Purchase finast 5mg
Technical principles of direct innominate artery revascularization: a comparison of endarterectomy and bypass grafts hair loss male legs cheap 5 mg finast free shipping. Diagnosis and long-term clinical outcome in patients diagnosed with hand ischemia. Magnetic resonance imaging depicts mural inflammation of the temporal artery in giant cell arteritis. Thrombosis of the palmar arterial arch and its tributaries: etiology and newer concepts in treatment. This chapter will review the anatomy of the upper extremity veins and thoracic outlet in addition to the prevalence, causes, clinical characteristics, complications, and diagnostic imaging of upper extremity deep venous thrombosis and thoracic outlet syndrome. The left brachiocephalic vein is approximately 6 cm in length, has a more horizontal course, and joins the right brachiocephalic vein to form the superior vena cava. The axillary vein begins at the inferior border of the teres major muscle and continues through the axilla to the lateral border of the first rib, where it becomes the subclavian vein. The subclavian vein continues medially, deep to the clavicle, until it joins the internal jugular vein, forming the brachiocephalic vein. Knowing these relationships will aid in identification of these vessels and help in distinguishing possible large collaterals from the native vessels. The superficial basilic and cephalic veins are also usually included in the examination. In the neck, the internal jugular vein courses from the jugular foramen at the base of the skull lateral to the carotid arteries within the carotid sheath. Earlier studies documented thrombosis in 2% to 12% of patients with central venous catheters. Catheter material and diameter have also been found to affect the incidence of thrombus. The lowest rates have been for polyurethane and silicone catheters and for those with an external diameter less than 2. Less common signs and symptoms include skin discoloration, a sense of coldness in the hand and forearm, tenderness over the affected vein, paresthesia, and numbness. These signs and symptoms, however, are nonspecific and confirmation of the diagnosis by objective testing is necessary. However, it is an invasive procedure that must be performed in the radiology department. It is uncomfortable for the patient and venous catheterization may be technically difficult secondary to arm swelling. Moreover, intravenous iodinated contrast administration carries the risk of nephrotoxicity and allergic reaction, in addition to predisposing to the development of thrombus. Venography may also fail to demonstrate the status of the internal jugular or brachiocephalic veins when more peripheral occlusive thrombus is present. It is a potentially portable examination and can be performed at the bedside for critically ill patients. Unlike venography, the internal jugular and peripheral brachiocephalic veins can be evaluated, despite the presence of thrombus in the more peripheral vessels. Limitations of duplex sonography include inability to visualize the superior vena cava and more central portions of the brachiocephalic veins. In addition, small nonocclusive thrombus may be missed in the subclavian vein secondary to the inability to compress this vessel because of the overlying clavicle. False-negative results can occur secondary to limitations in the ability to compress vessels (see earlier). Variations exist in the recommended techniques and protocols for an ultrasound examination of the upper extremity venous system. At our institution, the internal jugular, subclavian, axillary, and brachial veins are imaged, in addition to the superficial basilic and cephalic veins to the level of the antecubital fossa. Compression is always performed in the transverse plane because compression in the longitudinal plane may result in sliding off the vessel, potentially causing a falsenegative result. The subclavian vein is followed in its entirety and can be imaged from a supraclavicular approach medially and an infraclavicular approach laterally. It should be remembered that the subclavian vein lies anterior and caudal to the subclavian artery. The basilic vein is single, taking a more superficial and medial course in the upper arm. The basilic and cephalic veins run in the subcutaneous tissue, above the muscles of the arm, and do not course adjacent to an artery. The medial subclavian vein and other centrally situated veins, including the brachiocephalic veins, can be difficult if not impossible to visualize. Use of a square phased-array transducer and a suprasternal-supraclavicular approach may aid in imaging these regions. Spectral Doppler waveforms are obtained initially in the contralateral internal jugular and medial subclavian veins. These waveforms serve as an internal reference to evaluate for asymmetry, which may be indicative of more centrally located thrombosis not directly visualized by ultrasound examination. Waveforms are then obtained in the ipsilateral internal jugular vein and in the medial, mid, and distal portions of the subclavian vein. The vessel walls are thin and the lumens are generally anechoic, unless slow flow is present. Normal venous valves are easily visualized as thin leaf-like mobile structures and should not be mistaken for wall-adherent thrombus or sequelae from prior thrombosis. Diagnostic criteria for upper extremity venous thrombosis by ultrasound are similar to those described for lower extremity deep venous thrombosis. B, Sagittal image demonstrates the same thrombus (arrows) filling and distending the vessel. Color Doppler flow imaging makes visualization of anechoic and nonocclusive thrombus easier because it permits direct visualization of blood flow dynamics. Nonocclusive thrombus will generally be outlined by color and demonstrate some evidence of flow in the vessel. Generally, as thrombus becomes more chronic, its echogenicity increases and the clot retracts, with resultant decrease in the distention of the vessel. The visualized thrombus may be more eccentric and focal in location within the vessel lumen, with skip areas present. Although some veins may regain a normal appearance and compressibility over time, other vessels may demonstrate sequelae of chronic venous disease, such as frozen valve leaflets, synechia, and partial recanalization of the vessel. The affected native vessel may collapse and fibrose, with resulting collateral formation. In vessels in which thrombus has resolved, venous insufficiency or reflux may later be present. The diagnosis of recurrent thrombosis or acute thrombosis superimposed on chronic thrombosis is problematic by ultrasound. The normal spectral Doppler waveform of the upper extremity and neck veins are characterized by two phasic variations. Right atrial contraction results in a sawtooth pattern to the waveform, which is synchronized to the pulse rate. Superimposed on this cardiac pulsatility is a phasic change in amplitude caused by the respiratory cycle. Sniffing can cause momentary collapse of a normal vessel; a Valsalva maneuver will cause the vessel to distend and velocity of venous flow to decrease. Loss of cardiac pulsatility has been reported as a more sensitive predictor than loss of respiratory phasicity alone. Conversely, the demonstration of normal cardiac and respiratory phasicity is highly predictive of the absence of thrombus in these vessels. Longitudinal and transverse color Doppler flow images (B, C) demonstrate thrombus outlined by color (arrows). Bilateral dampening, however, can occur with thrombosis of the superior vena cava. As noted, considerable constraint is placed by the normal anatomy of the region, with the clavicle, manubrium, and sternum limiting visualization and compressibility of the veins, especially centrally. Compression may also be limited by body habitus, overlying bandages, or indwelling catheters. Color Doppler imaging may aid in the detection of nonocclusive thrombus, but care must be taken not to oversaturate the images with color, which can obscure thrombus. One should look carefully for swirling or slow-moving particles on real-time imaging, the presence of which will distinguish slow-flowing blood from true thrombus.
Purchase finast overnight delivery
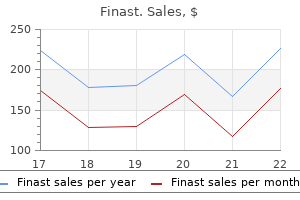
A subcutaneous test dose is no longer given because of the immune response it may generate in the patient hair loss in men 70s fashion buy 5mg finast with amex. If 131 I or 123I is employed, oral potassium iodide is given to block thyroid uptake of free radioactive iodide. In addition, blood pool subtraction techniques are required for 131I studies to simulate the non-tumour distribution of labelled antibody. Following injection of the antibody, a gamma camera provides serial images of the distribution and uptake of radiolabelled antibody between 18 and 72 h after the antibody has been administered. Excretion of 111In into the bladder has not been a problem, although non-specific bowel uptake may account for false-positive results. A central area of increased uptake is apparent at the site of a primary ovarian cancer. It is an analogue of glucose, thereby reflecting metabolism and detecting the increased glycolysis associated with several tumour types. It gains entry into cells by membrane transporter proteins, such as Glut-1, which are expressed in many tumours. Angiography Diagnostic and therapeutic angiography have made great strides in recent years with the development of catheters whose tips can be manipulated. This allows considerable control over the guidance of these catheters into selected vessels. In parallel with this, ingenious devices have been devised which can be introduced via these catheters for purposes as diverse as angioplasty and embolization. In gynaecological practice, the main use of angiography is the control of pelvic bleeding, but both the diagnosis of pelvic venous thrombosis and the prevention of subsequent pulmonary embolism are important roles for this exciting new technique. Pelvic arteriovenous malformations are most readily diagnosed and treated with angiography, and pelvic varices causing chronic pain may be managed in the same way. Selective sampling of gonadal venous blood and steroid hormone assay can be valuable in the preoperative assessment of phenotypic women with chromosomal abnormalities and intra-abdominal gonads of uncertain nature. Clinical Applications Normalanatomyandvariations Uterus the normal uterine cavity is delineated as a triangular structure on hysterosalpingography, with the cornua and the internal cervical os as the corners. Similar information can be acquired with ultrasound following instillation of saline into the uterine cavity (hysterosonography) (van den Brule et al 1998). On ultrasound, the uterine cavity is normally represented by a bright line of apposition of the endometrial layers, although occasionally a trace of fluid can be seen at menstruation. In adolescence, it may be caused by vaginal atresia, where the upper vagina dilates more than the uterus so that haematocolpos dominates the picture, while in postmenopausal women, cervical stenosis, either fibrotic or malignant, must be considered. The endometrium is seen as an echogenic layer of uniform texture, often with a fine echo-poor margin. Its thickness varies through the menstrual cycle from 12 mm premenstrually (double-layer thickness) to a thin line after menstruation. On T2-weighted images, the endometrium is seen as a central high-signal stripe which increases in thickness in the secretory phase of the menstrual cycle. The inner myometrium (junctional zone) is of lower signal intensity than the outer myometrium on T2 weighting, and correlates histologically with a layer of more densely packed smooth muscle. In this scan, taken in the luteal phase of the cycle, the secretory endometrium is seen as an echogenic band in comparison with the relatively echo-poor myometrium. Ultrasound contrast salpingography is currently being evaluated to reduce the radiation dose to the ovaries in patients trying to conceive. Normal uterine tubes cannot be demonstrated on ultrasound, but instillation of microbubble contrast agents into the uterus and tubes permits their visualization and can be used as an initial screening test for tubal patency. Although 63 5 Imaging techniques in gynaecology the anatomical detail is less than that offered by conventional X-ray salpingography and false-positive results occur, this technique of ultrasound salpingography seems likely to find an important role as an initial screen; if the tubes are demonstrated to be patent, no further investigation is necessary and this should result in a reduction of radiation exposure (Van Voorhis 2008). Ovaries the ovaries are best imaged with ultrasound (either transabdominal or, preferably, transvaginal). Infantile ovaries are small (except in the neonate when hypertrophy and follicles stimulated by maternal hormones may be a surprising finding) and they enlarge before puberty. Follicular development begins before menstruation, but these cycles and those at the menopause are often imperfect so that follicles may persist and continue enlarging for several months. In doubtful cases, a rescan at 6 weeks to image them at a different phase of the cycle may be needed to resolve their identity. Ovarian varices the pelvic congestion syndrome is one of many causes of chronic pelvic pain, and is associated with the presence of large varices within the broad ligaments (Liddle and Davies 2007). It is surrounded by a small amount of free fluid and contains minute developing follicles. These vessels are best demonstrated by selective ovarian venography, although they may also be imaged with Doppler ultrasound (Haag and Manhes 1999). Venography is performed via a femoral or internal jugular venous approach, and the ovarian veins are selectively catheterized with an appropriately shaped angiographic catheter. Satisfactory retrograde opacification of pelvic varices is achieved by injecting contrast medium through the selectively placed catheter with the patient almost upright on a tilting table, while the Valsalva manoeuvre is performed. Treatment of this condition is primarily surgical and consists of venous ligation. Symptomatic relief has been reported following transcatheter ovarian vein embolization (Ganeshan et al 2007). Adenomyosisandendometriosis the diagnosis of adenomyosis is often suggested by symptoms of hypermenorrhoea and dysmenorrhoea, but similar symptoms are also produced by leiomyomas. Hysterosalpingography may show multiple small tracks of contrast extending into the myometrium but is now obsolete. Pathologically, this represents smooth muscle hypertrophy and hyperplasia surrounding a focus of basal endometrium. Values for junctional zone thickness from >5 to >12 mm have been suggested for the diagnosis of adenomyosis. Structures within the follicle, such as the cumulus oophorus, can also be visualized. Transvaginal sonography has largely replaced the transabdominal approach in infertility practice because of the superior anatomical display and because it allows precisely guided aspiration of follicles and fluid in the pouch of Douglas. More precise measurement of follicles is possible, and the corpus luteum is easily recognized. Endometrial reflectivity patterns have been proposed as another way to assess ovulation (Randall et al 1989). Ultrasound is also useful for accurate timing of artificial insemination, while a postcoital test can help to differentiate between inadequate sperm penetration and poor mucus production in the presence of immature follicles. Ultrasound scanning is also employed to monitor patients on clomiphene therapy, and there is good correlation between follicular diameter and plasma oestradiol concentration. Ovarian hyperstimulation syndrome is uncommon if gonadotrophin therapy is monitored by ultrasound in conjunction with measurements of plasma oestradiol levels. Diffuse infiltration of a mixed-signal lesion (long arrow) is seen in the posterior wall. In these instances, absolute values for junctional zone widths are unhelpful (Hauth et al 2007), and ratios to the width of the outer myometrium or the cervical stroma may be more meaningful. The lesions of endometriosis are difficult to detect with imaging techniques, mainly because of their small size. Endoscopic ultrasound has been advocated to improve the diagnosis of endometriotic infiltration into the digestive tract (Dumontier et al 2000). Deep pelvic endometriosis consists mainly of fibromuscular rather than endometrial tissue (Del Frate et al 2006), and often goes undetected on visual inspection of the pelvic cavity because of its position.
Buy line finast
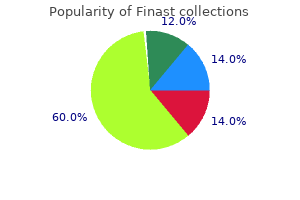
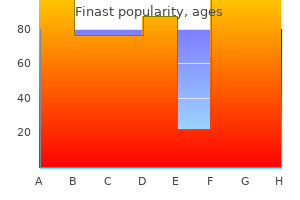
These effects are analogous to those induced by modulation in diathermy output which leads to the differences between cutting and coagulation diathermy referred to earlier hair loss 6 months after giving birth cheap finast 5 mg overnight delivery. Very short pulses, such as those produced by Q-switched lasers, can cause electromechanical breakdown in tissues because of the extremely high energy densities obtainable. In the early days, these lasers were tested in gynaecology but untoward side-effects were noted (Minton et al 1965). These will be described in detail, with a further section devoted to other types of laser which are now entering general usage after extensive research. Carbon dioxide laser this is the system which has been most used in gynaecology since it was used for the first time in 1973 for the treatment of cervical erosions. This has been because of its clinical stability, ease of use, reliability and easy serviceability. It is a precise laser, especially in ultrapulse mode, making it useful for division of adhesions and accurate and safe vaporization of deposits of endometriosis (Sutton 1993). Although a major drawback is that its output cannot be transmitted by fibres, it has so far not been totally displaced by other lasers but is rivalled by modern diathermy equipment. Sealed tube lasers are now available with radiofrequency low-voltage discharges being used for excitation. This radiation is absorbed rapidly by tissue water, and therefore cuts and vaporizes more easily than it coagulates. At each joint, there is a mirror which is adjusted so that the beam stays central despite movement between the two adjacent limbs of the arm. It is possible to use waveguide delivery systems to avoid the use of mirrors, but this limits the manoeuvrability of the complete system. The final delivery to the operation site can be carried out in two ways, both incorporating a focusing lens. For handheld surgery, the lens at the end of a straight delivery tube focuses the beam on the operative field approximately 1 cm from the end of the tube. Colposcopic delivery involves a mirror after the focusing lens which brings the beam into line with the viewing axis of the colposcope. Originally the spot size was changed using lenses of different focal lengths and so was limited to three or four predetermined sizes. Nowadays, the use of zoom optics allows infinite adjustment over a limited range (0. Pumping is achieved by energy input from a parallel gas discharge lamp, usually a water-cooled krypton tube, with the output radiation being refocused into the laser crystal. Output power levels up to 100 W continuous can be achieved, but, with a conversion efficiency of 1% or so, nearly 10 kW of input power is needed. This is particularly necessary where contamination with blood or blood products may make continuous operation difficult. An HeNe laser (or other light source) needs to be incorporated into the device as an aiming beam. This is also a very useful safety feature as near-infrared radiation can cause irreparable damage to the retina. An optoelectronic switch is incorporated inside the laser cavity and the lasing action is prevented for a large percentage of the time. The photon energy therefore builds up to an even higher level than normal, and when the switch is eventually opened, a massive pulse of energy is delivered. This type of action has found a use in ophthalmology where, by focusing the pulse to a very small spot, electromechanical breakdown of tissue can be induced with minimal surrounding damage. Hysteroscopic procedures include removal of fibroids and polyps, transsection of uterine septae, lysis of adhesions and endometrial ablation. The copper vapour and dye laser combination can produce over 5 W of red light at 630 mm, which is an absorption peak of haematoporphyrin derivative. The main disadvantage of the light lasers is the need to wear special protective glasses which can distort the view of the pelvis. Other laser systems Many other laser systems are used in medicine and the time period from research to common usage seems to be getting shorter. It is neither possible nor desirable to give a complete list, but some of the following examples have potential benefits for gynaecological surgery. Ultraviolet lasers Research into ultraviolet lasers has produced systems which seem to rely on non-thermal mechanisms for tissue destruction. These lasers have found a place in ophthalmology, and their potential for precise tissue removal offers the microsurgeon a very powerful tool. The early use of lasers in gynaecology was in the treatment of cervical intraepithelial neoplasia, but subsequently spread to most other areas of the lower reproductive tract. The use of the laser in treatment of intraepithelial neoplasia of the genital tract is described in Chapter 38. We are under pressure to decrease health costs, so alternative, less-expensive technology has reduced the use of laser technology in recent years. However, lasers are still used in various clinical settings in obstetric and gynaecological surgery. Other uses are being investigated, but the evidence on safety and efficacy outcomes thus far is insufficient to support use in a non-research environment. Examples of these include laparoscopic laser myomectomy and percutaneous laser therapy for fetal tumours. There are also controversial areas regarding the use of lasers which have entered commercial gynaecology without much regulation or scientific evaluation, such as laser vaginal rejuvenation. Metal vapour lasers As their name implies, metal vapour lasers consist of a container filled with a heated and vaporized metal in an inert gas atmosphere at low pressure. The copper vapour laser produces two beams at 510 and 578 nm at up to 25 W power output. These by themselves are not particularly useful, although the green can be used as a substitute for the argon laser in dermatology. The output is ideally suited to act as an optical pumping source for a dye laser, which can be tuned to provide radiation for photodynamic therapy. Photodynamic therapy Photodynamic therapy is a treatment for certain tumours (Spikes and Jori 1987). It relies upon selective retention in tumour tissues of a drug (photosensitizer), such as haematoporphyrin derivative, which only becomes active on exposure to light of a particular wavelength. Each photosensitizer has a particular spectrum of action requiring light of the appropriate wavelength for maximum absorption and effect. As there are many decay pathways 56 Lasers Lasersafety All laser systems in current use have no way of distinguishing between patient and operator. The subject of the safe construction and operation of lasers in medicine and surgery is thus very important and must be understood by all involved. A further publication by the Medicines and Healthcare Products Regulatory Agency (2008) outlines good laser practice together with some additional equipment safety features. All these publications should be considered by a laser protection adviser (a health authority or trust appointee) who will assist each user in specifying and installing lasers in clinical surroundings. Although the requirements will vary from laser to laser and from site to site, the following sections outline the major considerations involved. Nature of hazard the body is divided into two regions for hazard analysis: the eye and the skin. In the visible region, which extends into the near-infrared, the eye is the organ at greatest risk. Outside this range, the eye is no different from the skin, except that corneal damage can lead to visual loss although the retina itself may be undamaged. Maximum permitted exposure levels are laid down by the regulations and are set well below known damage thresholds. Manufacturing and administrative controls are written to prevent operators, assistants and patients from accidentally receiving radiation in excess of these limits. There are separate values for the skin and the eye, with the latter being the more stringent.
Order finast 5mg without prescription
A third of women who become isoimmunised have no demonstrable antibodies at the first antenatal visit hair loss legs order finast in india, so investigations for antibodies must be repeated during pregnancy in RhD-negative women. There is a correlation between the time of first antibody detection and the severity of haemolytic disease of the newborn. The earlier the antibodies are present during the pregnancy, the higher the risk of fetal/neonatal problems. If an antibody is present in pregnancy, serial monitoring of antibody levels is required. Prevention of RhD isoimmunisation the aim is to provide passive immunisation at times of risk of fetomaternal transfusion. Pregnancies after this involve a greater severity of fetal neonatal haemolytic disease. Other red cell antibodies There are about 700 red cell antibodies, but only a few cause severe haemolytic disease of the newborn. Many antibodies (A, P(I), Le(a), M, I) produce an immunoglobulin M (IgM) response only, which cannot cross the placenta, so they are of no significance in pregnancy. Some red cell antigens are poorly developed on fetal red cells, so antibodies (Lu(b), Y+(a)), even if IgG produced and crosses the placenta, have no adverse affect. There appears to be a poor correlation between the antibody titre and the effect on the fetus or neonate. Management the management of all red cell antibodies is similar in principle to Rhesus disease, including paternal genotype, serial titres, assessment of fetal anaemia and early delivery. It occurs in 15% of pregnancies, but only 1 in 30 show mild jaundice, 1 in 150 mild anaemia, and 1 in 3000 require exchange transfusion. Antepartum haemorrhage is bleeding from the genital tract in the period from 20 weeks gestation to the birth of the baby. It occurs in 3% of pregnancies of >28 weeks gestation and 5% of pregnancies of >20 weeks gestation. The placenta is attached to the lower segment of the uterus and/ or covering the cervix. The presentation is usually that of a painless antepartum haemorrhage with a high presenting part. Placenta percreta Invasion of the placenta to within the myometrium should be suspected in previous cases of placenta praevia. This is especially so in the case of placenta praevia and previous caesarean section where the rate of placenta acreta is 5%. As there is a significant risk of major haemorrhage, delivery via caesarean section should be well planned with blood products available and counselling of the possibility of hysterectomy. Abruption is haemorrhage from decidual detachment of a normally situated placenta. The woman presents with abdominal pain, tense and tender uterus, which is large for dates, and hypovolaemic shock that may be out of proportion with visible bleeding. It is often associated with velamentous insertion of the cord, with vessels present within the fetal membranes. Diagnosis Vasa praevia must be included in the differential diagnosis of intrapartum vaginal bleeding, and is associated with an ominous cardiotocography pattern. Diagnosis can occur in the antenatal period with transvaginal ultrasound and colour Doppler assessment of vessels across the top of the cervical os. In the presence of blood loss and ominous fetal heart rate, although theoretical tests (Apts) are available, vasa praevia may result in fetal anaemia and death. The intrauterine diagnosis is via the absence of fetal heart sounds and fetal movements. Aetiology Aetiology varies with gestational age and between developed and non-developed countries. There is a slow reduction in fibrinogen of about 500 mg/L per week, which is unlikely to be associated with bleeding tendency until levels are lower than 1 g/L. The coagulopathy is due to fibrinogen consumption with release of thromboplastins from retained products of conception. There may also be raised fibrin degradation products, prothrombin time and activated partial thromboplastin time with a reduction in platelets. Spontaneous labour occurs in 80% of cases within 2 weeks, with only 10% undelivered after 3 weeks. External cephalic version Spontaneous changes in fetal polarity are reduced with increasing gestation. The likelihood of spontaneous version at 32 weeks is about 55%, compared with 25% at 36 weeks. The risks of external cephalic version include tocolytic side effects, placental abruption, cord accidents and premature labour. The absolute contraindications to external cephalic version include multiple pregnancy, antepartum haemorrhage, placenta praevia, rupture of membranes, labour and fetal abnormalities. Term Breech Trial this randomised multicentre trial compared the policy of elective caesarean section with vaginal birth for selected breech deliveries. Breech born by maternal expulsive efforts up to the umbilicus After the knees have delivered, flex the knees by pressing on the popliteal fossa to deliver the legs. The head is delivered by various ways, including forceps, the Mauriceau-Smellie-Veit manoeuvre, the Wigand-Martin manoeuvre of suprapubic pressure and lateral rotation of head in pelvis, or the Bracht manoeuvre of grasping feet and placing the body onto the maternal abdomen with the symphysis acting as fulcrum. This occurs as a result of duplication of the normal process of conception, with separate chorions, amnions and placental circulations.

Proven finast 5mg
In part hair loss in menopause cures buy generic finast 5 mg line, this promiscuity can be attributed to the degree of hormonal stimulation or activation of different receptor subtypes. Calcium ions also activate cytosolic guanylate cyclase, an enzyme that catalyses the formation of cyclic guanosine monophosphate. The latter are well-recognized paracrine and autocrine mediators capable of amplifying or prolonging a response to a hormone stimulus. C Nuclearreceptors the nuclear receptors are classified by their ligands, which are small lipophilic molecules that diffuse across the plasma membrane of target cells. The receptor family predominantly resides in the nucleus, although increasingly nuclear import and export appears to be an important regulatory mechanism, as has been long recognized for the glucocorticoid receptor. The receptors have their primary effect by regulating the expression of specific target genes. Consequently, this need for transcription and translation to elicit a biological effect means that cellular responses are relatively slow compared with cell surface receptor signalling. The extracellular domain is ligand specific and hence less conserved across family members. The transmembrane domain has a characteristic heptahelical structure, most of which is embedded in the cell membrane and provides a hydrophobic core. Conserved cysteine residues can form a disulphide bridge between the second and third extracellular loops. The cytoplasmic domain links the receptor to the signal-transducing G-proteins and, in this example, is linked to membrane-bound adenylate cyclase. Target cell conversion of hormones destined for nuclear receptors A further characteristic of several nuclear hormone receptors includes enzymatic modification of the ligand within the target cell. This converts the circulating hormone into a more, or less, potent metabolite prior to receptor binding. An extreme example of this is the inactivation of cortisol to cortisone by type 2 11-hydroxysteroid dehydrogenase, which occurs in the placenta, thereby minimizing exposure of the fetus to maternal cortisol. This signalling pathway regulates major metabolic pathways, including those for lipolysis, glycogenolysis and steroidogenesis. Hormone specificity of the receptor this is the most important factor which determines specificity of action and occurs at two levels (King 1988). The presence or absence of a given receptor determines whether or not a cell will respond to a given class of steroids, whilst hormone specificity controls which particular compound is active. Free steroid in equilibrium with that bound to protein (A) diffuses across the target cell membrane (B). This recognition specificity is a reflection of the different affinities that the receptor has for the different hormone structures. In biological terms, this means that oestradiol is more active than oestrone, whilst testosterone can have oestrogenic effects but only at pharmacological concentrations. It is notable that the oestrogen receptor is not a single entity and that it is not restricted to the reproductive system. These receptors are functionally distinct, having different tissue distributions and different ligand activation, and as such play different roles in gene activation. Notably, the binding of oestradiol or selective oestrogen receptor modulators such as raloxifene (see below) to the receptor leads to oestrogen agonism and antagonism according to which receptor the ligand has bound to (see below) (Kearney and Purdie 2000). Androgen, glucocorticoid, progestogen and mineralocorticoid receptors are less precise in their binding requirements than the oestrogen receptor (Beato and Klug 2000). For example, many progestogens, especially the synthetic ones, bind to both progestogen and androgen receptors when present in pharmacological concentrations. For example, the practice of giving synthetic progestogens to pregnant women to prevent miscarriage resulted in some of their offspring having clinical features associated with androgen exposure (Aarskog 1979). The androgenic side-effects of the synthetic progestogens used in the oral contraceptive pill are another example. On binding of steroid to the receptor, there is a conformational change and the heat-shock protein is dissociated, revealing two polypeptide loops stabilized by zinc ions, known as zinc fingers, facilitating dimerization and the binding of cofactors which will promote (coactivators) or inhibit (corepressors) the interaction of the receptor to its target genes. An understanding of basic methodology permits the clinician to have confidence in the selection of specific laboratory tests, and leads to a greater understanding of the assay for better interpretation of results (Chard 1987). The three types of analytical procedure commonly available in clinical practice are physiochemical assays, bioassays and binding assays. Physicochemicalassays Some aspect of the physicochemical properties of a compound is utilized for its quantification. These are the assays used to measure some steroid hormones or intermediaries from their biosynthetic pathways. Techniques such as highperformance liquid chromatography or gas chromatography coupled with mass spectrometry are becoming increasingly used, and provide a definitive approach to the identification and quantification of hormones based on their physical characteristics. The hormone receptors and hence the assays derived from them have high affinity and hormone specificity, often generating favourable sensitivity, precision and sample capacity. Bioassays Detection or quantification is dependent on the biological actions of the compound. In-vivo bioassays investigate the biological potency of a hormone following its administration to an animal and quantification of a specific response. For example, human pregnancy could be diagnosed by the injection of maternal urine into the Black African Toad. Invitro bioassays measure biological effects when hormone is added to an isolated laboratory preparation of the target tissue. For example, in the bioassay of prolactin, when neural tumour cells grown in culture are exposed to prolactin, they replicate. Immunoassays A reaction, which reaches equilibrium, occurs between the hormone to be measured (antigen) and an antibody to monitor the reaction. The basic binding reaction can be subdivided into two categories, based on whether the antibody is present in a limited concentration or whether it is present in excess. The principle of an immunometric assay is that a constant amount of antibody is added with increasing known amounts of the reference hormone. After incubation, the amount of hormone bound to the antibody is detected by adding, to all the tubes, an excess amount of a second labelled anti-hormone antibody. The second antibody is directed against a different antigenic site on the hormone from the first antibody. Thus, a triple complex is formed, with the hormone sandwiched between the two antibodies. The unbound fraction of the second antibody is removed, leaving the amount of triple complex to be determined by quantifying the bound label; for example, by measuring the radioactivity or fluorescence emitted. This emission is plotted against the increasing known amount of hormone standard to generate a calibration curve. To determine the standard curve with precision, against which patient samples can be interpolated, usually five to eight Bindingassays these assays involve the combination of the compound, for example, an antigen, with a binding substance, for example, an antibody, which is added in a fixed amount to the solution. Binding assays can be further subdivided into three groups: receptor assays, competitive proteinbinding assays and immunoassays. The immunometric assay is only suitable when the hormone to be measured is large enough to permit the discrete binding of two antibodies. Enzymoimmunoassay, enzymoimmunometric assay and enzyme-labelled immunosorbent assay are currently the most widely used non-isotopic labels. Small quantities of antigen can be quantified by studying enzymatic substrate conversion that leads to a colour change. The second marker antibody will not be bound, so following the wash step, it will not be present to react with its substrate. The action of the individual hormones is discussed in further detail in the relevant chapters. Levels also change across gestation, and specific pregnancy ranges are required to ensure adequate thyroxine replacement in women with hypothyroidism. Deficiency of the thyroid hormones triodothyronine (T3) and T4 leads to anovulation associated with increased gonadotrophin levels. Therefore, it is important to assess thyroid function in the work up of oligoamenorrhoea and prior to diagnosing premature ovarian failure Circulating thyroid hormone is tightly bound to a group of proteins, chiefly thyroxine globulin. Oestrogen produces a rise in thyroxine-binding capacity and, therefore, thyroid function tests are affected by pregnancy and oestrogen-containing medications such as the contraceptive pill. Consequently, a raised thyroxine level does not mean that the free thyroxine concentration (the unbound and metabolically active hormone) is above the normal range.
Generic finast 5mg visa
Tubal secretions contain proteins that derive from the plasma and also some specific substances synthesized within the oviduct itself (Maguiness et al 1992a) hair loss in pregnancy 5mg finast amex. Both tubal proteins and the physical contact between the gametes and the tubal epithelium may play a role in gamete function. Aetiology of Tubal Disease Tubal disease is usually defined as tubal damage caused by pelvic infection such as pelvic inflammatory disease or tuberculosis, endometriosis, surgery or salpingitis isthmica nodosa, with varying degrees of tubal damage or obstruction, sometimes involving the adjacent ovary and the pelvic peritoneum, and adhesion formation. As a result, patients with tubal damage suffer from infertility and/or pelvic pain. This definition does not cover functional defects of the fallopian tube, as our ability to describe tubal disease is currently limited to demonstrating its patency and macroscopic normality. Salpingitis Most salpingitis is the result of an ascending infection from the lower genital tract, caused primarily by Chlamydia trachomatis and Neisseria gonorrhoeae (see Chapter 61, Pelvic inflammatory disease, and Chapter 62, Sexually transmitted infections, for more information). These micro-organisms cause mucopurulent endocervicitis, and break down major cervical barriers, such as the mucus plug that protects the endometrium and upper genital tract, and permits ascending infection. In a significant proportion of cases, no aetiological agent is identified; this suggests that a range of other aetiological agents have a role, but the identification of novel organisms is difficult to ascertain because of the limited availability of diagnostic tests. Serological evidence has associated Mycoplasma genitalium with pelvic inflammatory disease (Simms and Stephenson 2009). In the majority of patients, salpingitis is due to a sexually transmitted infection. In other cases, iatrogenic manoeuvres such as insertion of an intrauterine device, termination of pregnancy, hysterosalpingography or curettage can spread a cervical infection into the uterus and tubes. In a small proportion of women, pelvic infection may be secondary to gastrointestinal infections such as perforated appendicitis. Mycobacterium tuberculosis is still seen in developing countries; however, migration to developed countries has resulted in a significant increase in the number of tuberculosis notifications since the 1980s (Rose et al 2001). Acute salpingitis causes loss of ciliated cells and distal occlusion of the fallopian tubes. Some of the deciliation may be recovered later, but subsequent immune response following the acute phase causes permanent scarring, loss of mucosal folds and flattening of the mucosa (Lyons et al 2006). Distal occlusion of the tubes together with chronic inflammatory process could result in fluid collection in the lumen of the fallopian tube, leading to hydrosalpinges. Pelvic peritonitis during the acute phase may be followed by adhesions around the fallopian tubes and ovaries, distorting the pelvic anatomy. Othercauses Endometriosis, fibroids, previous pelvic/tubal surgery, salpingitis isthmica nodosa, endosalpingiosis and cornual polyps can be the cause of cornual obstruction or tubal damage. In some patients, tubal damage is secondary to previous tubal or pelvic surgery such as salpingotomy for ectopic pregnancy, ovarian cystectomy, myomectomy, ovarian wedge resection and shortening of round ligaments. Salpingitis isthmica nodosa was described by Chiari (1887) as nodular thickening of the proximal part of the fallopian tube. The aetiology of this entity is unknown but it is probably due to a noninflammatory process. Diagnosis Assessment of the fallopian tube should normally determine patency, a normal external and internal appearance, the ability to transport gametes and the embryo, and provision of an environment for the early steps of reproduction to occur. It is possible that, apart from the obvious need for tubal patency to allow passage of gametes, factors that affect the gametes and embryo, the effectors of tubal transport, the cilia, flow of tubal fluid and tubal contractions appear to constitute a higher-order system in which intact function of each may not be needed to achieve pregnancy (Verdugo 1986). Treatment may be the reason for unsuccessful tubal surgery even when tubal patency has been achieved. Similarly, a functional disorder of this system may account for subfertility in some cases of unexplained infertility. Currently, tubal function is determined by demonstrating patency and normal appearance at laparoscopy. The first two methods have been used for many years, whereas HyCoSy is a relatively new technique. All these methods have some degree of false-negative and false-positive results in determining tubal patency. Laparoscopy has the ability to identify peritubal adhesions, endometriosis, polycystic ovaries, and other pelvic and intra-abdominal pathology. However, it is usually performed under general anaesthesia and does not give information about the uterine cavity. Salpingoscopy is the transabdominal examination of the tubal lumen by introducing an endoscope through the fimbrial end. The presence of minor intratubal lesions is not necessarily incompatible with fertility (Maguiness and Djahanbakhch 1992); however, loss of mucosal folds and intratubal fibrosis are significant. Nowadays, salpingoscopic assessment of the tubal lumen is recommended by some groups before tubal surgery for hydrosalpinges (Puttemans et al 1998). De Bruyne et al (1989) proposed a classification of ampullary findings in hydrosalpinges: grades 1 and 2 refer to normal salpingoscopic findings, grade 3 (intermediate group) refers to focal adhesions, and grades 4 and 5 refer to severe adhesions and loss of mucosal folds. Transvaginal hydrolaparoscopy and fertiloscopy approaches utilize the advantages of laparoscopy but with a less invasive approach (Gordts et al 1998, Watrelot et al 1999). Transvaginal hydrolaparoscopy is the endoscopic examination of pelvic structures through the posterior vaginal fornix after instilling saline into the pouch of Douglas. This allows tubal patency to be checked, in addition to assessment of the pelvis for other pathology. Fertiloscopy includes salpingoscopy, microsalpingoscopy and hysteroscopy for complete examination of the female reproductive tract. Selective transcervical salpingography and tubal catheterization can be done in cases where it is doubtful that there is cornual obstruction (Ataya and Thomas 1991). Irregular vessels seen on the peritoneum surface as a result of previous inflammation (arrow). However, it is relatively expensive, labour intensive and carries risks of multiple pregnancy and ovarian hyperstimulation syndrome (see Chapter 22, Assisted reproduction treatments, for more information). Cornual occlusion Cornual occlusion due to inflammatory causes was treated by uterotubal implantation with very poor results. Ehrler (1963) described his technique and suggested that the intramural portion of the tube could be spared in most patients. Microsurgical methods described by Winston (1977) and Gomel (1977) became the surgical technique of choice. Destroying a possible sphincter at the uterotubal junction is associated with excessive bleeding and damage to the tubal blood supply; it shortens the tube and may increase the risk of rupture of the uterus in the event of subsequent pregnancy, which means that patients must be delivered by caesarean section. The use of magnification allows better identification of the intramural portion of the tube by careful shaving of the cornua until healthy tissue is found, permitting a more accurate tissue apposition with a watertight anastomosis between healthy tubal tissues. Once the ends are well defined, the anastomosis is done in two layers, using 8/0 nylon as a suture. The suture material should not penetrate the mucosa, only the muscularis (Seki et al 1977). A stitch of 6/0 Prolene between both ends of the mesosalpinx should be applied as a stay suture. More details about the technique have been given elsewhere (Winston 1977, Margara 1982). A review of the literature on fluoroscopic tubal cannulation showed pregnancy rates of 22. However, this type of surgery is still appropriate and effective for properly selected individuals (National Institute for Clinical Excellence 2004). The use of magnification and microsurgical techniques has been the traditional method. However, with advances in laparoscopic surgery, most of these methods are now possible to perform at laparoscopy. In some of them, the surgical freeing of the ovaries and tubes from adhesions can give symptomatic relief. Microsurgicaltreatment the microscope was first used for tubal surgery by Walz (1959). Whilst others used delicate electrosurgery and magnification (loupes) in the treatment of hydrosalpinges, Paterson and Wood (1974) in Australia and Winston and McClure-Browne (1974) in England adapted their experience from animal experiments to humans and operated on infertile women, under high magnification, using an operating microscope. The use of the microscope was originally much debated, but microsurgery is now well established and is a routine procedure for tubal infertility. Glazener et al (1987) stated that the removal of cornual polyps does not improve fertility and they are not a cause of infertility. However, consideration should be given to removal of large polyps present in the intramural or isthmic portion of the tube.
Order finast online now
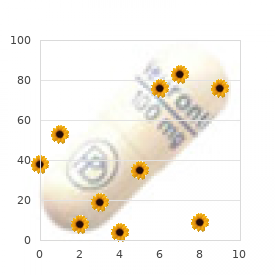
That said hair loss prevention mens health buy cheap finast 5mg on-line, there are some not uncommon pitfalls in patients presenting with pulseless, cool, painful extremities. In patients suffering from aortic bifurcation saddle embolus, the diagnosis is frequently missed, as discussed before. These patients are often evaluated for possible neurologic or neurosurgical problems owing to the bilateral paralysis on presentation, resulting in a delay of diagnosis and appropriate therapy. Aortic dissection can cause acute arterial insufficiency of one or both legs and must be considered in any patient presenting with a cold pulseless limb and abdominal, back, or chest pain. In some cases, percutaneous aspiration or mechanical thrombectomy is used before and in conjunction with thrombolysis. It is essential that any stenoses revealed on arteriography after thrombolysis be treated with angioplasty, bypass graft revision, or revascularization. In the interim from completion of thrombolysis until intervention directed at flowlimiting lesions, heparin infusion must be continued. Maintenance intravenous fluids should be initiated and the patient kept nil per os. Consideration should be given to either oral acetylcysteine14 or bicarbonate infusion15 if the patient has chronic renal insufficiency or diabetes because diagnostic or completion angiography will likely be indicated. Temperature extremes and fluctuations should be avoided; cold temperatures cause vasoconstriction, and heat causes increased tissue metabolic demands. Transfusion and optimization of cardiac output should be accomplished whenever these might result in improved oxygenation of the affected limb. Stents were placed in the newly patent left iliac limb to displace residual thrombus and to treat any stenoses that might have contributed to the thrombosis. Aortic occlusion may result from aortic saddle embolus, in situ thrombosis of an atherosclerotic abdominal aorta, thrombosis of an abdominal aortic aneurysm, or aortic dissection. It is important to establish the etiology of aortic occlusion because balloon catheter embolectomy through a femoral cutdown (see later) is usually successful in the setting of saddle embolus but is infrequently helpful in patients with in situ thrombosis of a chronically diseased abdominal aorta. In the latter scenario, the limbs are usually not profoundly ischemic owing to the chronic nature of the disease and resulting extensive collateralization; these patients may require aortobifemoral grafting to reestablish lower extremity perfusion. Acute unilateral iliac occlusion can occur in patients having undergone prior aortic aneurysmorrhaphy with a bifurcated graft, prior aortobifemoral reconstruction, or prior abdominal aortic stent grafting. In these situations, the surgeon may be able to restore patency of the graft limb with balloon thrombectomy performed from a groin incision, but a technical problem in the affected limb and graft stenosis must be suspected and subsequently addressed. Symptomatic popliteal aneurysms generally present with limb ischemia-from aneurysm thrombosis or distal thromboembolism-rather than with rupture. The diagnosis should be suspected in any patient with acute or chronic ischemia of the leg and a palpable firm pulseless (in the case of thrombosis) or pulsatile mass behind the knee. Treatment of a popliteal aneurysm presenting with acute limb ischemia consists of emergent catheter-directed thrombolysis to reestablish distal arterial patency20 and subsequent surgical exclusion and bypass; resection of the aneurysm is not necessary. There is also an emerging experience with covered stents for treatment of popliteal aneurysms. In patients suffering from thrombotic arterial occlusions and in those whose thromboembolism cannot be extracted or lysed, arterial bypass grafting may be necessary to treat stenotic or occluded vascular segments. Surgical arterial bypass and other revascularization procedures are detailed in Chapter 114. Chronic limb ischemia presents as a spectrum of disease from asymptomatic to claudication to critical limb ischemia. This spectrum is encapsulated in two similar staging systems for peripheral arterial disease: Fontaine stages and Rutherford categories (Table 113-4). Symptomatic patients with peripheral arterial disease generally present with either intermittent claudication or critical limb ischemia. Intermittent claudication is defined as muscle discomfort in the lower limb reproducibly produced by exercise and relieved by rest within 10 minutes. Critical limb ischemia is defined as persistent, recurring ischemic rest pain requiring opiate analgesia for at least 2 weeks with ulceration or gangrene of the foot or toes. Hence, Rutherford categories 4 through 6 comprise those patients with critical limb ischemia. However, the rational construct differentiating patients with immediately threatened limbs and those with chronically threatened legs is clinically useful. Prevalence and Epidemiology Intermittent claudication has a prevalence of approximately 3% in 40-year-olds and about 6% in 60-year-olds. However, continued smoking or coexistent diabetes portends worse clinical outcomes for claudicants, including more frequent eventual amputation. Critical limb ischemia has an incidence in the United States of approximately 1000 new cases per 1 million population. More than half of patients with critical limb ischemia undergo attempts at revascularization as definitive treatment; regardless, significant numbers of patients lose their limbs or die within 1 year. Risk factors for peripheral arterial disease include smoking, diabetes, hypertension, chronic renal insufficiency, African-American race, male sex, hyperlipidemia, and hyperhomocysteinemia. Again, the importance of chronic limb ischemia as a marker for atherosclerotic cardiovascular disease cannot be overstated. The 5-year mortality rate is 30% for patients with claudication and 70% for patients with critical limb ischemia. Etiology and Pathophysiology Peripheral arterial disease most commonly results from atherosclerosis of the distal arterial tree. Patients with intermittent claudication have normal blood flow to the limb at rest; but with exercise, the occlusive arterial disease prevents proper augmentation of blood flow, resulting in insufficient oxygen delivery to the muscles and the symptoms of claudication. Critical limb ischemia represents more advanced occlusive peripheral arterial disease in which oxygen delivery to the lower limb is suboptimal even at rest. Manifestations of Disease Clinical Presentation Intermittent Claudication Patients with intermittent claudication describe fatigue, aching, or cramping in the muscles of the leg that develops after walking a consistent established distance (or other exercise) and that resolves with rest. These symptoms most often appear in the calf but can affect the thigh or buttocks. The anatomic site of pain frequently corresponds to the level of occlusive disease; symptoms typically present in muscle groups one joint level below the region of arterial occlusion. Thus, calf muscle claudication is most commonly due to superficial femoral artery occlusion; hip, thigh, or buttock claudication is most commonly due to more proximal aortoiliac disease. The blood pressure should be measured in both arms and the ankle-brachial index in each leg. The abdomen is palpated in an attempt to detect an abdominal aortic aneurysm as a potential embolic source (although physical examination is only 50% sensitive for abdominal aortic aneurysms 4 to 5 cm in diameter). The peripheral vascular examination comprises palpation of the radial, ulnar, brachial, carotid, femoral, popliteal, dorsalis pedis, and posterior tibial pulses. Auscultation of the carotid, abdominal aorta, and iliac arteries and femoral artery can suggest occlusive vascular disease. In addition, the skin of the legs should be assessed for skin color, temperature, or decreased hair growth and the muscles of the leg for ischemic atrophy. As suggested before, ankle-brachial indices constitute a first diagnostic test in patients thought to have intermittent claudication. First, the systolic blood pressure is measured in each arm, and the higher is taken as the brachial pressure. The cuff is then placed on the calf, inflated, and then slowly deflated; the highest pressure at which the Doppler signal-at either the posterior tibial or dorsalis pedis-becomes audible again marks the ankle pressure. Critical Limb Ischemia Patients with critical limb ischemia present with some combination of ischemic rest pain, nonhealing ulcers, and gangrene. Ischemic rest pain is severe, is intolerable, sometimes improves with lowering of the affected limb (dangling the foot over the edge of the bed), and is responsive only to narcotic analgesics. The pain is often worst at night (when the limb is elevated), sometimes wakes the patient from sleep, and is sometimes transiently relieved by rubbing the foot. Except in cases of diabetic neuropathy and resulting anesthesia of the foot, patients with tissue loss of the lower extremity also often present with pain, localized to the wound. Ulcers and gangrene usually affect the toes, the heel and ankle, and, in severe cases, the distal foot proper. In those patients with critical limb ischemia and diabetes mellitus, the peripheral neuropathy often contributes to the trauma initiating ulcer formation and to the delayed recognition of the wound by the patient. The microvascular derangement of diabetes predisposes to nonhealing of these wounds and to the subsequent development of infection (wet gangrene). Complications of diabetic foot ulcers, including gangrene, are the most common cause of nontraumatic leg, foot, and toe amputation. Up to 15% of diabetic patients will suffer from a foot ulcer during their lives, and 15% to 25% of these will require an amputation at some level.
5mg finast amex
Patients should also be monitored for features of fluid overload such as jugular venous distension hair loss cure news 2012 cheap 5 mg finast overnight delivery, mucous membrane turgor, pulmonary rales, third heart sound and pitting oedema. Central venous pressure monitoring should be considered when there is difficulty assessing intravascular volumes. Invasive direct measures of cardiac output that enable accurate measurement of intravascular filling. Postoperative oliguria is most commonly prerenal and is caused by insufficient fluid replacement. This can be confirmed by a fluid challenge with the infusion of 250 ml of a colloid such as gelofusin over 15 min. If there is no improvement in urine output with the fluid challenge, the patient should be assessed for evidence of pulmonary oedema and renal impairment (due to tubular necrosis). In the elderly or those with known cardiac disease, fluid challenges should be given with caution as this may exacerbate pulmonary oedema. If prerenal and renal causes of oliguria have been excluded, a postrenal aetiology such as ureteric obstruction should be considered. If this is inconclusive, ureteric catheters can be used for diagnosis and treatment. Postoperative monitoring of electrolytes is therefore not required routinely in these patients. In addition, patients with renal impairment, diabetes or those receiving certain medications. These patients should be monitored for electrolyte imbalance and treated promptly for any abnormality. Hyperkalaemia can occur in patients undergoing extensive surgery due to shift of potassium from traumatized cells into the extracellular space. Moderate or severe hyperkalaemia (potassium level >6 mEq/l) is a medical emergency; if not corrected promptly, it can lead to severe cardiac arrhythmias and death. Hyponatraemia is usually secondary to excessive fluid administration or absorption of excessive amounts of irrigating fluid during hysteroscopic surgery, and hypernatraemia is secondary to dehydration. Bladdercare In women undergoing major gynaecological surgery, a urinary catheter is usually inserted just before the operation to keep the bladder empty throughout the procedure. This helps to minimize the risk of bladder injury and allows good access to the surgical field. The catheter should be removed as soon as the patient is able to mobilize and void comfortably. Postoperative voiding difficulty is a common problem in gynaecological surgery, especially following bladder neck operations, and can be due to spasm, oedema or tenderness of parauretheral tissue. It is also common following radical hysterectomy due to extensive perivesical dissection that interferes with the nerve and blood supply to the bladder. Failure to pass urine could also occur as a result of regional anaesthesia (which may cause bladder overdistension and atony) and abdominal pain, which may inhibit the initial voluntary phase of voiding. Following bladder neck surgery, most voiding difficulty resolves within 1 or 2 weeks of surgery, but up to 20% of women can continue with this problem for an extended period (up to 6 months) before being able to void normally (Smith and Cardozo 1997). This should also be performed in women undergoing bladder neck surgery or radical hysterectomy. Voiding difficulty is diagnosed if the residual volume is consistently greater than 100 ml. If this problem persists after several voiding attempts, a catheter should be inserted for 24 h. The catheter is then removed and further residual volume measurements are carried out. Eventually, if voiding difficulty persists, the patient should be trained to perform intermittent self-catheterization. A suprapubic catheter should be considered during surgery in patients expected to have postoperative voiding difficulty. This is followed by measurement of residual urine passing through the suprapubic catheter. Another 117 9 Postoperative care advantage of this catheter is the reduced risk of urinary tract infections compared with the urethral catheter. Drains Although not necessary in the majority of routine gynaecological procedures, drains can be helpful in certain cases. The main indication for placing a drain during gynaecological surgery is surface oozing following extensive pelvic surgery such as adhesiolysis, treatment of extensive endometriosis or complicated hysterectomy. Drainage in these cases is necessary to prevent haematoma formation and to allow early recognition of significant postoperative internal haemorrhage. However, the drain should not be used as a substitute for meticulous intraoperative haemostatesis. Intraperitoneal (pelvic) drains have been associated with an increased incidence of infection, and should only be used when the benefits outweigh the risks. Evidence from recent randomized trials and systematic reviews is against the routine use of drains. A recent large randomized trial of drains compared with no drains following radical hysterectomy and pelvic lymph node dissection concluded that drains can be safely omitted in the absence of excessive bleeding during surgery or oozing at the end of surgery (Franchi et al 2007). A systematic review evaluating the value of routine suction drains after retroperitoneal lymphadenectomy in gynaecological tumours concluded that the prophylactic use of continuous suction drains is associated with a significant increase in morbidity and should be avoided (Bacha et al 2009). On the other hand, drainage of surgical wounds (especially clean-contaminated wounds) using a closed-suction system has been used prophylactically to reduce wound infection (Panici et al 2003). Passive drains, which drain by overflow assisted by gravity, are preferred for the peritoneal cavity, where soft tissue can block the fenestrations of suction drains. Passive drains should not be brought out through the incision, to avoid the risk of wound infection. Suction drains are sealed systems with a vacuum to drain a potential space created by surgery such as the subcutaneous or subfascial space. They are also used to drain lymphatic fluid from the groins after lymphadenectomy. The precise timing for removal of a drain should be determined on an individual basis and depends on the reasons for its insertion. Drains that were placed prophylactically to avoid the accumulation of blood, pus or lymph can usually be removed when drainage is <100 ml in 24 h, usually by 2 or 3 days after surgery. Drains placed for drainage of an abscess should be managed according to the resolution of the condition. In addition, there is evidence that good pain relief can reduce the onset of chronic pain syndromes. Inadequate pain management could lead to reduced deep breathing, causing impaired oxygenation. It can also cause inability to cough and clear lung secretions which may lead to lung atelectasis. The first step in achieving good pain control is preoperative prediction and accurate postoperative assessment of the degree of pain. Such pain is subjective and can vary greatly in severity between patients from almost no pain to very severe pain. There are two main factors determining the degree of postoperative pain: firstly, the nature, extent and site of the surgery; and secondly, factors related to the patient including fear, anxiety and pain threshold. It is therefore important to plan postoperative pain management through consultation between the surgeon and the anaesthetist based on the predicted pain severity.


