of rabbit eggs. This evidence strengthened the need to abandon oocyte maturation in vitro and replace it with stimulating maturation by means of exogenous hormones. Our 1969 paper in Nature surprised a world unaccustomed to the idea of human fertilization in vitro (19). Richard Gardner, another PhD candidate, and I excised small pieces of trophectoderm from rabbit blastocysts and sexed them by staining the sex chromatin body. Those classified as female were transferred into adult females and were all correctly sexed at term. This work transferred my theoretical ideas of a few years earlier into the practice of preimplantation diagnosis of inherited disease, in this case for sex-linked diseases (20). So the first ethical papers were written by scientists and lawyers and not by philosophers, ethicists, or politicians. He had worked closely with two pioneers, Palmer in Paris (23) and Fragenheim in Germany (24). He improved the pneumoperitoneum to gain working space in the abdominal cavity and used carbon fibers to pass cold light into the abdomen from an external source (25). Those beautiful oocytes were surrounded by masses of viscous cumulus cells and were maturing exactly as predicted. It was a pleasure and a new duty to meet the patients searching for help to alleviate their infertility. Notice that the pronuclei are apparently aligned with the polar bodies, although more dimensions must be scored to ensure that polarity has been established in all axes. Ovarian stimulation, even though mild, produced five or six mature follicles per patient, and ripe oocytes came in a steady stream into my culture medium for insemination and overnight incubation. The next morning, the formation of two pronuclei and sperm tails indicated fertilization had occurred, even in simple media, now with a near-neutral pH. I had become highly familiar with the teratologic principles of embryonic development, and knew many teratologists. The only worry I had was the chance of chromosomal monosomy or trisomy, on the basis of our mouse studies, but these conditions could be detected later in gestation by amniocentesis. This beautifully expanded blastocyst had a large embryonic disc that was shouting that it was a potential source of embryonic stem cells. When human blastocysts became available, we tried to sex them using the sex chromatin body as in rabbits. Unfortunately, they failed to express either sex chromatin or the male Y body so we were unable to sex them as female or male embryos. Criticism was mostly aimed at me, as usual when scientists bring new challenges to society. Criticism came not only from the Pope and archbishops, but also from scientists who should have known better, including James Watson (who testified to a U. Senate Committee that many abnormal babies would the beginnings of human in vitro fertilization xix 18. The follicles had been classified as ovulating or non-ovulating by laparoscopic examination in vivo. Data were analyzed by cluster analysis, which groups follicles with similar features. Note that two sharply separated groups of follicles were identified, each with very low levels of withingroup variance. Attempting to combine the two groups resulted in a massive increase of within-group variation, indicating that two sharply different groups had been identified. These different groups accorded exactly with the two groups identified by means of steroid assays. With this form of stimulation, follicle growth displays considerable variation within groups. Attempts to combine all the groups result in a moderately large increase in variation. These scientist critics knew virtually nothing about my field, so who advised them to make such ridiculous charges Cloning football teams or intelligentsia was always raised by ethicists, which clearly dominated their thoughts rather than the intense hopes of our infertile patients. Growing embryos became a routine, so we decided to transfer one each to several patients. Transferring embryos via the cervical canal, the obvious route to the uterus, was virtually a new and untested method. From now on, we worked with patients who had seriously distorted tubes or none whatsoever. This step was essential, since no one would have believed we had established a testtube baby in a woman with near-normal tubes. Yet we already knew that embryos could be obtained for men with oligozoospermia or antibodies to their gametes, and for women in various stages of endometriosis. This condition was not a result of the aspiration of granulosa and cumulus cells, and luteal support would be needed, preferably progesterone. Injections of progesterone in oil given over that long period of time seemed unacceptable since it would be extremely uncomfortable for patients. While mulling over this problem, my attention turned to those earlier endocrinologists who believed that exogenous hormones would distort the reproductive cycle, although I doubt they even knew anything about a deficient luteal phase.
Buy tricor with american express
In the surviving patients best cholesterol lowering foods recipes cheap 160mg tricor, all posterior column graft sites healed, but four of the five proximal sacral sites showed a stable pseudarthrosis. All four patients who did not have complete bony healing progressed to have a complication that required surgical intervention. A careful balance must be maintained between providing primary stability using implants, while minimizing implant material to reduce infection risk. While the functional outcomes, hardware failures, and complication rates are comparable to existing techniques, there has been a decreased rate of deep infection that necessitated a revision surgery (14 vs. This principle of minimizing instrumentation to reduce infection risk may be useful in selecting what reconstruction method to utilize. Aside from painful nonunions, complications directly related to pseudarthroses have not been reported in articles describing spinopelvic reconstruction for tumor. However, there remains a high incidence of lumbosacral pseudarthroses in the spinal deformity literature and these have been associated with loss of fixation, fracture, and failure of instrumentation. These authors found that the type of surgery performed was the greatest risk factor for infection. In this series, all infections healed with surgical debridement and culture-directed antibiotics. Sacrifice of the S3, however, appears to be the key level that has the highest association with both bowel and bladder incontinence. Resection of the S1 nerve roots has been shown to decrease the chances of postoperative ambulation to 50 versus 76% or up to 100% when the highest level sacrificed is S2 or S3, respectively. At the time of revision, surgery should address the original cause of hardware failure. The concentration of Resection and reconstruction of sacropelvic tumors should aim to provide the patient a disease-free state with the hope of a functional outcome. Minimizing the risk of local recurrence is therefore a key aspect in selecting the proper surgical management. En bloc resection, in which the tumor is not violated during the procedure, has proven to be a technique that can decrease the risk of recurrence. The larger studies that 315 Thoracolumbar the high rate of complications with any technique. Early methods of spinopelvic reconstruction utilized extensive bone grafting to obtain an adequate fusion. The forces transmitted across the construct compress the proximal and distal docking sites of the fibular grafts, providing a loading condition that is more favorable for bony healing. The reported complications included one pseudarthrosis and hardware failure, one wound infection, two local recurrences, and two distant metastases. The closed-loop technique was developed in an effort to avoid the points of stress identified in the earlier techniques. This construct allows the axial load to be transmitted to the pelvis at two separate fixation points, through the transiliac bar, as well as the rod connecting the iliac screws. An additional benefit of this technique is the minimal amount of instrumentation needed to provide the additional stability. Maximum stress is observed at a point on the spinal rod between the pedicle screw of the fifth lumbar vertebra and the iliac screw (I). In recent years, multiple institutions from around the globe developed a database of nearly 1,500 patients with primary tumors of the spine. There is conflicting data on the extent that adjuvant chemotherapy and radiotherapy contribute to the rate of complications. Though many techniques have been described, there remains no consensus on the best reconstruction method because all have had high complication rates. Newer reconstruction techniques developed have been targeted toward decreasing the failures of the constructs and minimizing instrumentation. The analysis of the treatment of giant cell tumor of the pelvis and sacrum [in Chinese]. Pelvic reconstruction with compound osteosynthesis following hemipelvectomy: a clinical study. Partial pelvic resection (internal hemipelvectomy) and endoprosthetic replacement in periacetabular tumors [in German]. Modular hemipelvic endoprosthesis reconstruction-experience in 100 patients with mid-term follow-up results. Reconstructive strategies for partial sacrectomy defects based on surgical outcomes. Reconstruction after total sacrectomy: early experience with a new surgical technique. Bowel and bladder continence, wound healing, and functional outcomes in patients who underwent sacrectomy. Surgical management of primary bone tumors of the spine: validation of an approach to enhance cure and reduce local recurrence. Use of pedicle screw fixation in the management of malignant spinal disease: experience in 100 consecutive procedures. Surgical resection and reconstruction after resection of tumors involving the sacropelvic region. There are two main categories of such inflammatory arthritides-seropositive and seronegative spondyloarthropathies. Because of advances in treatment, the burden of this disease has decreased, thus reducing the need for surgical intervention. In the cases that fail medical management, surgery plays a critical role in maintaining neurological function and spinal stability. Perhaps the most difficult complication is that of instrumentation failure because of poor bone quality and diminished healing potential. Instability and subsidence of the atlantoaxial joints can lead to occipital headaches that result from impingement of upper cervical nerve roots. Patients with atlantoaxial subluxation may report the sensation of the head falling forward during flexion. Yonezawa et al defined subaxial subluxation as more than 4 mm or 20% olisthesis of the vertebral body diameter. In addition, this process creates syndesmophytes, or ossification of the ligaments around the vertebrae, leading to the formation of a "bamboo spine. Although both approaches allow decompression, fusion, and stabilization, the posterior approach is generally more extensile compared to the anterior and allows for extension of the surgical incision from the occiput all the way to the pelvis. Specifically, lateral mass screws are commonly used in the subaxial cervical spine. Pain is usually worse in the morning and at night, and spinal motion and chest expansion are limited. As the disease progresses, there is a gradual loss of lordosis in the lumbar and cervical spine, which can lead to progressive sagittal plane deformity given the patient is no longer able to stand upright. Cages or allograft bones are generally used to replace the resected disc or vertebral body and to reconstruct the anterior column. Additionally, anterior plates may be used to stabilize the fusion site and prevent cage or graft displacement. Typically, however, the location of neurologic impingement requiring decompression will usually dictate the surgical approach. Supplemental posterior instrumentation should be considered when multilevel anterior procedures are done to avoid the risk of pseudarthrosis. Stabilization may be performed with long posterior constructs, unless the source of neurological compression is anterior. For rigid chin-on-chest deformity stemming from cervicothoracic kyphosis, single-stage opening or closing wedge osteotomies have been described. Because these procedures lacked rigid fixation, however, patients were often placed in halo-vest immobilization postoperatively which was associated with significant morbidity. Today, posterior wiring is commonly used as adjunct with other types of internal fixation.

Purchase tricor in india
Perioperative problems included an increased risk of neural injury and morbidity from prolonged operative exposure cholesterol jumped 50 points purchase 160 mg tricor amex. In this article, we outline the evolution of sublaminar wiring with a stress on the reported complications. They reported on 100 patients who underwent treatment for scoliosis with this technique and described no instances of neural injury, with a 14% rate of pseudoarthrosis at 2 years which they attributed to imperfect wirefixation technique. Direct dural contusion occurring during wire passage and manipulation is also reported. In their experience of more than 10 years with sublaminar, stainless steel wires, Lea Plaza et al24 described the development of layers of fibrous tissue that isolate metal from dura. This, they believe, acts like a protective shield, when occasionally the wires have to be removed and as a barrier to prevent spread of infection from bone or soft tissue to meninges. There have been interesting studies that reported the dimensions of the human spinal canal at various levels specifically looking at the safety of passing a sublaminar wire in the vicinity of the spinal cord and nerve roots. Such a "safety zone" is nonexistent in lambs and pigs unless an extensive laminectomy is performed to decrease the depth of wire penetration. Most new bones were formed outside the spinal canal and although the radius of the canal reduced, it was not sufficient to result in spinal stenosis during the period of the study. Dove30 reported the results from a questionnaire circulated among members of the British Scoliotic Society in order to establish the morbidity of surgery for spinal deformities in the years 1983 and 1984 in Great Britain. Support for the spondylitic spine by means of buried steel bars attached to the vertebrae. Segmental spinal instrumentation in the management of neuromuscular spinal deformity. Segmental spinal instrumentation in the management of fractures of the thoracic and lumbar spine. The advantages of titanium alloy over stainless steel plates for the internal fixation of fractures. Surgical correction of scoliosis with a new three-dimensional device, the "Lea Plaza Frame". Our discussion of efficacy will serve only to frame our discussion of complications following percutaneous vertebral cement augmentation. However, when they do occur they have the potential for devastating consequences to the patient. In five patients, the injury occurred from bony retropulsion at the procedural level ranging from 3 to 112 days after the initial procedure. Three patients developed injuries related to fracture retropulsion at adjacent levels to the index procedure, which were also addressed surgically. Leakage of cement into the intervertebral disc has been associated with an increased risk of adjacent level fracture. In the rare instances where postprocedural infection has been reported, it has been in immunocompromised hosts. Biomechanical studies have demonstrated that augmentation reduces compliance within that segment in both neutral and bending modes, thus leading to greater force transmission to the adjacent levels. Although these procedures are minimally invasive and often performed by specialists other an spinal 161 Thoracolumbar surgeons, the potentially devastating side effects that can occur require a treatment plan both for intensive medical management and open surgical intervention should the need arise. Percutaneous vertebroplasty in 1,253 levels: results and long-term effectiveness in a single centre. Pain relief following percutaneous vertebroplasty: results of a series of 283 consecutive patients treated in a single institution. Vertebral compression fractures: pain reduction and improvement in functional mobility after percutaneous polymethylmethacrylate vertebroplasty retrospective report of 245 cases. Percutaneous vertebroplasty: a developing standard of care for vertebral compression fractures. Percutaneous vertebroplasty compared with optimal pain medication treatment: short-term clinical outcome of patients with subacute or chronic painful osteoporotic vertebral compression fractures. Percutaneous vertebroplasty: functional improvement in patients with osteoporotic compression fractures. Clinical outcomes after acute osteoporotic vertebral fractures: a 2-year non-randomised trial comparing percutaneous vertebroplasty with conservative therapy. Effectiveness of vertebroplasty using individual patient data from two randomised placebo controlled trials: meta-analysis. Comparison of kyphoplasty with use of a calcium phosphate cement and non-operative therapy in patients with traumatic non-osteoporotic vertebral fractures. Kyphoplasty in osteoporotic vertebral compression fractures-guidelines and technical considerations. Therapeutic efficacy of injectable calcium phosphate cement in osteoporotic vertebral compression fractures: prospective nonrandomized controlled study at 6-month follow-up. Filling materials used in kyphoplasty and vertebroplasty for vertebral compression fracture: a literature review. The association of radiographically detected vertebral fractures with back pain and function: a prospective study. Vertebral augmentation in the treatment of vertebral compression fractures: review and new insights from recent studies. Randomized controlled trial of percutaneous vertebroplasty versus optimal medical management for the relief of pain and disability in acute osteoporotic vertebral compression fractures. Balloon kyphoplasty for the treatment of acute vertebral compression fractures: 2-year results from a randomized trial. Balloon kyphoplasty versus non-surgical fracture management for treatment of painful vertebral body compression fractures in patients with cancer: a multicentre, randomised controlled trial. Paraplegia as a complication of percutaneous vertebroplasty with polymethylmethacrylate: a case report. Percutaneous vertebroplasty for subacute and chronic painful osteoporotic vertebral compression fractures can safely be undertaken in the first year after the onset of symptoms. Neurological deficit due to cement extravasation following a vertebral augmentation procedure. Dose-dependent epidural leakage of polymethylmethacrylate after percutaneous vertebroplasty in patients with osteoporotic vertebral compression fractures. Cement embolization of a segmental artery after percutaneous vertebroplasty: a potentially catastrophic vascular complication. Risk factors predicting the new symptomatic vertebral compression fractures after percutaneous vertebroplasty or kyphoplasty. Aortic embolism of cement: a rare complication of lumbar percutaneous vertebroplasty. Anatomical and pathological considerations in percutaneous vertebroplasty and kyphoplasty: a reappraisal of the vertebral venous system. Vertebroplasty: cement leakage into the disc increases the risk of new fracture of adjacent vertebral body. Balloon kyphoplasty in the management of vertebral compression fractures: an updated systematic review and metaanalysis. Higher incidence of new vertebral fractures following percutaneous vertebroplasty and kyphoplasty-fact or fiction The adjacent bony endplates are exposed by removal of the vertebral disks and cartilaginous endplates. Patients with unstable burst fractures that have canal compromise greater than 50%, local kyphosis greater than 30 degrees, loss of vertebral body height of greater than 50%,4,5 or neurologic compromise are also considered candidates for surgical management. For this minimally invasive approach, a 4-cm incision is made lateral to the midline and a Kirschner wire is introduced lateral to the facet and held near the pedicle at the target thoracic level. A series of progressively larger diameter dilators are inserted and a retractor is placed over the largest one. The transverse process, facets, and lamina are exposed, and blunt dissection is carried down subperiosteally to expose the lateral portion of the vertebral body; the pedicle is removed and the dura is protected, if needed, with gentle medial retraction. The vertebral body resection is then performed and a compacted expandable cage is inserted through the portal and into the interbody space and subsequently extended. Because of adjacent anatomic structures, posterolateral approaches offer a smaller window through which to work anteriorly. This method of cage placement is particularly important in the lumbar spine because it avoids the need to sacrifice nerve roots in order to insert the device.
Cheap 160 mg tricor fast delivery
This is especially pertinent while working from a posterior approach because once the cage is deployed cholesteryl ester storage disease buy generic tricor line, it may very difficult to re-engage the cage with the extender if the placement needs revision. This type of cage/extender configuration can make it difficult to safely, or appropriately, steer the device into proper position. In a cadaveric analysis, Ebraheim et al24 found that the ideal placement of the posterior screw is 4 to 5 mm anterior to posterior wall with slight ventral angulation (10 degrees). Anterior screws should be placed perpendicular to the posterior wall or with a slight dorsal trajectory. The current incidence or subsidence is variable, with some studies reporting less than 10%25,26 and others as high as 80%. Lau and colleagues28 found that expandable cages have a higher rate and risk of subsidence compared to static cages. Vertebral body instrumentation following corpectomy requires preparation of the associated endplates. Nonexpandable cages should be slightly longer than the size of the relaxed corpectomy site given that retraction of the distracted ligaments will hold the graft in place. Implant failure may require revision surgery, in which case instrumented levels are increased to provide greater support and stability. Small cohort reports have shown that these approaches lead to reduced blood loss, smaller exposure and associated muscle dissection, decreased perioperative pain and morbidity, as well as earlier mobility. Advances in thoracic spine instrumentation and surgical approaches will lead to further reduction in associated morbidity/mortality and improve outcomes. There are a variety of stabilization and vertebral reconstruction systems available. Respiratory problems are the most common complication in up to 50% of patients and less frequently occurring complications include cardiac, vascular, gastrointestinal, and infection, which occur in 10 to 30% of patients. Use a double lumen endotracheal tube to help with selective lung deflation to limit lung injury during surgery. When applicable, the use of spiked vertebral plates (with rod systems) helps limit screw migration and resists axial loads. The anterior vertebral screw should be parallel to the posterior border of the vertebral body and the posterior screw should be slightly anterior. Vertebral body replacement systems should not be used as a stand-alone system as they should have additional stabilization by plate or rod instrumentation systems. Complication risk can be reduced with a thorough assessment of patient history and medical comorbidities, radiographic findings, surgeon proficiency with the surgical approach, and instrumentation system selection. Surgical planning for the treatment of thoracolumbar fractures: anterior, posterior, or combined approach An unusual complication of anterior spinal instrumentation: hemothorax contralateral to the side of the incision. They included biologic failure (related to infection, osteoporosis, and patient-specific issues), biomechanical failure, error in thought process, and error in application. For example, a translational deformity can result from an intrinsic bending moment between the rods, which can be avoided by cross-fixation of the dual rods and triangulation of the screws within the body. The posterior vertebral body screw should be placed 4 to 5 mm anterior to posterior vertebral wall with a slightly angulated trajectory (~10 degrees). They recommend screw placement in the anterior or middle portion of the vertebral body. From T3 to T12, the maximum posterior angle of the vertebral body relative to the frontal plane increases as you descend the spine. Thus, canal violation can be avoided by placing the posterior screw slightly anterior. Radiological outcomes of static vs expandable titanium cages after corpectomy: a retrospective cohort analysis of subsidence. The Mini-Open transpedicular thoracic discectomy: surgical technique and assessment. Minimal invasive anterolateral transthoracic transpleural approach: a novel technique for thoracic disc herniation. Video-assisted thoracoscopic surgery for thoracic disc disease: Classification and outcome study of 100 consecutive cases with a 2-year minimum follow-up period. Recommended diagnostic criteria for multiple sclerosis: guidelines from the International Panel on the diagnosis of multiple sclerosis. Segmental instrumentation for thoracic and thoracolumbar fractures: prospective analysis of construct survival and five-year follow-up. The relative lack of resistance to rotation and side bending with posterior element-based constructs has motivated the widespread use of pedicle screw fixation with rod constructs for segmental stabilization. Limited clinical data are available thus far regarding long-term safety and efficacy of these devices, and further studies will help refine the most appropriate indications for their use. These devices are commonly grouped because of their biomechanical similarities, though long-term complications with dynamic spacer use, such as device migration, are theoretically obviated by the achievement of segmental stability following successful fusion. Both devices function in a similar capacity to achieve indirect decompression via interspinous distraction, and as such, have similar limitations as to the precise pathoanatomy suitable for their use. While early research showed promise for treatment of neurogenic intermittent claudication, dynamic interspinous spacers have been shown to be associated with relatively high rates of spinous process fractures, especially in patients with osteoporosis and/or spondylolisthesis. Pedicle screw placement is technically demanding, but it has been demonstrated to be a safe and reproducible technique with appropriate training. Stabilization of segmental motion is essential to create a microenvironment suitable for osseous intervertebral fusion to occur. The spinous processes of the affected levels are identified through manual palpation and the use of intraoperative imaging. The interspinous ligament may either be removed or dilated without complete removal. Shepherd et al created a cadaveric model of spinous process loading in which hooks were placed through the spinous process and a tensile load to failure was applied. Three of these fractures were noted to heal spontaneously at 1 year, and three necessitated implant removal and laminectomy. The authors note that radiographically occult spinous process fractures may be only mildly symptomatic, but are likely responsible for a greaterthan-previously-considered proportion of suboptimal outcomes following interspinous spacer implantation. Such scenarios require a thorough dialog between physician and patient to ensure informed consent prior to proceeding with an extensive revision procedure. Advances in materials and minimally invasive surgical techniques have led to the development of a new generation of implantable devices for interspinous fusion. Association between degenerative spondylolisthesis and spinous process fracture after interspinous process spacer surgery. A comparative study of transpedicular screws, laminar hooks, and spinous process wires. Complications of pedicle screw fixation in scoliosis surgery: a systematic review. Transpedicular screws are still largely considered to be the "gold standard" technique for this purpose because they achieve fixation across all three columns and therefore represent a powerful tool for maintaining segmental stability which is well suited for applications such as deformity correction, trauma, and tumor/infection. Osteoporosis currently affects over 40 million individuals in the United States alone and is expected to become even more prevalent in the future as the elderly population continues to grow. This report also included an in-depth discussion of the various benefits as well as the potential pitfalls associated with this method of segmental instrumentation. The pullout strength of the cortical implants was found to be significantly higher, which the authors suggested could be related to their medial starting point and their unique thread design which allow them to acquire greater bony purchase. A traditional pedicle screw trajectory (a) exploits a cancellous channel and terminates in cancellous bone. While this technique may be relatively safer than transpedicular fixation because the implants are directed away from the thecal sac and nerve roots, the drill, tap, or screws may still extend beyond the margins of the vertebra so that they are in continuity with the central canal, foramina, disc space, or psoas muscle.
Cheap 160mg tricor free shipping
They cheerfully tolerated my ignorance cholesterol lowering foods olive oil buy 160 mg tricor amex, and patiently answered all my questions, however irrelevant or naive. Besides Joelle, Genevieve (and later Nadine), Soraya, the technicians, and the trainees, the meetings are regularly attended by Myriam, a leading clinical geneticist with multispecialty training in genetics, pediatrics, and fetopathology and an impressive publication record in molecular genetics. She was recently named to a prestigious genetics professorship at the time of my visit, and is especially active in promoting close links between the fetopathology and genetics departments. Myriam is also one of the main genetic counselors at Ah, and specializes in complex and difficult cases. She is a young pediatrician with parallel training in fetopathology who was working on her thesis in clinical genetics. Chief on the agenda of each weekly staff meeting is a review of all the fetal autopsies held during the past week, with a focus on unusual or difficult cases. The most difficult among them are often recalled by the fetopathologists, sometimes years later. Fetopathology staff is one among several regular departmental meetings at Ah dedicated to fetal and newborn anomalies. The others are molecular genetics, gynecology and maternity, pediatrics, and a weekly meeting of geneticists and students centered on the investigation of complex genetic 88 / Chapter Three conditions. Myriam and Isabelle often participate in all these meetings, with Soraya joining occasionally. In addition, Soraya and Joelle are frequently invited to present cases at the molecular genetics staff meetings and periodically at the maternity and pediatrics staffs. They prepare these presentations very carefully, partly because fetopathology may be seen as a lower-status specialty, and partly because they are keen to receive feedback from other experts. Leila, a fetopathologist specializing in the study of fetal brain tissue and usually responsible for retrieving data from cases discussed at the fetopathology staff meetings, might have added, "when the computer system is working as it should," which was far from being always the case. Sometimes, the first five or ten minutes of the fetopathology staff meetings are dedicated to fiddling with the computer to retrieve the appropriate data and project them on a screen. The simultaneous use of both methods of recording and organizing data may correspond to the "bicultural" aspect of fetal pathology: at the same time a traditional specialty rooted in nineteenth-century autopsy protocols and one that participates in the development of cutting-edge scientific knowledge. The morgue is usually empty, and the collection of a fetal body is a relatively rare event. In compliance with the French law of 2008 concerning the disposal of fetal bodies, the decision of what to do with such a body belongs exclusively to the couple. Joelle told me that when she started work as a fetopathologist twenty years ago, 90% of the parents agreed to a fetal autopsy. She was convinced that the percentage of permissions received for an autopsy was lower now; recent data indeed support this view. She and Soraya attributed the decrease to a sharp decline in the overall number of autopsies being performed in French hospitals; the growing importance of religion, especially Islam, among people originally from North and sub-Saharan Africa; and the influence of midwives, who increasingly encourage the couple to see the expelled fetus as "their baby. The growing assimilation of fetuses with children may extend such reluctance to nonviable fetuses. Joelle and Soraya receive a steady stream of mostly female young physicians who undergo fetopathology training, and dedicate an important portion of their time to such training. Soraya, who at the time of my study was nearing the French obligatory retirement age for public servants (a category that includes physicians in public hospitals), is especially concerned about transmitting her very impressive knowledge of anomalies of the fetal neural system. Myriam is a very gifted teacher, able to present complex problems in a clear and well-organized manner. She often illustrates her explanations with diagrams and photographs containing images either already present in her computer or rapidly found on the web. Their solicitude reflects a worry that young people will abandon a specialty that is difficult to master and has a relatively low standing. Students of fetopathology have to familiarize themselves with a very traditional medical specialty, pathology, and a very new one, clinical and molecular genetics. They need to acquire a "feel" for tissues that they cut and manipulate, and a good visual memory of normal fetal structures and pathological changes in these structures. They have to develop the manual dexterity needed to manipulate tiny fetal bodies, as when learning how to pass a thin probe through fetal heart chambers to check for the presence of blocked passages. Trainees also need to learn how to cope with "difficult" fetal bodies, especially those macerated and decomposed in the womb. Maceration may be the result of late discovery of spontaneous fetal death, or of a long interval between the initiation of induced abortion and the expulsion of the fetus. Macerated fetuses have an unpleasant aspect; they are also more difficult to study, because the pathologist has to distinguish between malformations which existed before fetal demise, and changes which took place after the death, such as the rapid deterioration of brain tissue. To persuade their students to persist in their choice of specialization despite all the obstacles, Joelle and Soraya attempt to convey their enthusiasm about fetopathology. They make special efforts to include students at every interesting professional event in the hospital, Diagnostic Puzzles / 91 take time to explain each unusual case, and strive to find them feasible and stimulating subjects for their dissertation. Joelle explained that she started to make such photographs as an informal service for the parents. At first she employed her own very simple camera, but later a bereaved family offered her a better one. Joelle sometimes mentioned parents who wished to dress the fetus/child in fancy or unusual clothes. I saw only one such case: a photograph of a thirdtrimester fetus dressed in a blue and yellow Superman tee shirt. Sometimes the parents also want to have the hospital identification bracelet placed on the body in the maternity ward. Myriam recalled a case in which the father of a deceased fetus/child who had come for a follow-up visit asked for such a bracelet (the mother, described as highly distressed by the pregnancy loss, had returned to her country of origin). A frequent cause of the latter is preeclampsia-pregnancy-related high blood pressure with a high level of protein in the urine. The fetus often suffers, too, but fetal problems are seen as secondary to maternal ones. Other maternal diseases, such as diabetes, may produce severe fetal malformations. Joelle remarked to me several times that discussions about causes of fetal malformations tend to focus on abnormal genes and neglect the frequent nongenetic causes of inborn malformations, such as diabetes or placental anomalies. Death in the womb can also be produced by too much or too little amniotic fluid, the leaking of amniotic fluid, and in more dramatic cases the premature rupture of the amniotic sac. Leaking of amniotic fluid increases the danger of abnormal fetal development and of infection. The opposite is also true: an infection can be at the origin of an insufficient production of amniotic fluid, while a combination of infection and a paucity of amniotic fluid can produce fetal malformations. When fetal medicine experts at Ah observe a combination of an infection and fetal anomalies, they usually inform the pregnant woman about a "reserved prognosis of the future child"-that is, a high probability that the child will die either in the womb or immediately after birth. Twin pregnancy is riskier than a single one; hence the relatively high proportion of twins among dissected fetuses. In some cases, the demise of one twin is followed by the death of the other, even when the twins did not share placentas and amniotic sacs. In such cases, autopsy frequently reveals that both twins had multiple malformations. This option has become more viable with the improved survival rate of very premature babies. If the condition develops at a stage at which it is too early to safely induce a delivery, the physicians may attempt fetal surgery in the womb. The most accepted method today is blocking the blood vessels that connect the twins via fetoscopic laser coagulation. The impossibility for a woman to terminate a pregnancy after twenty-two to twenty-four weeks led to "desperate" surgeries with a high fetal mortality rate. Death in the womb, especially late in pregnancy, is frequently an unanticipated event. Most French women undergo routine screening for Down syndrome at ten to twelve weeks of pregnancy, which includes ultrasound, and a second detailed ultrasound at twenty to twenty-two weeks. If their physicians suspect that the fetus has a rare or complicated condition, they are referred to a tertiary center such as Ah, where they are seen by several experts in fetal medicine and clinical genetics. They are integrated into dense networks of interdisciplinary collaborations and rely on the contributions of many colleagues and collective debates about contentious cases.


